Coronary artery disease is the insufficient blood and oxygen supply to the heart muscle caused by narrowing of the coronary vessels that feed the heart due to plaque buildup on their inner surface. This chronic process creates life-threatening risks because the heart cannot receive the energy it needs. The main causes of this condition, which often signals itself with typical symptoms such as chest pain, include factors such as genetic predisposition, diabetes, and smoking. Thanks to the invasive and medical treatments offered by modern medicine, vascular blockages can now be opened safely and the progression of the disease can be controlled. Early diagnosis is the most effective way to prevent damage to the heart muscle.
What Is Coronary Artery Disease and How Does It Affect the Working System of Our Heart?
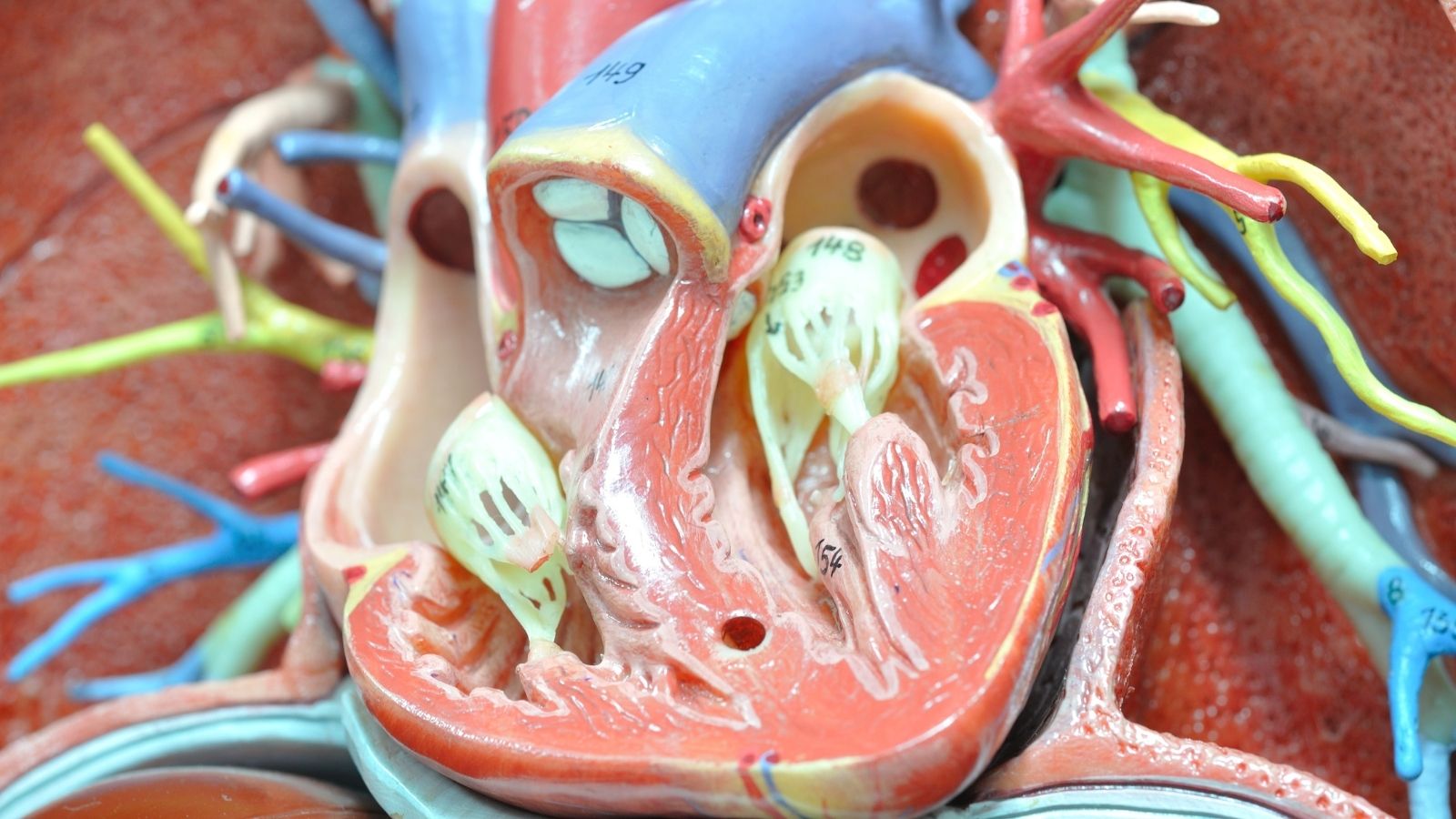
Coronary Artery Disease is the narrowing or complete blockage of the main and side vessels that feed the heart as they lose their elasticity over time. At the basis of the development process of this disease lies a highly complex structural deterioration called atherosclerosis in the medical world and known among the public as vascular stiffness. Vascular stiffness is not a simple and mechanical event such as fat accumulating inside a tube-shaped structure. On the contrary, it is a chronic, insidious, and years-long inflammatory process that begins in the innermost layer of the vessels.
