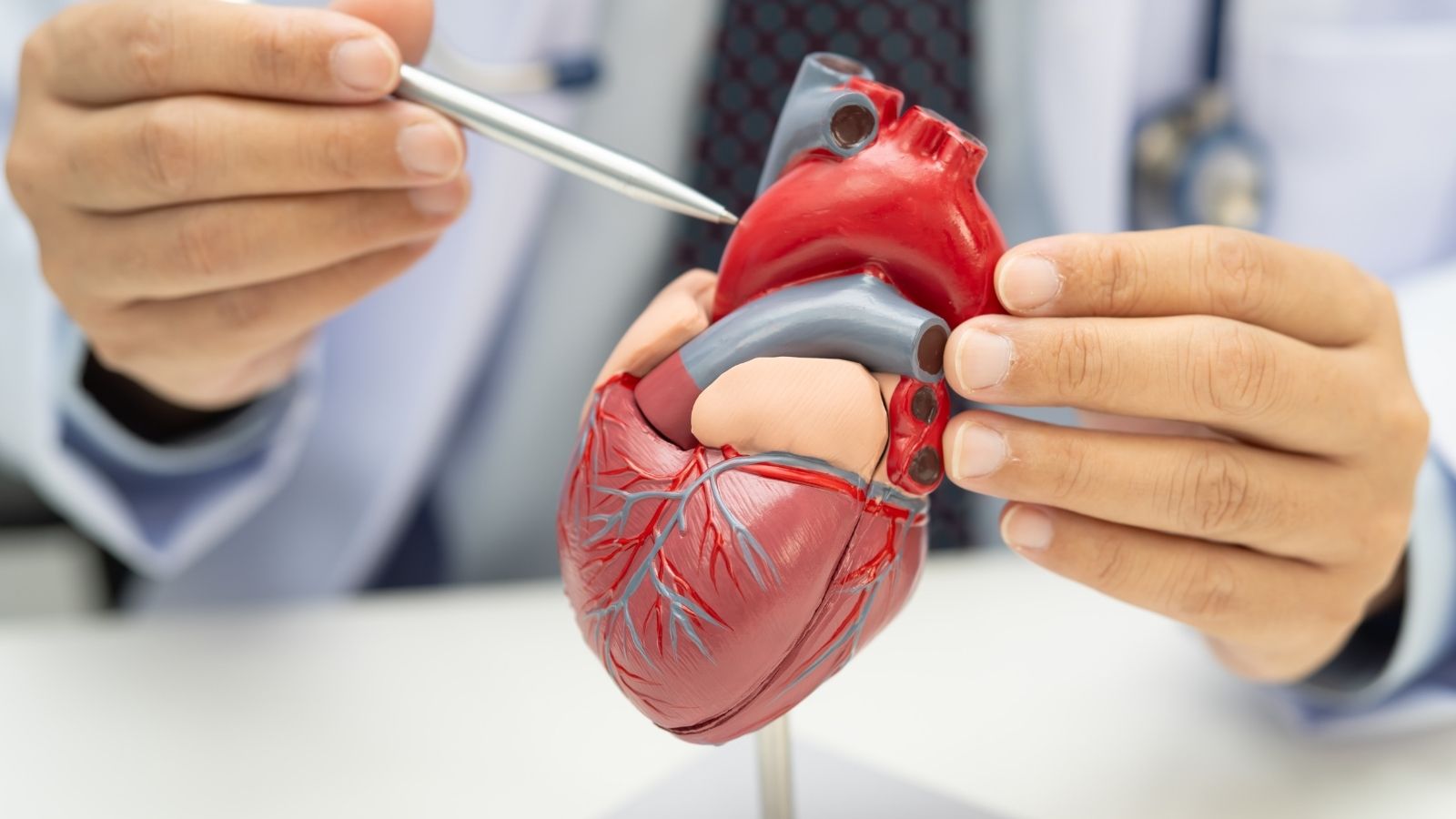
Angiography is the gold-standard diagnostic and treatment method that visualizes blockages in the heart vessels with millimetric precision and detects life-threatening risks in advance. It is generally performed by entering the vascular route through the wrist or groin with the help of a thin tube and injecting a special dye substance to create a detailed X-ray map of the heart. This method not only shows vascular narrowing but also offers the opportunity to intervene immediately in blocked vessels with applications such as stents and balloons. Although the procedure is performed with high success using advanced technologies, it is an invasive procedure that carries risks such as bruising, bleeding at the entry site, or rarely serious complications.
Why Do Heart Vessel Blockages Occur and Why Is Angiography Necessary?
