Bradycardia is a rhythm disorder characterized by the heart rate dropping below 60 beats per minute and indicates that the heart is working slower than normal. Although it may be seen physiologically in athletes, in some cases it develops due to problems in the heart conduction system and requires clinical evaluation.
Common symptoms of bradycardia include dizziness, weakness, easy fatigue, shortness of breath, and difficulty concentrating. An insufficient heart rate may reduce the amount of oxygen going to the tissues. This condition may lead to a marked decrease in performance in daily life activities, especially in older individuals.
Serious symptoms that may develop due to bradycardia include fainting, chest pain, and confusion. A significant drop in heart rate may prevent adequate blood supply to the brain and other vital organs. Therefore, cardiological evaluation and rhythm analysis are important in symptomatic cases.
Bradycardia risk factors and causes include heart conduction system diseases, electrolyte imbalances, certain medications, and age-related changes in heart tissue. Electrocardiography, Holter monitoring, and clinical evaluation are used in the diagnostic process; when necessary, permanent pacemaker treatment may be applied.
| What You Need to Know | Information |
| Definition | Bradycardia is the condition in which the heart rate drops below 60 beats per minute. While this condition may be physiological in some individuals, in others it may indicate an underlying health problem. |
| Normal Pulse Range | In healthy adults, the normal resting pulse is generally between 60–100 beats per minute. Bradycardia indicates values below this limit. |
| Physical Bradycardia | Especially in well-trained athletes, the pulse may be low at rest because the heart works more efficiently, and this condition is considered normal. |
| Pathological Bradycardia | It is a type of bradycardia that occurs due to causes such as problems in the heart conduction system, medication use, metabolic disorders, or neurological diseases and requires treatment. |
| Most Common Symptoms | Dizziness, fainting (syncope), weakness, easy fatigue, chest pain, shortness of breath, impaired concentration, and cold sweating. |
| Conditions That Progress Without Symptoms | In some individuals (especially athletes), bradycardia may not cause any symptoms and may be detected incidentally. |
| Risk Factors | Aging, having had a heart attack, degeneration in heart tissue, certain medications (beta blockers, digitalis glycosides), thyroid hormone deficiency, sleep apnea. |
| Diagnostic Methods | ECG (Electrocardiogram), Holter monitor (24-72-hour heart rhythm monitoring), exercise stress test, electrophysiological studies, and blood tests. |
| Emergency Symptoms | Sudden loss of consciousness, severe chest pain, shortness of breath, and prolonged fainting require emergency intervention. |
| Treatment Methods | Depending on the cause, adjustment of medications, treatment of the underlying disease, permanent pacemaker implantation. |
| Prevention Methods | Regular monitoring of medications, lifestyle changes that support heart health, regular health check-ups, and management of risk factors. |
What Is Bradycardia?