When bad cholesterol particles circulating in the blood begin to leak under the very thin protective membrane called the endothelium, which lines the inner surface of the vessels, the body’s immune system perceives this as a threat. Defense cells immediately rush to this area and try to destroy the cholesterol particles. However, as a result of this struggle, the defense cells swell and take on a foamy structure, becoming trapped inside the vessel wall. As a result of this accumulation continuing for years, even decades, structures called plaques form in the vessel wall. As these plaques grow, they gradually narrow the space through which blood flows. The heart muscle can tolerate this narrowing while at rest and continue its function, even with limited blood flow. However, when the person climbs stairs, runs, or experiences an intense moment of stress, the heart’s working speed increases and it needs much more oxygen. When the narrowed vessel cannot meet this increased oxygen and blood demand, the heart muscle cells remain deprived of oxygen and begin to send alarm signals.
With Which Risk Factors and Physiological Causes Does Coronary Artery Disease Occur?
The development process of the disease is usually not due to a single cause. The vessel structure is damaged as a result of many different metabolic, genetic, and environmental factors interacting with each other over the years. These risk factors are divided into two main categories: factors that the person cannot change through their own efforts and factors that can be controlled through lifestyle changes.
Advanced age, male sex, and a family history of heart disease at an early age are the main risks that a person is born with and cannot be modified. It is known that individuals whose first-degree relatives had vascular blockage at a young age are genetically much more prone to this disease. In addition, unhealthy lifestyle habits and chronic diseases brought by the modern age directly damage the inner vessel structure. For example, high blood pressure damages the protective inner membrane of the vessel through the mechanical stress created by blood constantly hitting the vessel wall with high pressure. Diabetes causes glucose molecules that remain constantly high in the blood to attach to vascular cells, disrupting their normal functions and causing the vessels to become more fragile and calcified. Tobacco use, on the other hand, increases the tendency for clotting in the blood and directly poisons the inner surface of the vessel, accelerating the plaque formation process to an incredible degree.
The main risk factors involved in the development of the disease are as follows:
- Advanced age
- Genetic predisposition
- Diabetes
- High blood pressure
- High cholesterol
- Smoking
- Obesity
- Sedentary lifestyle
- Chronic stress
What Symptoms Does the Body Show in Individuals Who Develop Coronary Artery Disease?
The disease may present with very different symptoms depending on the severity of the narrowing in the vessels and whether the blockage develops suddenly. If the narrowing in the vessel has increased gradually, the body usually begins to give warnings during exertion. In this condition, known as stable chest pain, the person feels a very clear pressure right in the middle of the chest, behind the breastbone, while climbing uphill, carrying a heavy load, or walking against a cold wind. This feeling is usually not like a needle prick, but a dull pain as if a heavy stone has settled on the chest or the rib cage is being compressed. When the patient stops and rests, the heart’s oxygen need decreases, so these complaints completely disappear within five to ten minutes.
