Heart failure is a condition in which the heart cannot pump the blood, oxygen, and nutrients needed by the body to the organs with sufficient pressure due to a structural or functional disorder. Although there is a mistaken perception among the public that it means the heart has completely stopped, it is actually a progressive process in which the organ continues to work with reduced efficiency. When heart failure symptoms that affect daily life are correctly analyzed in the early period, the progression of the disease can be controlled to a great extent. Thanks to modern heart failure treatment applied today and especially non-surgical, intravascular interventions performed by an expert interventional cardiologist, patients’ quality of life is dramatically improved. This condition is not a hopeless end, but a chronic process that can be safely managed with current medical approaches.
What Is Heart Failure?
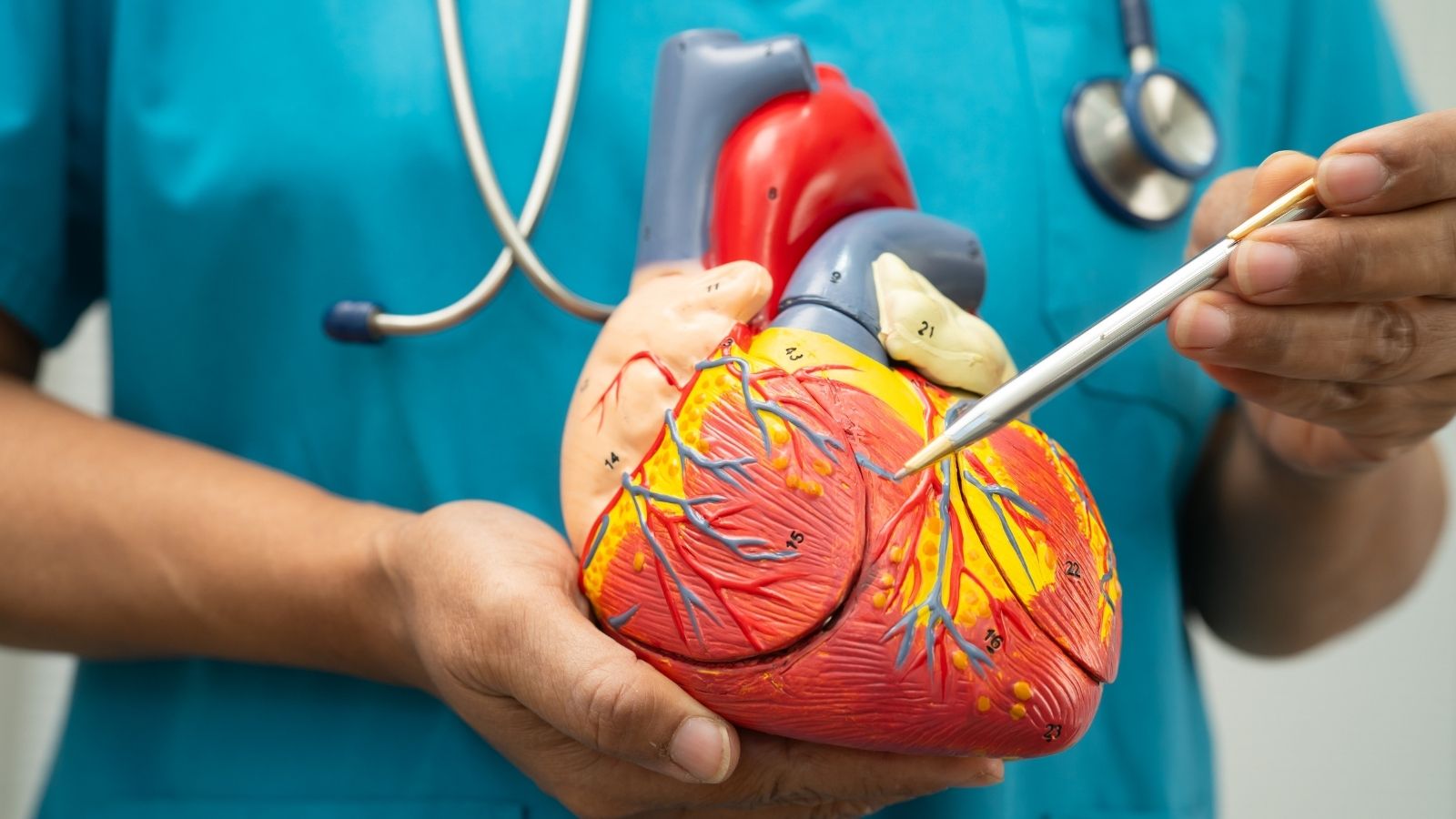
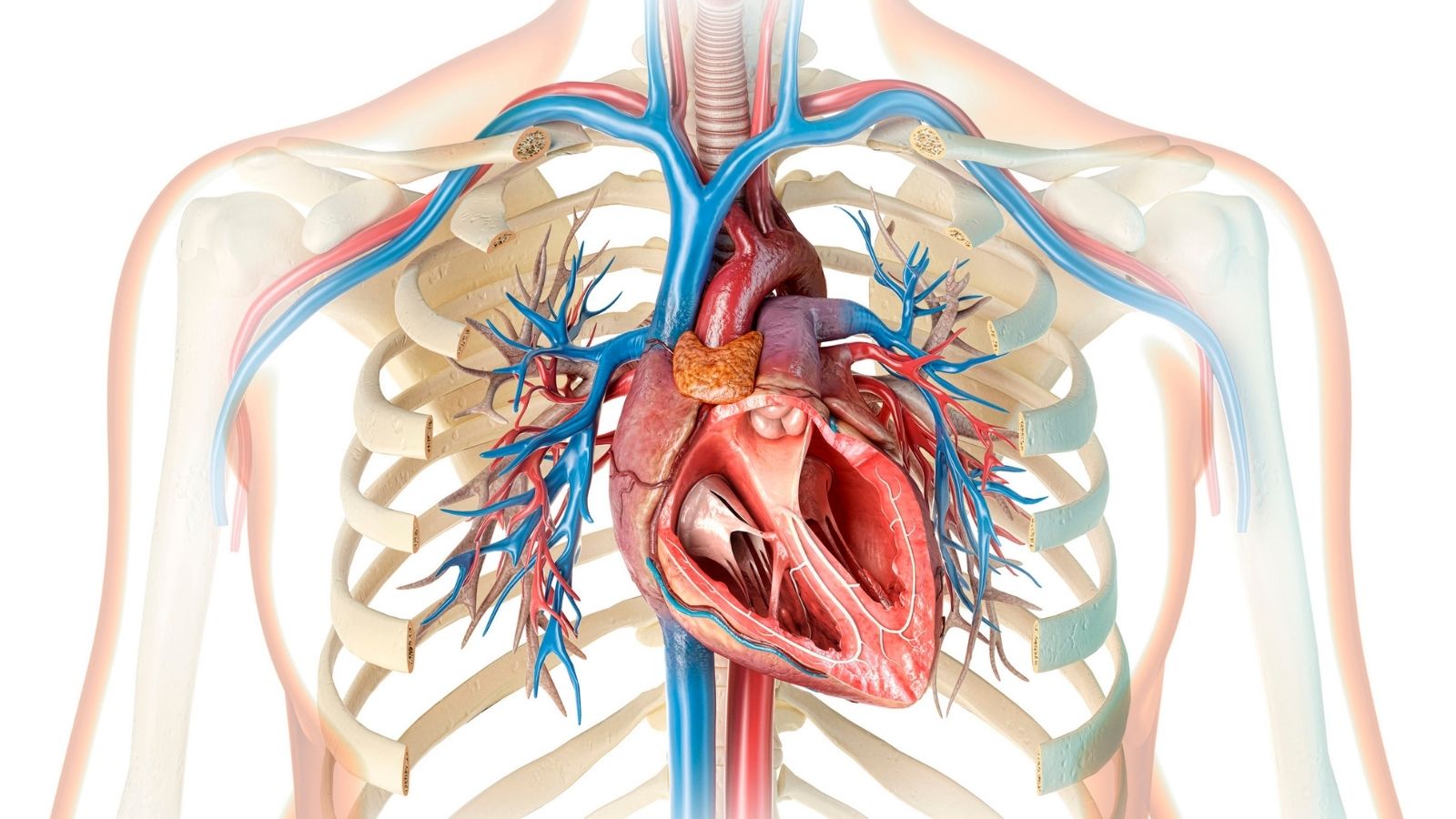
To better understand heart failure, it is quite useful to compare the heart to a gigantic two-chamber pump system that provides pressure to the water system of our home and works continuously without ever stopping. The right side of the heart collects the blood returning from the body in a polluted state and sends it to the lungs to be cleaned. The left side takes the clean, oxygen-washed, nutrient-rich blood from the lungs and pumps it to the entire body, organs, and tissues. If the motor power of this pump weakens over time or if its walls thicken and harden with the fatigue of years and do not allow enough water to fill inside, the balance of this flawless system begins to deteriorate.