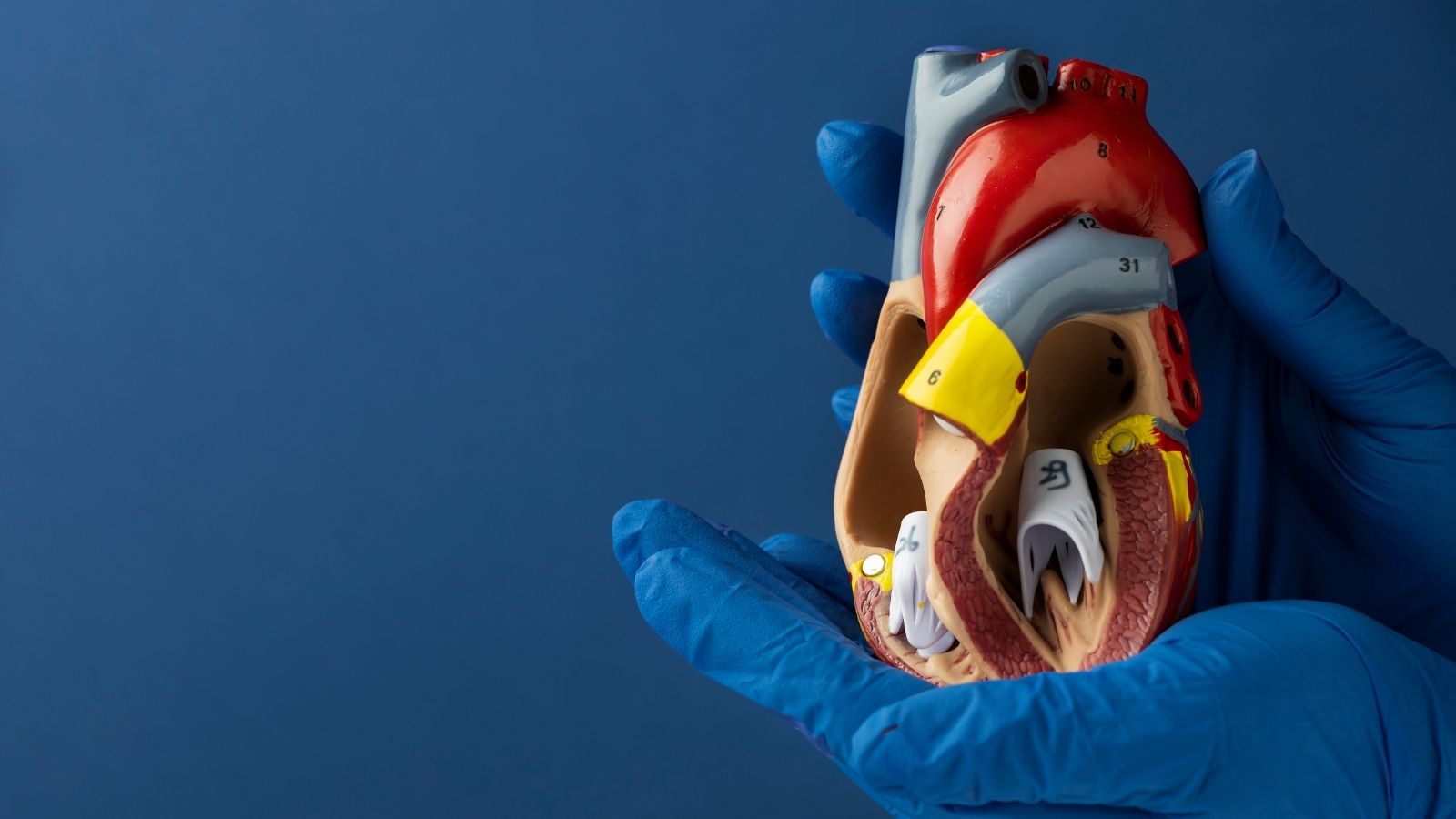
Bradycardia is the condition in which the heart beats at a rate of less than 60 beats per minute. This slowing may occur due to an abnormality in the heart’s electrical system or damage occurring in the heart itself. Simply put, your heart is like a pump, and in bradycardia this pump works more slowly than it should. When this pump, which carries blood to all tissues and organs of the body, slows down, it becomes unable to carry sufficient oxygen and nutrients.
How Does Heart Rate Work?
It is a complex electrical system that regulates the heart rate. This system begins from special cells called the sinoatrial (SA) node, located in the upper chambers of the heart (the atria). The SA node produces electrical impulses at regular intervals. These impulses cause the atria to contract and push blood into the lower chambers of the heart (the ventricles). Then, these impulses reach the atrioventricular (AV) node between the atria and ventricles. The AV node slightly delays the impulses, allowing the ventricles to fill with blood, and then transmits the impulses to the ventricles. This electrical activity causes the ventricles to contract and blood to be pumped to the body. In bradycardia, a disruption occurs in this electrical conduction.
What Is a Normal Heart Rate?