However, if the plaque structure inside the vessel suddenly cracks or ruptures, the situation reaches a much more dangerous level. When the plaque ruptures, the substances inside it come into contact with blood, and the body immediately sends clotting cells to that area, creating a plug that completely blocks the vessel. In this picture, called a heart attack, the pain no longer goes away with rest, has no relation to exertion, and may be severe enough to wake the person from sleep. During these minutes when the cells are completely deprived of oxygen, the symptoms are much more intense and frightening. Especially in women and elderly diabetic patients, hidden symptoms such as only extreme fatigue or stomach discomfort may also be seen instead of this classic chest pain.
The main symptoms most commonly experienced by patients are as follows:
- Chest pain
- Shortness of breath
- Palpitations
- Cold sweating
- Nausea
- Dizziness
- Pain spreading to the left arm
- Numbness in the jaw
- A feeling of pressure in the neck
- Extreme fatigue
Which Diagnostic Methods Are Used in Individuals Suspected of Having Coronary Artery Disease?
In a person who presents to the hospital with chest pain or similar complaints, a highly detailed scientific process that progresses step by step is carried out to make the correct diagnosis. The physician’s primary goal is to determine whether the complaints truly originate from the heart and whether damage has occurred in the heart. The first and most basic step is electrocardiography. This device prints the electrical map of the heart on paper and provides the first and fastest clues about whether the heart muscle is receiving enough oxygen. In emergency situations such as a heart attack, electrocardiography enables diagnosis at a life-saving speed.
However, if there is no complete blockage in the vessels and only a partial narrowing exists, the electrocardiography taken while the patient is resting may appear completely normal. At this point, the exercise test comes into play. The patient is made to walk on a treadmill at a certain pace, artificially increasing the workload of the heart, and during this time the electrical waves of the heart are continuously monitored to check whether a hidden state of oxygen deprivation emerges. The echocardiography device uses sound waves to display the heart chambers, the contraction strength of the walls, and the condition of the valves live on the screen. Thanks to this device, a decrease in the contraction ability of a heart muscle region damaged due to vascular blockage can be clearly seen. When necessary, tomographic angiography methods, which map calcification and possible narrowings inside the vessels three-dimensionally in a computer environment, are also frequently used.
How Is the Angiography Procedure Performed in the Definitive Diagnosis of Coronary Artery Disease?
If serious narrowing in the vessels is suspected as a result of preliminary tests, coronary angiography, accepted as the gold standard in the medical literature, is used. Although it is a word that creates considerable concern among the public, modern angiography procedures are performed in an extremely comfortable, fast, and safe manner. Angiography is not an open surgery; it does not require general anesthesia, the patient’s rib cage is not opened, and the patient is fully awake throughout the procedure. Only the entry area is numbed with a small needle, completely eliminating the feeling of pain.
Today, this procedure is mostly performed through the radial artery in the wrist, which is much smaller and safer than the groin vessel. After the wrist is numbed, thin, flexible, plastic, hollow tubes are placed inside the vessel. These tubes are gently advanced together with the blood flow until they reach the entrance of the main vessels of the heart. A special liquid that shines under X-rays is injected through the tubes into the vascular network. While this liquid fills the entire vascular network of the heart within seconds, the device takes consecutive images. Thanks to this moving map reflected on the screen, the location, number, and severity of the narrowings in the vessels are detected with millimetric precision. Diagnostic-only angiography procedures that do not require any intervention are completed in an average of about fifteen minutes, and after procedures performed through the wrist, patients can leave the hospital walking within a few hours and return to their daily lives.
Which Advanced Imaging Technologies Are Used When Making a Treatment Decision in Coronary Artery Disease?
Although angiography provides an excellent map, sometimes it may not be possible to understand by visual inspection alone whether the narrowing seen on the screen is serious enough to leave the heart muscle without oxygen. Especially in moderate narrowings, the inside of the vessel must be examined at the cellular level in order to avoid placing material in the vessel unnecessarily or to avoid overlooking a narrowing that should be taken seriously. At this stage, high-tech intravascular measurement and imaging systems come into play.