Blood that cannot be pushed forward, that is, cannot be sent to the vessels with sufficient pressure, begins to accumulate backward in the system. This accumulation leads to fluid collection in the lungs and various parts of the body, especially in the lower parts due to the effect of gravity. This fluid accumulation, which we call “congestion” in medicine, is the main cause of the complaints experienced by heart failure patients in daily life. Heart failure is the combination of the heart’s reduced performance and the fatigue and blockage sensation created by this fluid accumulated in the vascular system. The body tries to solve this condition by narrowing the vessels to increase pressure or by retaining water through the kidneys to increase blood volume, but these defense mechanisms further increase the load on the heart and make the condition even more difficult to manage.
What Are the Types of Heart Failure?
The most important criterion in diagnosing this disease and determining the correct treatment path is what percentage of the blood inside the heart can be ejected into the body with each beat. This ratio, known in medical language as “Ejection Fraction,” determines the character of the disease. Heart failure is generally divided into main groups.
The clinically accepted types of heart failure are as follows:
- Heart failure with reduced ejection fraction
- Heart failure with preserved ejection fraction
- Heart failure with mildly reduced ejection fraction
The meaning of these classifications is very critical for the patient’s treatment plan. In the group with reduced ejection fraction, the main problem is the significant weakness in the contraction power of the heart. The heart muscle has become tired, thinned, and stretched like a balloon. Its contraction power is far below normal. In the group with preserved ejection fraction, a very different mechanism operates. Here, the contraction power of the heart and the percentage of blood ejected appear completely normal. However, due to reasons such as high blood pressure or aging, the heart muscle has become so stiff and thickened that it cannot relax and stretch. A container that cannot stretch sufficiently cannot fill with enough blood. Because the filling volume decreases, although the pumped ratio appears normal, the amount cannot meet the body’s needs. The third group represents the intermediate form that remains between these two extremes, has transitional characteristics, and may carry symptoms of both groups.
How Do the Stages of Heart Failure Affect Daily Life?
Heart failure is not a surprise condition that appears overnight, but rather a process that progresses silently over years and passes through certain stages. These stages are classified very clearly according to the person’s mobility and exercise capacity in daily life.
At the very beginning of the disease, although some signs of fatigue have structurally begun in the heart, the person does not feel it. There is no limitation in daily physical activities; the person does not experience any unusual complaint even while climbing stairs, running, or doing heavy work. However, when the disease progresses to the next stage, although there is no problem at rest, mild fatigue and shortness of breath begin during ordinary efforts such as brisk walking or daily shopping.
When the disease progresses further, daily life becomes seriously limited. Walking from room to room at home, getting dressed, taking a shower, or climbing a slight slope may cause significant shortness of breath and palpitations. The patient has to stop and rest frequently. In the most advanced and difficult stage, the patient experiences these complaints severely even while completely at rest, lying in bed, or sitting in a chair. At this stage, no physical activity can be performed comfortably, and the person has to spend most of the day lying down or sitting.
What Are the Symptoms of Heart Failure?
Reduced fresh blood flow in the body and excess fluid accumulating backward create very typical symptoms that deeply affect patients’ quality of life. These symptoms may vary depending on which side of the heart is more affected.
The most common symptoms are as follows:
- Shortness of breath
- Waking up at night with a feeling of suffocation
- Swelling in the legs
- Edema in the ankles
- Abdominal bloating
- Getting tired quickly
- Deep weakness
- Dry cough
- Palpitations
- Rapid weight gain
Shortness of breath is especially the result of fluid pooling in the lungs. When the patient lies on their back, the fluid accumulated in the legs and abdomen throughout the day shifts toward the chest cavity and presses on the lungs. Therefore, patients suddenly wake up from sleep at night with shortness of breath and have to sleep with more than one pillow, sometimes even in a sitting position, to breathe comfortably.