Normal heart rate may vary according to age and general health status. In children, heart rate is usually higher. In adults, the heart rate considered normal at rest is between 60 and 100 beats per minute. However, in people who exercise regularly, such as athletes, the heart rate may be lower, and this condition is usually a healthy adaptation. Bradycardia refers to a heart rate that falls below this normal range.
Different Types of Bradycardia
There are several different types of bradycardia, and these types are generally classified according to the underlying cause and the affected area in the heart’s electrical system:
- Sinus Bradycardia: This is the most common type of bradycardia and occurs when the SA node produces impulses more slowly than normal. It can usually be seen in physiological situations such as sleep, exposure to cold, or use of certain medications. However, in some cases it may also be a sign of an underlying heart disease.
- Subnodal Bradycardia (AV Block): In this type of bradycardia, electrical impulses are produced normally from the SA node, but a slowing or interruption occurs in conduction at the AV node or below the AV node. There are different types according to the degree of this blockage:
First-Degree AV Block: Electrical impulses reach the ventricles, but more slowly than normal. This usually does not cause symptoms.
Second-Degree AV Block: Some electrical impulses cannot reach the ventricles. This condition is divided into two as “Mobitz Type I” (Wenckebach) or “Mobitz Type II.” While Mobitz Type I is generally milder and may not cause symptoms, Mobitz Type II may be more serious and carries a risk of progressing to complete heart block.
Third-Degree AV Block (Complete Heart Block): No electrical impulse can be transmitted from the AV node to the ventricles. In this condition, the ventricles try to produce impulses on their own at a very slow rate, which may lead to severe bradycardia and life-threatening danger.
- Sinoatrial (SA) Pauses: This is the condition in which the SA node temporarily stops producing electrical impulses. This may cause sudden pauses in heartbeats.
The classification of bradycardia helps doctors determine the underlying cause and choose the most appropriate treatment method.
Causes of Bradycardia
Bradycardia may result from various factors that affect the heart’s electrical conduction system. These causes may sometimes be temporary and harmless, while sometimes they may be a sign of a serious underlying disease. Understanding the causes is critically important for correct diagnosis and treatment.
Heart Diseases
Structural or functional disorders occurring in the heart itself are among the most common causes of bradycardia.
- Heart Attack (Myocardial Infarction): Sudden interruption of blood flow to the heart muscle may damage heart muscle cells. This damage may disrupt the electrical system of the heart and lead to bradycardia. Especially during the recovery period after a heart attack, disturbances in the heart’s electrical conduction may be seen.
- Heart Failure: In this condition, in which the heart cannot pump enough blood needed by the body, the heart usually tries to beat faster. However, in some types of heart failure or in advanced cases, the heart rate may slow down due to damage in the heart muscle or problems in electrical conduction.
- Heart Valve Diseases: Narrowing or insufficiency in the heart valves may cause the heart to work harder. In the long term, this condition may cause fatigue in the heart muscle and electrical conduction problems, leading to bradycardia.
- Myocarditis and Pericarditis: Inflammation of the heart muscle (myocarditis) or the membrane surrounding the heart (pericarditis) may disrupt the electrical activity of the heart and lead to bradycardia. These inflammations may occur due to infections, autoimmune diseases, or other unknown causes.
- Congenital Heart Diseases: Some people may be at risk of bradycardia due to congenital heart abnormalities. These abnormalities may affect the electrical system of the heart.
Medications
Many medications may slow the heart rate as a side effect. These medications are among the most common causes of bradycardia, and the problem usually disappears when the medication is stopped or the dose is adjusted.
- Beta Blockers: These medications, used in the treatment of high blood pressure, angina, and heart failure, act by reducing the speed and strength of the heart’s work. Therefore, they are expected to slow the heart rate.
- Calcium Channel Blockers: These medications are also used to lower blood pressure and regulate heart rhythm. They act by slowing the contraction of the heart muscle and electrical conduction.
- Digoxin (Digitalis): This medication, used in the treatment of heart failure and some rhythm disorders, may increase the contraction strength of the heart while also slowing the heart rate.