In the method called Fractional Flow Reserve, a hair-thin wire with a micro-sized pressure sensor at its tip is passed beyond the narrowing inside the vessel. This sensor measures the pressure of the blood before and after the narrowing and reveals, with a mathematical ratio, how much the narrowing truly obstructs blood flow. If there is no significant drop in pressure, there is no need to intervene in that narrowing, and the patient can be followed with medication. Another miraculous technology is intravascular ultrasonography. With a miniature ultrasound device sent into the vessel, not an externally taken film of the vessel but a direct 360-degree cross-sectional image from inside is obtained. In this way, the structure of the plaque in the vessel wall, the true diameter of the vessel, and the exact dimensions of the material to be placed are calculated with flawless precision. All these technologies raise the success rate of the intervention to the highest level.
How Are Stent and Balloon Applications Performed in the Treatment of Coronary Artery Disease?
If, as a result of angiography and advanced measurement methods, it is decided that the vessel needs to be mechanically opened, the treatment phase is started either in the same session or in a planned manner. This treatment process is generally called percutaneous coronary intervention. The aim of the treatment is not to destroy the plaque inside the vessel, but to crush that plaque, widen the vessel lumen, and return blood flow to its normal course.
The procedure begins by sending a very thin guidewire into the vessel through the angiography catheters. This wire carefully passes through the narrowed area and is fixed beyond the vessel. A very small deflated balloon advanced over the wire is positioned exactly in the center of the narrowing and inflated with high pressure applied from outside. When the balloon inflates, it crushes the plaque on it toward the vessel wall and stretches the vessel, widening it. However, when the balloon is deflated, there is a high possibility that the vessel will shrink again. To prevent this, stents, which are a type of construction scaffold or a very thin metal mesh tube, are used. The stent, mounted on the balloon, is inflated in the same area and embedded firmly into the vessel wall. The metal mesh structure permanently prevents the vessel from collapsing again. Within weeks, the inner surface of the vessel covers this metal with its own cells, turning the stent into a natural part of the body.
The types of stents selected according to vessel structure are as follows:
- Drug-eluting stents
- Bare metal stents
- Fully bioresorbable stents
With Which Special Devices Is Coronary Artery Disease Solved in Advanced and Calcified Vessels?
In the medical world, not every vascular blockage is the same. Because some patients feel no symptoms for years, vessels may become completely blocked, and months or even years may pass after the blockage. In this condition called chronic total occlusion, the inside of the vessel is filled with plaques that have hardened almost like concrete. Classic guidewires cannot pass through this hard tissue. In such complex cases, completely different, special-tipped wires and much more technical strategies are used. Sometimes the blocked area is tried to be opened from behind by advancing in the opposite direction through capillary pathways from the other intact vessels of the heart. These procedures are advanced interventions that take quite a long time and require great patience and experience.
Apart from this, especially in elderly or diabetic individuals, the vessel wall may become stone-like due to excessive calcium accumulation. In these vessels, using only high-pressure balloons may both burst the balloon and cause the vessel to tear. A stent cannot be placed in a stone-like vessel; even if it is placed, it becomes blocked again in a very short time because the stent cannot open fully. In such difficult scenarios, special shaving devices with diamond dust at their tips and rotating at an incredible speed of one hundred and fifty thousand revolutions per minute are used. This drill-like, very thin device turns the calcium inside the vessel into microscopic dust particles and opens a smooth channel so that the stent can be placed flawlessly.
Which Drug Treatments Are Used After Intervention for Coronary Artery Disease?
Opening the vessel with a stent provides immediate relief to the patient, the heart’s oxygen deprivation ends, and the person feels they have regained their health. However, this mechanical repair does not mean that the disease has completely ended. Since vascular stiffness is a cellular problem affecting the entire body, the drug treatment applied after stent placement has life-saving importance. During the adaptation phase of the stent to the body, it is mandatory to use two different blood-thinning medications continuously for months as standard in order to prevent blood from clotting on the metal.
