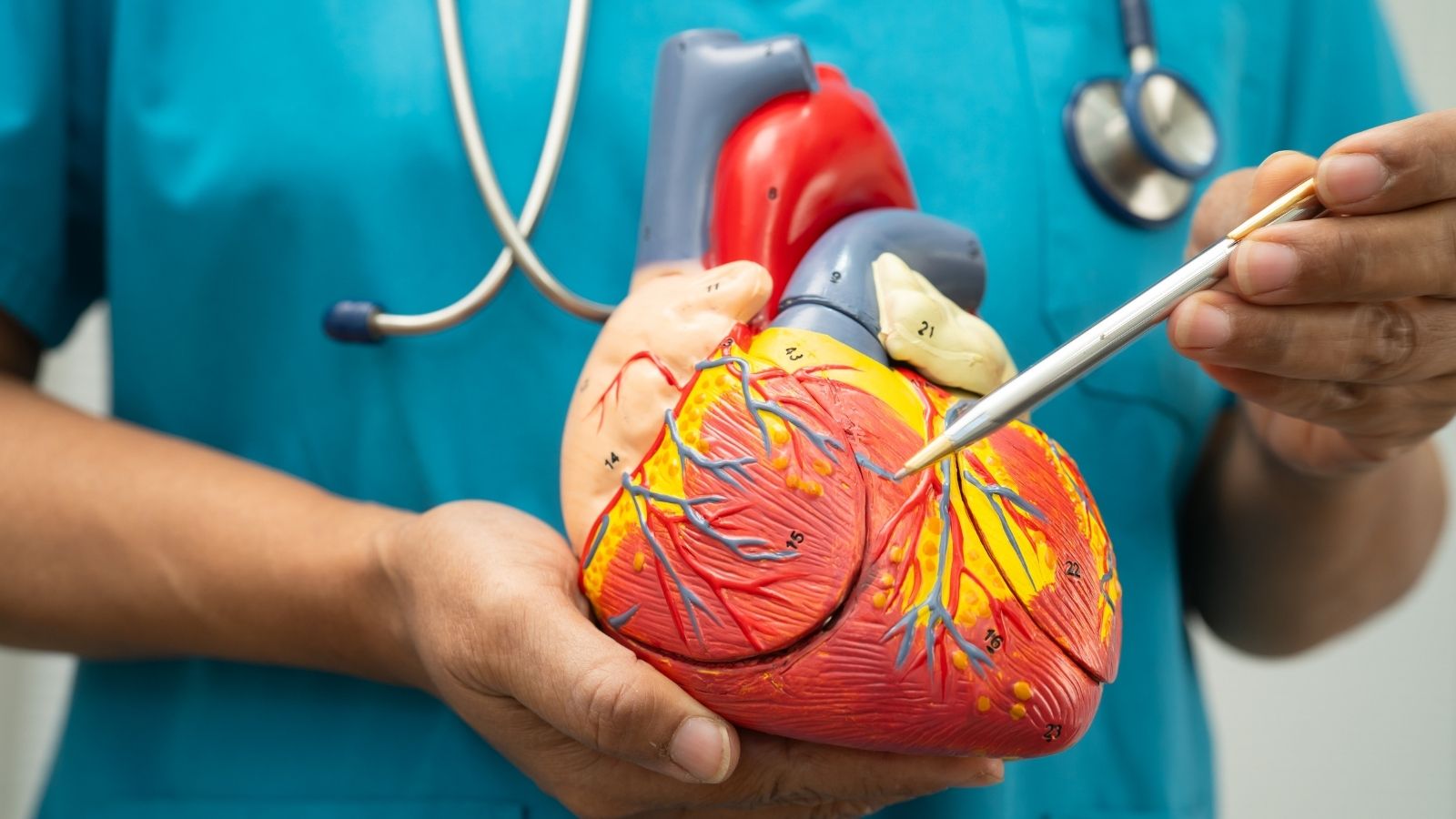
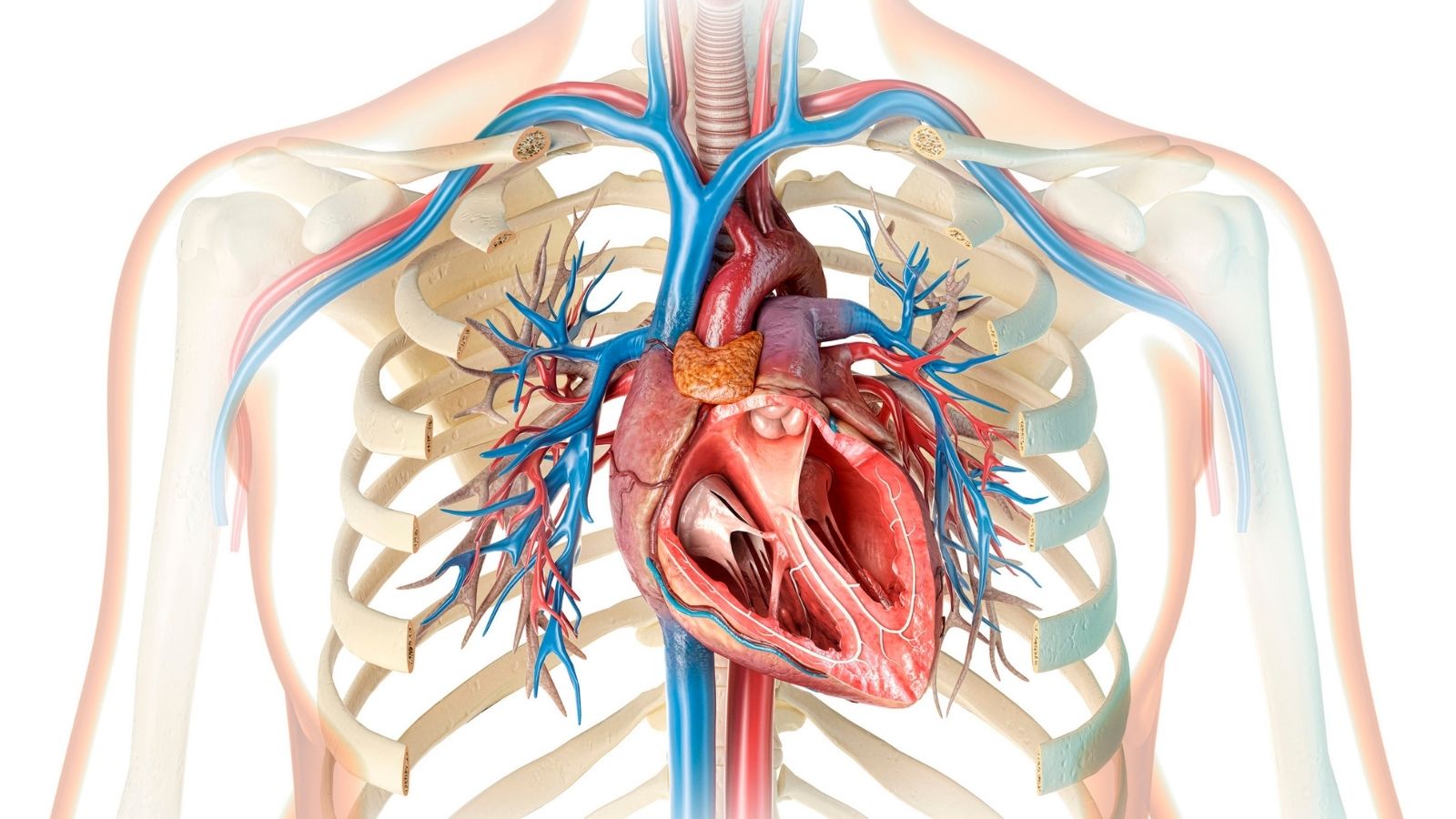
Cardiac examination is a detailed health check that evaluates the muscle structure of the heart, valve functions, vascular network, and working rhythm, enabling possible cardiovascular diseases to be diagnosed at an early stage. This process begins with the physician carefully examining the general body signals and proceeds step by step with technological measurements determined according to individual needs. This method, applied to find the main source of complaints such as pressure felt in the chest area, unexplained fatigue, or shortness of breath, clearly maps the heart’s instant performance. Regular cardiological evaluations are the most vital step for preserving quality of life and safely resolving silently progressing problems before they reach dangerous dimensions.