- Antiarrhythmic Medications: Medications used to treat some rhythm disorders may cause bradycardia when used at the wrong dose or in the wrong patient.
- Opioids: These medications, used as pain relievers, may slow the heart rate by affecting the central nervous system.
- Some Antidepressants and Antipsychotics: Although rarely, some agents in these medication groups may affect heart rate.
Electrolyte Imbalances
Imbalance of electrolytes in the body (minerals such as sodium, potassium, calcium, magnesium) may seriously affect the electrical activity of the heart.
- Hyperkalemia (High Potassium): A potassium level in the blood higher than normal may disrupt the electrical conduction of the heart and lead to bradycardia and even cardiac arrest. It is more common in patients with kidney failure.
- Hypokalemia (Low Potassium): A low potassium level in the blood may also cause heart rhythm disorders.
- Other Electrolyte Disorders: Imbalances in calcium and magnesium levels may also affect heart functions.
Thyroid Problems
The thyroid gland produces hormones that regulate the body’s metabolism. Imbalance of these hormones may also affect heart rate.
- Hypothyroidism (Underactive Thyroid Gland): Deficiency of thyroid hormones slows metabolism, and this usually causes a decrease in heart rate. Hypothyroidism is one of the common causes of sinus bradycardia.
Sleep Apnea
Sleep apnea, defined as repeated stopping or shallowing of breathing during sleep, lowers oxygen levels in the body. This condition may put pressure on the autonomic nervous system, which can cause the heart to beat more slowly. Bradycardia attacks may be seen especially during REM sleep.
Infections and Inflammations
Serious infections in the body (such as sepsis) or inflammatory conditions may disrupt heart functions and lead to bradycardia. The body’s response to infection may slow the heart rate contrary to what is expected.
Brain Damage or Diseases
The brain is an important part of the autonomic nervous system that regulates heart rate.
- Head Trauma: Serious head traumas may disrupt signal transmission in the brain and cause changes in heart rhythm.
- Stroke: Damage in the areas of the brain that control heart rhythm may lead to bradycardia.
- Brain Tumors: Masses in the brain may affect heart functions by putting pressure on nerve pathways.
Autoimmune Diseases
Autoimmune diseases, in which the body’s own immune system mistakenly attacks its own tissues, may target the electrical system of the heart. Diseases such as lupus and rheumatoid arthritis may cause inflammation and conduction disorders in the heart, leading to bradycardia.
Aging
With age, natural changes may occur in the electrical system of the heart. Age-related degenerative processes such as decreased function of the SA node or fibrosis in conduction pathways (scar tissue formation) may cause sinus bradycardia or AV blocks.
Exposure to Extreme Cold
When the body is exposed to extreme cold, it lowers the metabolic rate and slows the heart rate to protect vital organs. This is a survival mechanism.
Bradycardia in Athletes
The heart of athletes who exercise regularly and intensely adapts to work more efficiently. As part of this adaptation, their heart rates at rest may be lower than normal (usually 40-50 beats per minute). This condition is generally a physiological adaptation, not a pathological problem, and is not concerning as long as the athlete’s general health is good. However, bradycardia due to other causes may also develop in athletes.
Unknown Causes (Idiopathic Bradycardia)
In some cases, despite all examinations, the exact cause of bradycardia may not be found. These conditions are called idiopathic bradycardia.
The causes of bradycardia are quite diverse, and doctors try to determine the most likely cause by considering the patient’s medical history, symptoms, and physical examination findings.
Symptoms of Bradycardia
Bradycardia may not always cause obvious symptoms, especially if the heart rate is not too slow or if the person is young and healthy. However, when the heart rate drops significantly or when enough blood is not pumped to the brain and other organs, various symptoms may occur. These symptoms generally result from the body’s lack of oxygen.