In addition, even if the patient’s cholesterol level appears ideal, highly effective cholesterol-lowering medications are added to the treatment in order to stabilize the other plaques in the vessel wall, dry out the inflammation inside them, and shrink the plaque. Rhythm medications that regulate the heart’s working speed and minimize its oxygen need, thereby resting the heart, also have a very valuable place in the recovery process. Since keeping the patient’s blood pressure at levels that will not tire the vessels is critical in preventing heart enlargement and the development of heart failure, special blood pressure regulators are also among the indispensable parts of this prescription.
The main medication groups that need to be used are as follows:
- Blood thinners
- Cholesterol-lowering medications
- Rhythm regulators
- Blood pressure medications
- Stomach-protective medications
What Should Individuals with Coronary Artery Disease Pay Attention to in Their Diet?
The success of medical and interventional treatments is directly linked to how the patient treats their own body after the procedure. One of the most effective ways to protect vascular health is to change eating habits completely and permanently. Animal-derived saturated fats, trans fats, and processed foods that support plaque formation inside the vessels should be quickly removed from the diet. Instead, a Mediterranean-style diet offered by nature, supporting vascular repair and possessing anti-inflammatory properties, should be adopted.
Whole grains, fresh vegetables, and fruits, which are extremely rich in fiber, greatly contribute to regulating blood values by reducing cholesterol absorption in the intestines. Seafood and plant-based oils containing Omega-3 fatty acids, which preserve the flexibility of the cell membrane, must be at the center of the diet. Salt consumption, one of the most insidious enemies that tire the heart, should be seriously restricted, and natural spices should be preferred instead of salt when flavoring meals. In addition, strictly avoiding simple carbohydrates, sweets, and white flour products that rapidly raise blood sugar and damage the inner vessel membrane is a critical step for successfully maintaining the treatment process.
Foods that should be included in a heart-friendly diet are as follows:
- Extra virgin olive oil
- Salmon
- Raw almonds
- Raw walnuts
- Oatmeal
- Spinach
- Broccoli
- Flaxseed
- Green tea
- Apple
- Garlic
Foods to avoid are as follows.
- Margarine
- Processed meat products
- Fried foods
- Sugary drinks
- Pastries
- White bread
What Should Change in Lifestyle to Stop the Progression of Coronary Artery Disease?
The complement of treatment and the key to lasting success are hidden in the radical changes the patient makes in their lifestyle. A sedentary body leads to slowing of metabolism, deterioration in the quality of blood circulation, and laziness of the vessels. Therefore, it is extremely important to perform regular, moderate-intensity physical activities for at least one hundred and fifty minutes per week, as approved by the physician. Brisk walking, swimming, or light cycling exercises increase the pumping strength of the heart, encourage the formation of new capillary vessels, and lower blood pressure naturally.
In addition, sleep quality and stress management also have very strong effects on heart health. The intense stress brought by daily life causes cortisol and adrenaline hormones to remain constantly high in the body, narrowing the vessels and tiring the heart. Learning to manage stress and getting sufficient and deep sleep gives the body the time it needs to repair damaged cells throughout the night. Habits such as tobacco use, which practically invite a heart attack, must be stopped immediately without excuse. From the first day smoking is stopped, the body enters a major repair process and the risk of clotting begins to decrease rapidly.

Prof. Dr. Kadriye Orta Kılıçkesmez is one of the leading figures in the field of Turkish cardiology. She was born on January 24, 1974, in Tekirdağ. After completing her undergraduate education at Istanbul University Cerrahpaşa Faculty of Medicine, she chose cardiology as her specialty and received her specialist training at the Cardiology Institute of the same university. In 2015, she was appointed by the university to establish the Şişli Etfal cardiology clinic and Angio laboratory. Becoming a professor in 2017, Kadriye Kılıçkesmez established the cardiology clinic and Angio laboratory of Prof. Dr. Cemil Taşçı Hospital in 2020 and ensured that the clinic became a training clinic.