What Signals Does Our Body Give Us Before a Cardiac Examination?
When the heart starts to have problems, it usually does not remain silent; it calls for help through different parts of the body. The evaluation process begins the very second the person steps inside. The pace of the person’s walk, whether they have enough breath while speaking, or the general expression of fatigue on their face actually tells a lot. When the blood in our body cannot carry sufficient oxygen to the tissues, a bluish color change may occur in the skin color, especially on the lips and fingertips. This condition is called cyanosis and is a very clear indicator that the oxygen level has dropped.
In addition, when the heart cannot pump blood strongly enough, fluid begins to pool in the lower parts of the body. As a result of this pooling, visible swelling occurs especially in the ankles and legs, also with the effect of gravity. This condition, called edema, may indicate that the pumping power of the heart has weakened. In addition, small yellowish fatty deposits appearing around the eyelids may be a clue that the amount of cholesterol circulating in the blood is very high. Some basic warning signs that can be observed are as follows:
- Chest pain
- Palpitations
- Shortness of breath
- Getting tired quickly
- Swelling in the legs
- Bluish discoloration of the lips
Why Are Blood Pressure and Pulse Values Important During a Cardiac Examination?
To understand whether a machine is working properly, it is necessary to look at its pressure gauges. In the human body, these indicators are blood pressure and pulse. Blood pressure refers to the internal pressure created when the heart pumps blood into the vessels. When this pressure remains continuously high, it causes damage over time to the inner surface of the pipe system, that is, the vessels. When blood pressure is measured from both arms, pressure differences between the arms may reveal a possible enlargement or blockage in the main vessels at an early stage.
Pulse shows how many times the heart beats per minute and whether these beats are regular. Those rhythmic beats felt when the fingertips gently touch the vessel are one of the most basic reflections of the heart’s health status. The fullness of the vessels and the speed of the rhythm contain very important information. The main points where pulse is checked in the body are as follows:
- Neck
- Wrist
- Groin
- Top of the foot
What Does the Stethoscope Tell Us During a Cardiac Examination?
The stethoscope, one of the best-known and most classic symbols of medicine, is a bridge that carries the sounds coming from inside the heart to the outside. In a normal and healthy heart, the opening and closing sounds of the valves are heard very clearly and rhythmically as “lub-dub.” These sounds show that the doors regulating the flow of blood between the chambers are working properly.
However, sometimes these doors become calcified, narrowed, or fail to close and begin to leak blood backward. As blood passes with difficulty through these defective doors or narrowed areas, it creates turbulence. This condition, which resembles the rustling sound water makes while passing through a narrow pipe, is called a “murmur.” Hearing a murmur directly indicates a mechanical problem in the internal structure of the heart. The area where the sound is heard and its intensity reveal with great accuracy which valve the problem is in. The main valves listened to in the human heart are as follows:
- Aortic valve
- Mitral valve
- Tricuspid valve
- Pulmonary valve
How Do ECG and Rhythm Holter Work During the Cardiac Examination Stage?
What enables the heart to contract is the small electrical currents it produces within itself. Electrocardiography, commonly known as ECG, records these electrical currents as waves on paper through small electrodes placed on the chest, arms, and legs. ECG recording takes only seconds, is completely painless, and instantly shows whether the heart muscle is receiving enough oxygen or whether there is a rhythm disorder.
Rhythm Holter devices may be used to capture these irregularities that suddenly appear and disappear over time. This device, about the size of a mobile phone, stays on the person for twenty-four or forty-eight hours and records every single heartbeat in its memory. Afterwards, these recordings are examined on a computer, and what type of rhythm disorder occurred at what time of the day is identified.
What Is Echocardiography (Heart Ultrasound) Within the Scope of Cardiac Examination?
When the sounds heard with a stethoscope and the electrical waves on the ECG need to be converted into visual data, echocardiography, in other words heart ultrasound, is used. This method works entirely with sound waves, contains no radiation, and is extremely safe. Sound waves sent through the chest wall hit the walls, valves, and chambers of the heart and return. These returns create a moving video image on the screen.