Edema is one of the clearest signs that the right side of the heart is tired. When blood begins to accumulate in the veins, fluid first collects in the ankles, then in the legs, and in advanced stages of the disease in the abdominal cavity, also due to the effect of gravity. Because of this excessive fluid retained in the body, patients may suddenly gain two or three kilograms within just a few days. Insufficient oxygen reaching the skeletal muscles creates a constant feeling of fatigue; the person feels so exhausted that they cannot lift their arms and legs. Chronic fluid accumulation in the lungs may also sometimes cause a tickling type of dry cough that increases especially when lying down and does not go away.
Which Methods Are Used for the Diagnosis of Heart Failure?
A wide variety of methods offered by medical technology are used for the correct diagnosis of the disease and to understand the extent of the damage. The process usually begins with a detailed listening to the patient’s complaints and a careful physical examination.
The basic methods used in the diagnostic process are as follows:
- Blood tests
- Chest X-ray
- Electrocardiography
- Echocardiography
- Right heart catheterization
Echocardiography, that is, heart ultrasound, plays a key role in diagnosis. With this method, the wall thicknesses of the heart, the condition of the valves, the width of the chambers, and the pumping percentage of the heart are clearly seen with the help of sound waves. However, especially in advanced-stage patients, when medical treatment is insufficient, and during the decision-making stage for device or valve treatments to be applied, much clearer data are needed.
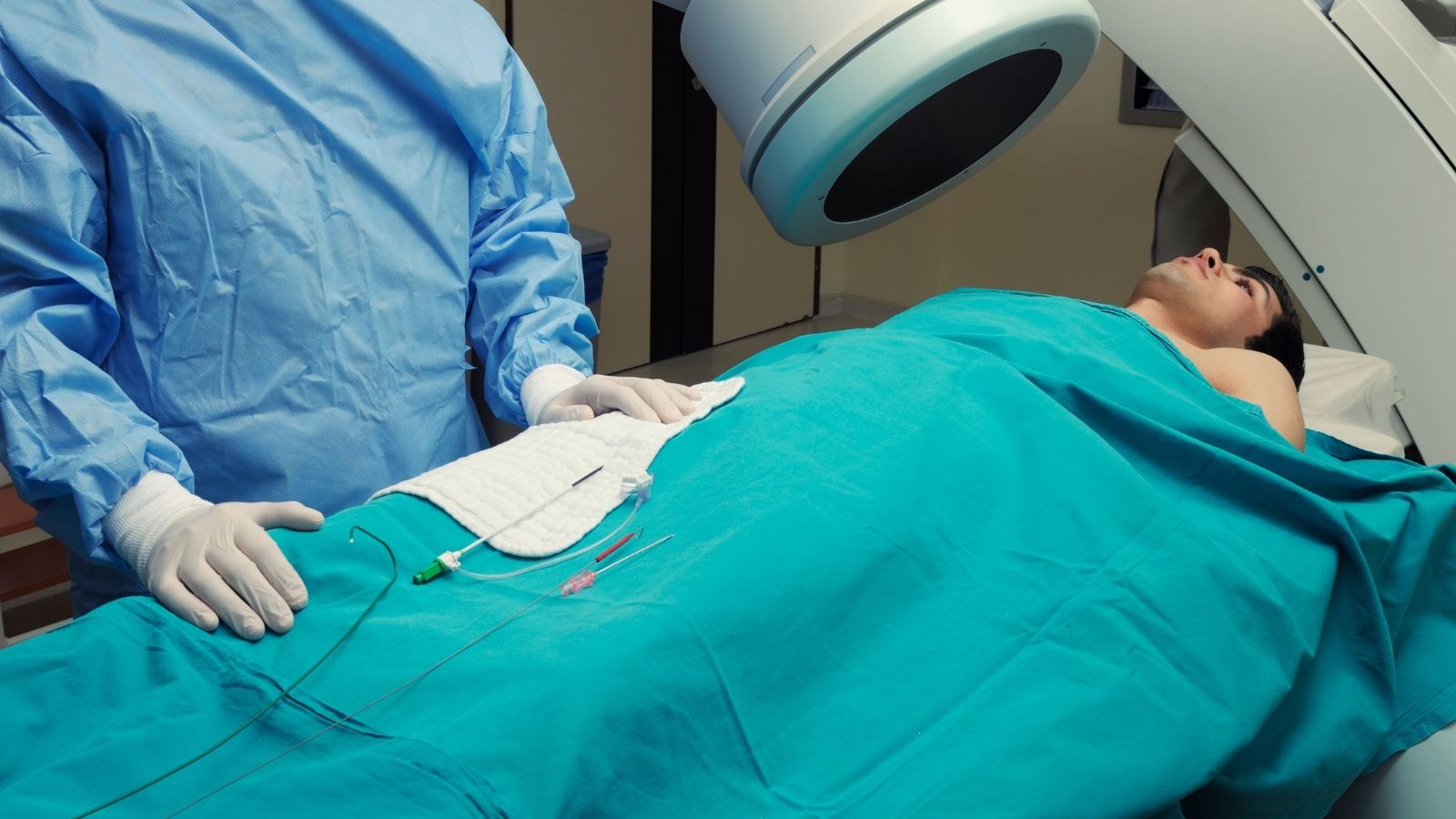
This is where a specialized procedure called “Right Heart Catheterization” comes into play. Usually, with the help of a very thin tube (catheter) as thick as spaghetti pasta, advanced from the wrist or groin area, the right side of the heart and then the lung vessels are reached. In this way, the pressures inside the heart, the resistance of the lung vessels, and how many liters of blood the heart can pump in one minute are measured with millimetric precision. This valuable information is the most important map showing whether the high-tech interventions to be applied to the patient will really work or not.