- Dizziness and Lightheadedness
One of the most common symptoms when enough oxygenated blood does not reach the brain is dizziness or lightheadedness. This feeling may become more pronounced when suddenly standing up or standing for a long time. The person may feel unsteady or as if “in a void.” This condition may make daily activities dangerous.
- Fainting (Syncope)
When blood flow to the brain drops to critical levels due to bradycardia, the person may experience temporary loss of consciousness. This is called syncope. Fainting usually starts suddenly and lasts briefly. Just before fainting, there may be warning symptoms such as dizziness, nausea, sweating, or visual disturbances. Syncope requires urgent medical evaluation because it may be a sign of a serious underlying condition.
- Fatigue and Weakness
When body tissues cannot receive enough oxygen, a general feeling of fatigue and weakness occurs. The person may feel constantly exhausted and low in energy. Even tasks that are normally done easily become difficult. This condition may significantly reduce the person’s quality of life.
- Shortness of Breath (Dyspnea)
When the heart cannot beat fast enough to meet the body’s oxygen needs, shortness of breath may be felt in order to take more oxygen into the lungs. This condition may become more pronounced especially during exertion or while lying down. The person may have difficulty taking deep breaths or may become breathless.
- Chest Pain (Angina)
When the heart muscle cannot receive enough oxygen, chest pain or a feeling of discomfort may occur. This pain may be in the form of pressure, tightness, or burning and may spread to the arm, neck, or jaw. Chest pain should never be ignored because it may be a sign of a heart attack.
- Difficulty Concentrating and Memory Problems
Decreased oxygen going to the brain may also affect cognitive functions. The person may have difficulty focusing, experience forgetfulness, or feel a slowing in thought processes. This condition may be more pronounced especially in elderly patients and may be confused with dementia.
- Depression and Mood Changes
Chronic fatigue, weakness, and deterioration in general health status may negatively affect the person’s mood over time. Depressive feelings, anxiety, and a general state of unhappiness may occur.
- Cold, Pale Skin
When the body prioritizes blood flow to vital organs, blood flow to the extremities (hands and feet) may decrease. This condition may cause paleness and coldness in the skin.
- Decrease in Exercise Capacity
Physical activities that can normally be done comfortably become difficult due to bradycardia. The person may have difficulty climbing stairs, walking, or exercising and may tire quickly.
- Feeling of Heart Palpitations (Rarely)
Although bradycardia is generally characterized by slowing of the heartbeats, in some cases the heart may beat irregularly. These irregularities may cause the person to feel that their heart is racing or beating irregularly. This may be a sign of an underlying rhythm disorder.
- Timing and Severity of Symptoms
Symptoms of bradycardia may vary greatly from person to person. In some people, symptoms may be mild and intermittent, while in others they may be severe and continuous. The severity of symptoms generally depends on how much the heart rate has dropped and how well the body can tolerate this condition. For example, a person whose heart rate falls below 50 at rest but rises above 60 when active may experience fewer symptoms. However, a person whose heart rate falls below 40 or who has a serious conduction disorder such as AV block will experience more severe symptoms.
- In Which Situations Should a Doctor Be Consulted?
If you are experiencing any of the symptoms above, especially if conditions such as fainting, severe dizziness, shortness of breath, or chest pain are present, it is important to seek medical help immediately. Your doctor will perform the necessary tests to determine the cause of the symptoms and plan appropriate treatment.
Diagnosis of Bradycardia
The diagnosis of bradycardia is made through a combination of the patient’s symptoms, medical history, physical examination findings, and various cardiac tests. The aim is both to confirm that the heart rate is slow and to find the underlying cause of this slowing.
- Medical History and Physical Examination
The doctor first listens to the patient’s complaints in detail. Information such as when symptoms like dizziness, fainting, fatigue, and shortness of breath started, how often they occur, which situations trigger them, and how long they last is important. In addition, the patient’s medications, known heart diseases, thyroid problems, other medical conditions such as diabetes, and family history of heart disease are questioned.