Thanks to these moving images, the contraction power of the heart is measured clearly. If one part of the heart contracts more sluggishly than the others, this raises suspicion that there may be a blockage in the vessel feeding that area. Sometimes, because of the structure of the rib cage or to see the rearmost parts of the heart more clearly, a thin tube may be lowered through the esophagus to obtain much closer and higher-resolution images. These detailed images serve as a vital guide, especially in cases where heart valves will be treated without surgery.
Who Is Virtual Angiography Performed on After a Cardiac Examination?
In individuals who do not have typical chest pain but have very high risk factors, an easier screening test may be preferred instead of performing classic coronary angiography. Coronary Computed Tomography Angiography, popularly known as virtual angiography, is a method that can be used in these situations. Only a colored liquid is given through a normal vein in the arm, and with the help of advanced tomography devices, a three-dimensional map of the heart is created within seconds.
This method not only shows whether there is a structural blockage in the vessels, but also calculates the amount of calcification in the vessel walls. The calcification score is a very valuable piece of data in predicting a person’s future risk of developing coronary artery disease. If virtual angiography shows that the vessels are completely open, the patient is safely sent home; if a suspicious condition is detected, more advanced procedures are started.
How Is Coronary Angiography, One of the Interventional Cardiology Procedures, Performed?
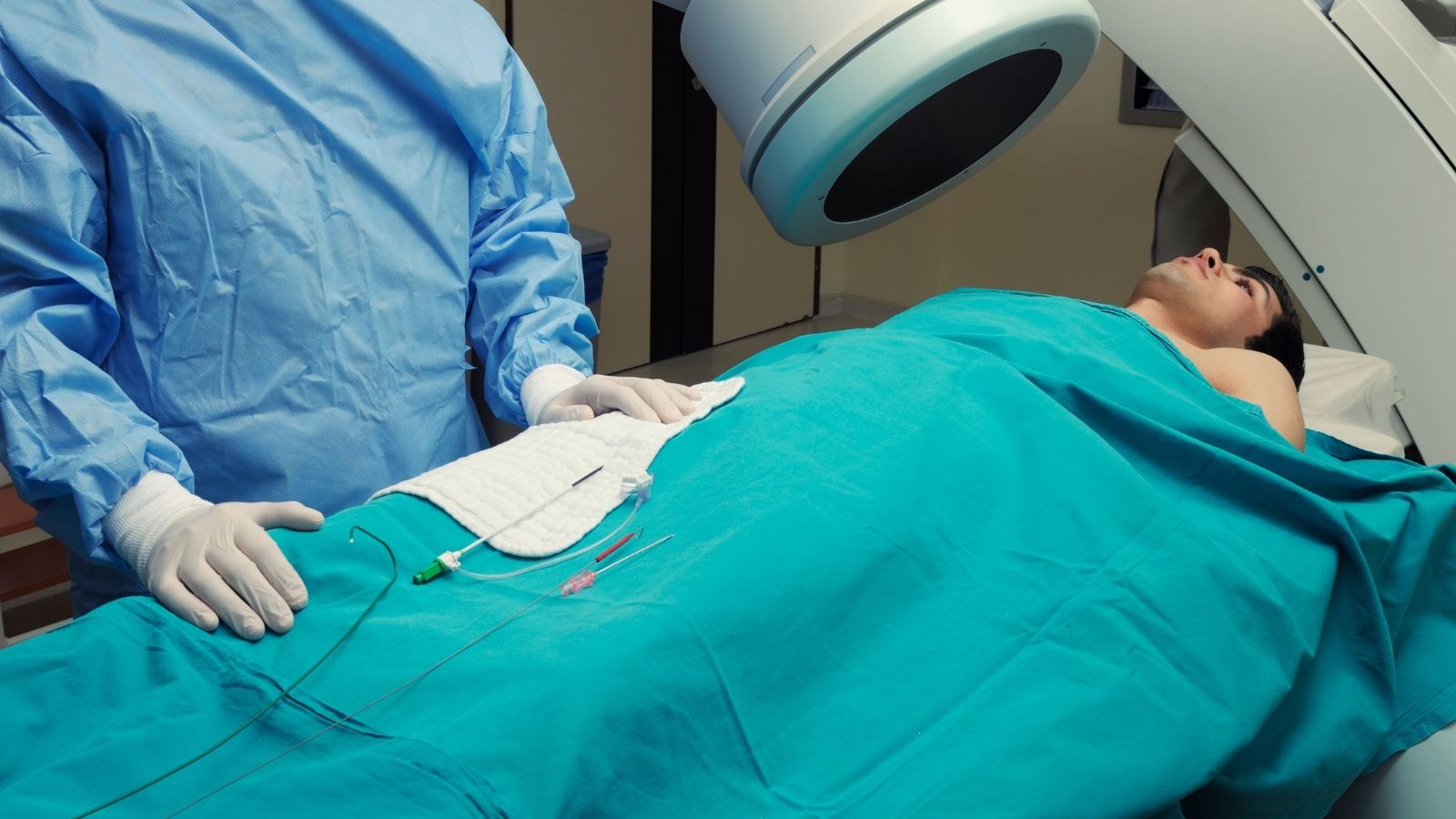
If externally performed tests indicate that there is a serious blockage in the vessels, coronary angiography, the most definitive and clear stage of diagnosis, is performed. This procedure is not a surgery; it does not require general anesthesia, and the patient is fully awake throughout the procedure. Only the area where entry will be made is numbed with local anesthesia. In past years, this procedure was performed only through the artery in the groin. However, today, the artery in the wrist is frequently preferred to increase patient comfort and minimize the risk of bleeding.
Very thin, flexible, hollow plastic tubes are sent inside through the small vessel in the wrist. Since the inside of the vessels does not have pain nerves, the person does not feel the progress of these tubes. When the tip of the tubes reaches the beginning of the coronary vessels feeding the heart, a special dyed liquid called contrast is given inside. This liquid allows the inside of the vessels to appear like a black-and-white tree branch under the X-ray device. If there is an interruption, narrowing, or complete blockage in blood flow, this condition appears in detail on the screen within seconds.