What Is Done When Medications Are Insufficient in Heart Failure Treatment?
The indisputable foundation of heart failure treatment is lifestyle changes and strong, multidisciplinary medication therapy. Modern medications reduce the heavy burden on the heart, remove excess fluid from the body through the kidneys, dilate the vessels, and slow down the progressive enlargement of the heart. However, when the problem in the heart reaches a mechanical or structural dimension rather than cellular fatigue, medications alone may become helpless.
If the heart valves are torn, narrowed, or if the electrical system inside the heart has completely collapsed, the problem cannot be solved no matter how many medications are used. At this point, interventional cardiology methods come into play and offer incredible opportunities for patients who are not suitable for heart surgery or whose open-heart surgery risk is very high. The greatest advantage of these innovative methods is that they can repair mechanical failures in the heart with special catheter systems advanced only through the vessels, without cutting and opening the patient’s rib cage.
Is There a Non-Surgical Solution for Heart Failure and Mitral Valve Problems?
The mitral valve, located between the left atrium and the left ventricle of the heart, is a two-leaflet door that prevents clean blood from leaking backward. As heart failure progresses, the heart muscle enlarges like a balloon. This enlargement also moves the leaflets of the valve away from each other and causes the valve to become unable to close completely. This condition is called mitral insufficiency. Because of the valve that does not close, with each beat, blood escapes backward toward the lungs instead of moving forward, starting a deadly vicious cycle that makes heart failure much worse.
Special technologies working with a clipping logic have been developed for these patients who are too exhausted to tolerate open-heart surgery. A long delivery tube is sent into the heart by entering through the vein in the groin. While the heart continues to work, the valve leaflets that have moved away from each other and do not close are attached to each other exactly from their middle with the help of a very small, special metal clip. Thus, the enlarged opening is narrowed and the backward leakage of blood is stopped instantly. After the procedure, the load on the heart decreases within seconds and the patient’s shortness of breath decreases dramatically.
Can the Valve Be Replaced Without Opening the Chest in Aortic Stenosis That Causes Heart Failure?
The aortic valve is the main exit door through which clean blood full of oxygen is pumped from the heart to the entire body. With advancing age, this valve may calcify, harden, and become unable to open completely. In this condition, which we call aortic stenosis, the heart has to work against a very great pressure to push blood out through a very narrow hole. This incredible effort causes the heart muscle to thicken excessively over time, become exhausted, and eventually lead to heart failure.
Today, transcatheter methods are used for this difficult condition, whose only solution in the past was open-chest surgery. Usually, the groin artery is entered only with local anesthesia. A brand-new biological valve mounted on a stent is placed directly inside the old valve that has become stone-like from calcification and cannot open. The new valve crushes the old valve, takes its place, and immediately starts working. That enormous wall in front of the heart suddenly disappears. The patient usually returns home walking within a few days.
What Are the New Treatments in Heart Failure and Tricuspid Valve Diseases?
The tricuspid valve, located on the right side of the heart, was a valve that was not intervened much and was neglected in the medical world for many years. However, today we know very well that leakage of this valve plays the leading role in the development of right heart failure and excessive fluid accumulation in the body. The inability of the tricuspid valve to close completely causes blood to reflux toward the liver, kidneys, and legs, disrupting the entire body system.