During the physical examination, the doctor evaluates the patient’s general condition, checks the pulse (rate, rhythm, fullness), measures blood pressure, listens to the lungs, and listens to heart sounds. Findings such as skin color and the temperature of the extremities may also provide clues.
- Electrocardiography (ECG)
ECG is a basic test that records the electrical activity of the heart muscle. This test evaluates heart rhythm, heart rate, and electrical conduction in different parts of the heart. It is one of the most important tools for diagnosing bradycardia. ECG may show that heartbeats are below 60 per minute and may also reveal underlying abnormalities such as AV blocks, SA node dysfunction, or heart attack. However, if bradycardia attacks are intermittent, they may not be captured during a standard 12-lead ECG.
- Holter Monitor
A Holter monitor is a portable ECG device and continuously records the patient’s heart rhythm for 24 to 48 hours (sometimes longer) while the patient performs daily activities at home. This is very useful for diagnosing bradycardia, especially in patients whose symptoms occur occasionally. Holter recording allows the doctor to see when the heart rate drops, how long it lasts, and whether this slowing is related to the patient’s symptoms.
- Event Recorder
If symptoms occur less frequently than the coverage period of the Holter monitor, an event recorder may be used. This device is manually activated when the patient feels symptoms and records the heart rhythm for a certain period. Some event recorders can also automatically detect and record abnormal rhythms.
- Exercise Stress Test
Exercise stress testing is the monitoring of heart activity while the patient performs physical exercise, such as walking on a treadmill or cycling. This test is done to see how the heart responds during exercise. Some types of bradycardia (for example, exercise-related bradycardia or some AV blocks) may not be apparent at rest but may appear or worsen during exertion. However, in some cases, instead of triggering bradycardia, the exercise stress test may show that the heart rate increases normally.
- Tilt Table Test
This test is used in patients with recurrent fainting episodes and in whom bradycardia is suspected to be related to the autonomic nervous system. The patient is placed on a table and the table is tilted toward certain angles. This mimics the body’s response to an upright position. During the test, heart rate and blood pressure are continuously monitored. In some patients, during the transition to this position, the heart rate may suddenly drop and fainting may be triggered (vasovagal syncope or neurocardiogenic syncope).
- Cardiac Magnetic Resonance Imaging (Cardiac MRI)
Cardiac MRI uses powerful magnetic fields and radio waves to image the structure and function of the heart in detail. This method has begun to be used more in recent years and may be used to detect damage, inflammation, scar tissue, or congenital abnormalities in the heart muscle. These findings may help understand the structural causes underlying bradycardia.
- Echocardiography (ECHO)
Echocardiography is a test that evaluates the structure, dimensions, wall movements, and valve functions of the heart using ultrasound waves. It is used to identify structural problems that may cause bradycardia, such as weakness of the heart muscle, valve problems, or abnormalities in the heart chambers.
- Blood Tests
Blood tests are important in investigating metabolic or hormonal causes of bradycardia.
Electrolyte Panel: Checks potassium, sodium, calcium, and magnesium levels. Hyperkalemia in particular may be a serious cause of bradycardia.
Thyroid Function Tests: TSH, T3, and T4 levels evaluate the activity of the thyroid gland. Hypothyroidism is a common cause of bradycardia.
Kidney Function Tests: Checks whether the kidneys are working properly, because kidney failure may lead to electrolyte imbalances.
Cardiac Biomarkers: If a heart attack is suspected, enzymes such as troponin may be measured.
- Cardiac Catheterization and Coronary Angiography
If coronary artery disease is suspected, coronary angiography may be performed. In this procedure, a catheter (a thin, flexible tube) is directed to the heart through a blood vessel (usually from the groin), and contrast material is injected into the coronary arteries. This substance makes narrowing or blockages in the vessels visible under X-rays. This test is used to identify problems that may block blood flow to the heart muscle and therefore affect the electrical system of the heart.