Why Are Advanced Imaging Technologies Needed During Interventional Cardiology?
When looked at visually, a narrowing in the vessel may appear very serious, but sometimes this narrowing does not affect blood flow that much. Or, on the contrary, a calcified plaque that looks innocent from the outside may actually seriously threaten the vessel. To avoid placing a metal stent unnecessarily or to reveal hidden dangers, it is necessary to enter directly into the vessel and make much more precise measurements.
For this purpose, special devices as thin as a strand of hair are used. Systems that measure blood pressure before and after the narrowing inside the vessel decide with mathematical certainty whether that narrowing really needs to be treated. In addition, thanks to tiny ultrasound cameras sent into the vessel, the structure of the vessel wall is examined millimeter by millimeter. Thanks to these microscopic examinations, the content of the plaque blocking the vessel is understood. The following substances are usually found inside plaques:
- Calcium
- Cholesterol
- Connective tissue cells
How Do Stent and Balloon Treatment Work in Interventional Cardiology Applications?
If a serious narrowing that endangers blood flow is detected in a part of the vessel during angiography, the treatment stage is started at the same time. The most common method used to widen the narrowed pipe from the inside is balloon and stent application. First, a long thin balloon in a deflated state is advanced to the point where the narrowing is located. When it reaches the correct point, the balloon is inflated with high pressure. This inflation movement crushes the calcified and fatty mass blocking the vessel toward the vessel wall and opens a tunnel through which blood can pass.
However, vessels have an elastic structure, and when they are opened only with a balloon, they tend to collapse inward and narrow again after a short time. To prevent this, specially designed metal cages called stents are placed in that area opened with the balloon. The stent supports the vessel wall from the inside like a scaffold and keeps it open. The stents used today are drug-coated; that is, by slowly releasing medication from their surfaces, they prevent the body from perceiving that metal as a foreign substance and covering it again with tissue. Sometimes the calcification is so hard that it cannot be crushed with a balloon. In these cases, that calcification is broken with microscopic drills and turned into powder, and after the vessel is cleaned, the stent is placed. The main materials used in stent production are as follows:
- Titanium
- Stainless steel
- Cobalt
- Chromium
Is Non-Surgical Heart Valve Replacement (TAVI) Possible with Interventional Cardiology?