Special systems similar to clipping technology are also used for the non-surgical solution of this serious problem. Again, by reaching the right side of the heart through the groin vessel, the sagging or separated leaflets of the valve are brought closer together with special clips. Since the backward leakage of blood into the venous system decreases, patients’ stubborn leg edema resolves quickly, the pressure on their liver is relieved, and their exercise capacity increases significantly.
How Are Leaks in Old Valves Eliminated in Heart Failure?
Some mechanical problems may occur over time in patients who underwent open-heart surgery in previous years and received metal or biological prosthetic valves. Even if the valve itself works perfectly, loosening or opening may occur over time in the sutures at the edge areas where the valve is sewn to the heart. The blood leaking from here both causes serious anemia by breaking down red blood cells and leads to severe heart failure findings depending on the amount of leakage.
Taking the patient to open surgery for a second time to repair this leak is, as can be imagined, extremely risky. Instead, with interventional methods, these small leaking holes are reached through the groin vessels with very thin and steerable wires. Tiny special devices resembling umbrellas or plugs are placed into these holes, the opening is completely closed, and the leak is permanently stopped without surgery.
How Is Electrical Dyssynchrony of the Heart Corrected in Heart Failure?
The right and left ventricles of a healthy heart contract at the same millisecond, as a whole, just like synchronized swimmers, thanks to electrical signals. However, in some heart failure patients, this electrical communication network breaks or becomes damaged. The electrical signal reaches the left side of the heart much later than the right side. This causes one side of the heart to contract while the other side is still in the relaxation phase. Instead of squeezing like a pump, the heart begins to move like a cradle swaying from side to side, and its pumping efficiency drops incredibly.
To correct this mechanical dyssynchrony, special three-wire pacemakers are used. The wires coming from a smart generator placed under the skin are positioned on both the right and left outer walls of the heart. The pacemaker sends millisecond electrical impulses to both sides at the same time, allowing the two ventricles of the heart to contract again simultaneously and in complete harmony. In this way, the heart begins to work with high efficiency again, its stretched dimensions shrink over time, and the patient’s quality of life increases extraordinarily.
If Heart Failure Is Not Suitable for Pacemaker Therapy, How Are the Muscles Strengthened?
In a significant portion of heart failure patients, there is no problem in the electrical conduction of the heart; the heart works in a highly synchronized and harmonious way, but the muscle’s own strength is very weak. In these patients, standard three-wire pacemakers that provide synchrony do not work. The brand-new technology developed for these patients is modulation devices that directly affect the contraction strength of the heart muscle.
These devices do not determine the rhythm or speed of the heart like classic pacemakers. Instead, they detect the heart muscle’s natural impulse and send special high-voltage signals from outside at that critical moment when it contracts. These signals do not create an extra heartbeat; however, they affect the chemistry of the heart cell and allow more calcium to enter the cell. This creates a biochemical training effect in the heart muscle. When applied regularly and continuously, the natural contraction strength of the heart muscle increases globally.
What Can Be Done Against the Risk of Sudden Rhythm Disorder in Heart Failure Patients?
The weakening, thinning, and balloon-like enlargement of the heart muscle over time unfortunately greatly increases the risk of fatal rhythm disorders in the heart. The most common cause of sudden losses in heart failure patients is the heart suddenly beating very fast and irregularly, becoming unable to pump blood. In patients whose pumping power has fallen below a certain level, the greatest protection against this insidious danger is pacemakers with shock capability.
These smart devices, after being placed in the patient’s chest, work like an internal emergency team that monitors the heart rhythm continuously 24 hours a day, 7 days a week. The moment they detect a life-threatening, very rapid and chaotic rhythm developing in the heart, they deliver an internal electroshock to the heart within seconds and restore the rhythm to normal. These devices do not treat heart failure itself and do not relieve shortness of breath, but they eliminate the risk of sudden death and enable the patient to hold on to life.
How Is Increased Intracardiac Pressure Balanced in Types of Heart Failure?
Especially in the type of heart failure with preserved ejection fraction, where the heart muscle becomes stiff and thickened, although the pumping power of the heart appears normal, the pressure in the left atrium where blood collects is incredibly high. There is no problem while the patient is sitting calmly, but when they want to walk, climb stairs, or exert effort, this pressure suddenly rises even more. When the pressure increases, blood directly flows backward toward the lungs and creates a severe feeling of suffocation in the person.