- Evaluation of Medications
The doctor carefully reviews all medications used by the patient. If bradycardia has occurred as a side effect of a certain medication, the doctor may recommend changing the medication, adjusting the dose, or completely stopping the medication. This process must be carried out under medical supervision.
The diagnostic process may vary according to the patient’s specific condition. The doctor will decide which tests are necessary to make the most accurate diagnosis.
Management and Treatment of Bradycardia
Treatment of bradycardia varies depending on the underlying cause, the severity of symptoms, and how much the heart rate has slowed. While treatment may not be required in some cases, emergency intervention and long-term management may be necessary in others.
Treatment of the Underlying Cause
If bradycardia is caused by a treatable reason, the priority is to eliminate this cause.
- Medication Adjustment: If there are medications causing bradycardia, the doctor may reduce the dose of the medication, switch to another medication, or stop the medication. This is especially valid for medications that slow the heart rate, such as beta blockers, calcium channel blockers, or digoxin.
- Correction of Electrolyte Balance: If electrolyte imbalances such as hyperkalemia are present, methods such as dietary changes, medications, or dialysis may be used to restore potassium levels to normal.
- Thyroid Hormone Therapy: If bradycardia has developed due to hypothyroidism, the heart rate can be restored to normal with thyroid hormone replacement therapy.
- Sleep Apnea Treatment: In patients with sleep apnea, use of a CPAP (Continuous Positive Airway Pressure) device or other treatment methods may reduce bradycardia attacks during sleep.
- Infection Treatment: In bradycardia due to infection, it is important to control the infection with appropriate antibiotic or antiviral treatment.
- Management of Heart Diseases: Specific treatments are applied for underlying heart conditions such as heart failure, post-heart attack conditions, or heart valve diseases.
Pacemaker Implantation
If bradycardia causes serious symptoms, if the underlying cause cannot be treated, or if there is permanent damage in the electrical conduction of the heart, the most effective treatment method is insertion of a pacemaker. A pacemaker is a small device and is usually surgically placed under the collarbone. The device’s wires (electrodes) are placed inside the heart, monitoring the heart’s electrical activity and sending electrical impulses to speed up the heartbeats when necessary.
- Temporary Pacemaker: In some cases, for example after heart surgery or during an acute heart attack, a temporary pacemaker may be used. These pacemakers work with the help of a wire placed into the heart through a vein and are usually removed within a few days or weeks, if the problem has ended, or replaced with a permanent pacemaker if it continues.
- Permanent Pacemaker: Permanent pacemakers are used in cases of permanent bradycardia. These pacemakers can last for years and significantly improve the patient’s quality of life. There are different types of permanent pacemakers:
Single-Chamber Pacemaker: Only one electrode is used (usually placed in the right ventricle). Dual-Chamber Pacemaker: Two electrodes are used (one in the atrium, the other in the ventricle). This better mimics the heart’s natural coordination. * Biventricular Pacemaker (CRT – Cardiac Resynchronization Therapy): Three electrodes are used (one in the atrium, two in the ventricles). This device is used in patients with heart failure whose heart contractions are not synchronized. It relieves symptoms by enabling the heart to contract more effectively.
Pacemaker insertion is generally a low-risk procedure, but as with every surgical procedure, risks such as infection, bleeding, or electrode problems exist. After pacemaker insertion, patients may need to attend regular doctor check-ups and comply with some activity restrictions.
Lifestyle Changes
In some cases, lifestyle changes may help with the management of bradycardia.
- Healthy Nutrition: A balanced and nutritious diet supports general heart health.
- Regular Exercise: Regular exercise at the level recommended by the doctor may strengthen heart functions. However, patients who experience symptoms during exercise should be careful.
- Stress Management: Stress may affect heart rhythm. Stress reduction techniques (such as meditation and yoga) may be beneficial.
- Alcohol and Smoking: Limiting alcohol consumption and quitting smoking are important for heart health.
- Adequate Fluid Intake: Dehydration may affect heart rate.