The aortic valve is the last and largest door through which purified blood exits the heart to be distributed throughout the body. As age advances, this valve wears out, becomes calcified, and becomes unable to open and close comfortably like a door. In the past, the only solution to replace this valve was difficult open-heart surgery in which the chest cavity was completely cut open. For elderly people or people with other diseases, the risk of this surgery was very high, and unfortunately many patients remained untreated.
The TAVI method, one of the most tremendous developments offered by technology, has completely changed this situation. Now, without opening the chest cavity at all, entry is made through the vessel in the groin just like performing angiography. A new valve made of biological material, folded at the tip of a catheter as thick as a pen, is placed. This valve is advanced up to the heart and opened like an umbrella right in the middle of the calcified old valve. As the new valve opens, it crushes the old valve toward the walls and takes over its function within seconds. Recovery after the procedure is incredibly fast, and patients can return home within a few days, breathing comfortably.
Who Is Mitral Valve Clipping (MitraClip) Applied to with Interventional Cardiology?
On the left side of the heart, there is a two-part door system that regulates blood flow between the atrium and ventricle; this is called the mitral valve. When this valve cannot close, every time the heart contracts, some of the blood escapes backward toward the lungs instead of moving forward. Over time, this causes fluid accumulation in the lungs and severe shortness of breath.
Again, for these patients with high surgical risk, a wonderful method called MitraClip has been developed. In this method, entry is made through the vein in the groin. With a special device, a small clip shaped like a clasp is placed right in the middle of the two valve leaflets that cannot close completely and cause backward leakage. The clasp fastens these two leaflets together from the middle like stapling them. Thus, while blood flow continues from the sides, the large leak in the middle is stopped. Patients’ quality of life rises rapidly, and hospitalization rates decrease greatly.
What Is Ablation in the Treatment of Rhythm Disorders with Interventional Cardiology?
The electrical system in the heart sometimes begins to produce faulty signals on its own without any external intervention. The heart, which normally works rhythmically, suddenly begins to beat very fast or its rhythm becomes completely irregular because of these short circuits. This condition causes severe palpitations that reduce the person’s quality of life.
In such cases, an electrophysiological study is performed, special wires are sent into the heart, and an electrical map of the inner walls of the heart is created with the tips of these wires. With the energy delivered from the tip of the catheter, this small area is either heated and burned with radio waves or frozen and rendered nonfunctional with special gases. This procedure is called ablation. Since the problematic area is eliminated, the heart’s electrical system returns to its normal settings and the rhythm disorder is permanently treated.
What Should Be Considered After Interventional Cardiology Procedures?
Because modern procedures do not create large incisions in the body, patients get back on their feet very quickly, but this rapid recovery process should not be misleading. The long-lasting success of a successful procedure is directly related to how well the person takes care of their health after the procedure. In order for a newly placed stent to fully adapt to the body and not become filled with clots, it is absolutely essential that the prescribed blood-thinning medications are used without interruption, paying attention even to their timing.
In addition, the colored liquid used during the procedure to make the vessels visible is filtered by the kidneys and removed from the body. It is very important to drink plenty of water for a few days after the procedure so that the kidneys can do this work easily. Mild hardness or a small bruise in the treated wrist or groin area is normal, but if there is sudden growing swelling or severe pain, the hospital should be contacted immediately. The real treatment is the new lifestyle that begins when leaving the hospital. Radical lifestyle changes should be made to keep the body strong in the fight against the disease. The basic habits that should be integrated into life to preserve a healthy vascular structure and support the success of the procedure can be listed as follows:
- Quitting smoking
- Mediterranean diet
- Regular walking
- Stress management
- Weight control
- Treatment of diseases such as hypertension and diabetes

Prof. Dr. Kadriye Orta Kılıçkesmez is one of the leading figures in the field of Turkish cardiology. She was born on January 24, 1974, in Tekirdağ. After completing her undergraduate education at Istanbul University Cerrahpaşa Faculty of Medicine, she chose cardiology as her specialty and received her specialist training at the Cardiology Institute of the same university. In 2015, she was appointed by the university to establish the Şişli Etfal cardiology clinic and Angio laboratory. Becoming a professor in 2017, Kadriye Kılıçkesmez established the cardiology clinic and Angio laboratory of Prof. Dr. Cemil Taşçı Hospital in 2020 and ensured that the clinic became a training clinic.