To prevent these sudden pressure explosions, small shunt devices are placed in the thin wall between the two atria of the heart. These smart devices allow a small, controlled, and permanent opening to remain between the two chambers. When the pressure on the left side, that is, just behind the lungs, reaches dangerous levels, some of the blood escapes through this hole toward the right side, where the pressure is lower. Thanks to this simple but effective drainage system, the risk of sudden fluid accumulation in the lungs is prevented, and the patient’s shortness of breath complaints in daily life are significantly relieved.
Can Heart Failure Be Treated Through the Nervous System?
Heart failure is not a problem limited only within the borders of the heart; it is a process in which the entire autonomic nervous system also goes into an alarm state. When the heart cannot pump enough blood to the body, our brain perceives this as a vital danger, a bleeding or stress situation. In response, it continuously causes adrenaline to be released into the body. Although this situation accelerates the heart and raises blood pressure in the short term, when it continues for months and years, it exhausts the heart completely by whipping it.
Innovative methods in which a tiny electrode is placed on the carotid artery in the neck are used to break this harmful communication loop. This system continuously sends the message “everything is fine, blood pressure is sufficient, there is no danger” to the brain. When the brain receives this calming stimulus, it turns off the stress system and activates the resting mode. Thus, the vessels relax, the heart rate decreases to reasonable levels, the whipping effect on the heart is removed, and the kidneys relax and expel excess salt and water from the body.
How Is Clot Risk Prevented Without Medication in Heart Failure?
In a fairly large portion of heart failure patients, a rhythm disorder called “Atrial Fibrillation,” in which the atria of the heart cannot contract properly and only tremble, develops over time. In this rhythm disorder, blood flow inside the heart slows down, and blood begins to pool especially in the extension of the left atrium that resembles a blind sac. Slowly flowing blood rapidly clots, and clots formed in this region may break loose and travel to the brain, causing very severe stroke conditions.
To eliminate this risk, patients need to use strong blood-thinning medications for life. However, patients who cannot use these medications due to reasons such as advanced age, a history of stomach bleeding, or risk of falling are under great danger. As a solution to this condition, again by entering through the groin, a tiny umbrella or plug is placed at the opening of this blind sac. This area, where almost all clots form, is completely closed and disabled, and patients are freed from the danger of stroke without having to use high-risk medications.
What Should Heart Failure Patients Pay Attention to in Their Daily Lives?
All these high-tech interventional treatments, excellent surgical methods, or smart devices are doomed to remain incomplete if the patient does not support the process with a good lifestyle and medical follow-up. In the modern medical approach, the most important key to a successful result is for the patient to be an active and conscious part of their own treatment. The daily routines that must be followed in this process are extremely clear.
Very important rules to follow in daily life are as follows:
- Daily weight monitoring
- Restricting salt consumption
- Limiting fluid intake
- Regular and light exercise
- Taking medications exactly on time
- Completely quitting alcohol and smoking
Salt consumption is one of the most critical and most emphasized points. Every excess salt molecule entering the body attracts water like a sponge and holds it in the vessels. This condition incredibly increases the fluid load that the heart has to pump, and excess water quickly leaks into the lungs. With the same logic, the total amount of fluid consumed during the day should not exceed the limits determined by the physician; because a weakened pump has difficulty removing excess water from the body.
The most valuable test that can be done at home is daily weight monitoring. Patients should weigh themselves every morning on an empty stomach, after using the toilet, and with the same clothes. If an increase of more than two kilograms is noticed suddenly within a few days, this does not mean that the person has gained fat, but that the body has started retaining water. This sudden increase is the earliest warning sign that the legs will swell or that a night will be spent waking up with a feeling of suffocation. In such a situation, a physician should be consulted without wasting any time to adjust the treatment plan.

Prof. Dr. Kadriye Orta Kılıçkesmez is one of the leading figures in the field of Turkish cardiology. She was born on January 24, 1974, in Tekirdağ. After completing her undergraduate education at Istanbul University Cerrahpaşa Faculty of Medicine, she chose cardiology as her specialty and received her specialist training at the Cardiology Institute of the same university. In 2015, she was appointed by the university to establish the Şişli Etfal cardiology clinic and Angio laboratory. Becoming a professor in 2017, Kadriye Kılıçkesmez established the cardiology clinic and Angio laboratory of Prof. Dr. Cemil Taşçı Hospital in 2020 and ensured that the clinic became a training clinic.