Risks of Untreated Bradycardia
When bradycardia is not treated, it may lead to serious health problems because sufficient oxygen does not reach the brain and other organs. These include sudden fainting, injuries due to falls, loss of control while driving, memory problems, progression of heart failure, and even risk of sudden cardiac death. Therefore, it is recommended that people experiencing symptoms of bradycardia consult a cardiology specialist.
The treatment plan is determined individually for each patient and should be applied in line with the doctor’s recommendations.
Frequently Asked Questions
In which situations does bradycardia become dangerous and which pulse value is risky?
Bradycardia is generally defined as the heart rate falling below 60 per minute; however, especially values below 40 are considered dangerous if they are accompanied by dizziness, fainting, or shortness of breath. In this case, the heart cannot pump enough blood and urgent evaluation may be required.
With which complaints does bradycardia appear in daily life?
The most common symptoms in people with bradycardia are fatigue, dizziness, weakness, easy fatigue during exercise, and sometimes fainting. When the pulse slows too much, blood flow to the brain decreases and difficulty concentrating or blurred vision may develop.
How is a low pulse seen in athletes distinguished from pathological bradycardia?
In athletes who exercise regularly, the heart works more efficiently, so the resting pulse may be low. However, athlete bradycardia usually does not cause symptoms. If dizziness, fainting, or shortness of breath is present, this condition may indicate pathological bradycardia.
Which heart diseases or conduction system problems lead to bradycardia?
Sinus node disease, heart blocks, heart muscle diseases, and conduction system damage that occurs after a heart attack may cause bradycardia. In these conditions, the electrical signals of the heart are not transmitted properly and the heart rate slows significantly.
Which medications can cause the pulse to slow dangerously?
Beta blockers, some blood pressure medications, heart rhythm regulators, and some sedative medications may lower heart rate. Especially in elderly people or those with heart disease, these medications may lead to bradycardia and dose adjustment may be required.
Why does bradycardia become more common with advancing age?
As age advances, the electrical conduction system of the heart may naturally weaken. Decreased sinus node function or development of heart blocks causes the pulse to slow in elderly individuals, and this condition may sometimes require a permanent pacemaker.
Can bradycardia cause fainting and why does this occur?
Yes, bradycardia can lead to fainting. When the heart beats too slowly, enough blood and oxygen cannot reach the brain. This condition may cause short-term loss of consciousness and increases the risk of falls and injury, especially when it develops suddenly.
Which tests are performed for the diagnosis of bradycardia?
Electrocardiography (ECG), 24-hour Holter rhythm recording, and sometimes an exercise stress test are used for diagnosis. These tests evaluate the heart rhythm in detail and help determine whether the slowing of the pulse is temporary or a permanent rhythm disorder.
In which situations is a pacemaker required in bradycardia treatment?
A pacemaker may be recommended in cases that cause symptoms and where the heart rate is dangerously low. The pacemaker regulates the electrical impulses of the heart, ensures that the pulse remains at a safe level, and reduces complaints such as fainting and fatigue.
How does bradycardia affect quality of life and how is recovery after treatment?
Marked bradycardia may lead to easy fatigue, dizziness, and exercise intolerance in daily activities. After appropriate treatment, medication adjustment, or pacemaker application, energy levels increase in most patients and quality of life improves significantly.

Prof. Dr. Kadriye Orta Kılıçkesmez is one of the leading figures in the field of Turkish cardiology. She was born on January 24, 1974, in Tekirdağ. After completing her undergraduate education at Istanbul University Cerrahpaşa Faculty of Medicine, she chose cardiology as her specialty and received her specialist training at the Cardiology Institute of the same university. In 2015, she was appointed by the university to establish the Şişli Etfal cardiology clinic and Angio laboratory. Becoming a professor in 2017, Kadriye Kılıçkesmez established the cardiology clinic and Angio laboratory of Prof. Dr. Cemil Taşçı Hospital in 2020 and ensured that the clinic became a training clinic.