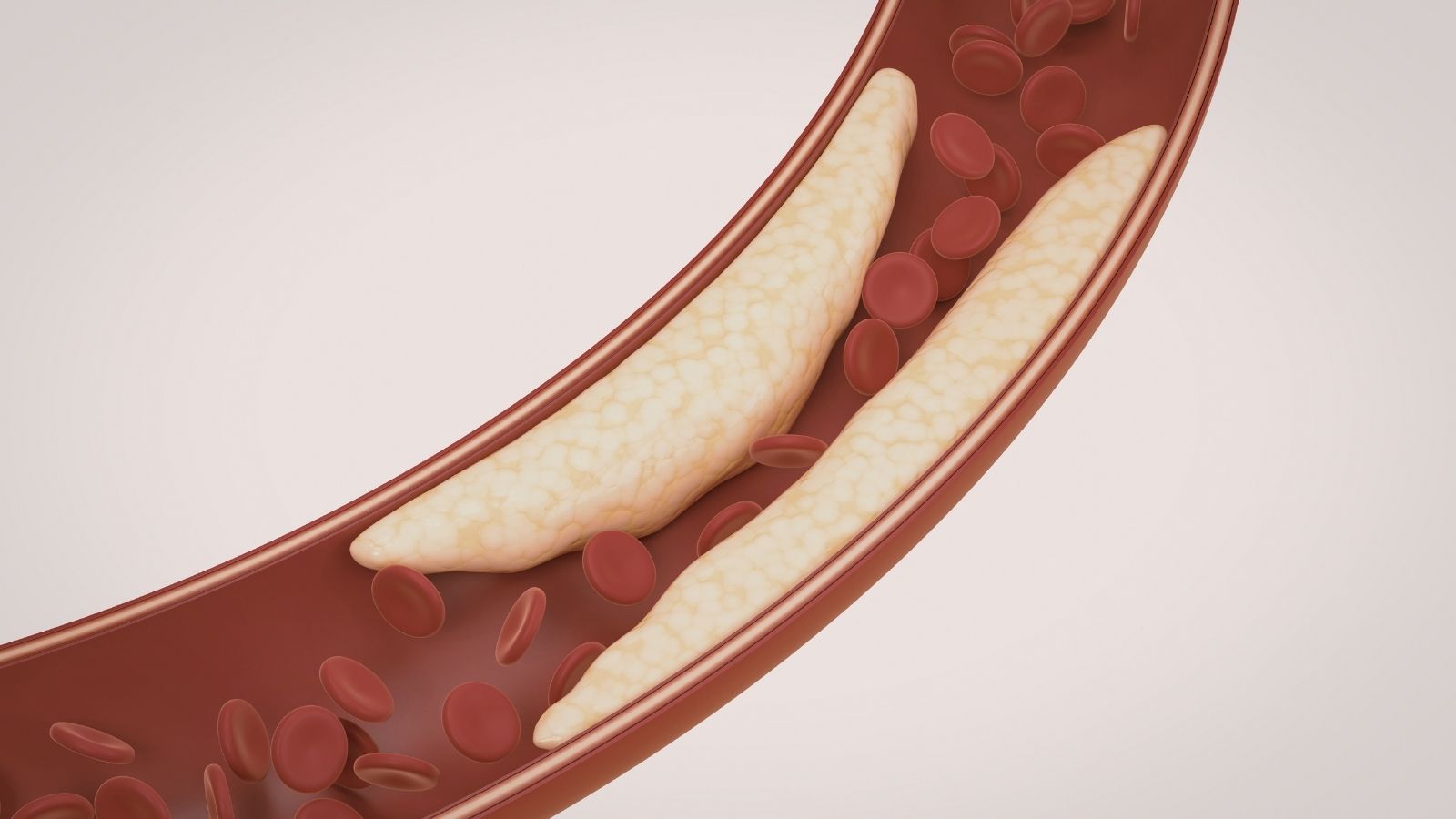
Blockage of the heart vessels is usually not a condition that happens overnight. It is the result of an insidious process that lasts for years, even decades. Cholesterol known as harmful cholesterol, calcium, cellular waste, and clotting factors circulating in the blood gradually begin to seep into the inner surface of the vessel walls. These substances come together to form hard and sticky layers that we call “plaques.” As the process progresses, the inner space of the vessel gradually narrows. When the vessel narrows, the amount of blood that can pass through it naturally decreases.
You can compare this to a garden hose. Just as the flow of water is disrupted when the end of the hose is squeezed, blood flow to the heart muscle is disrupted when a heart vessel narrows. While at rest, that is, when lying in bed or sitting on a sofa, this narrowing may not create a problem because the heart does not need much energy. However, when you start climbing stairs, eat a heavy meal, walk in cold weather, or suddenly become angry, the heart has to beat faster and need more blood. The narrowed vessel cannot meet this increased demand. The heart muscle deprived of oxygen reacts as if saying, “Help me.” This reaction appears as a feeling of pressure, burning, or tightness in the chest area. If this plaque layer suddenly cracks, the body perceives that area as a bleeding wound and can completely block the vessel within seconds by rapidly forming a clot. This condition is a direct heart attack. To see the condition inside the vessels, the exact location of the narrowing, and its severity, it is necessary to look directly inside the vessel. The only method that provides this clear view is angiography.
When Which Symptoms Are Felt Is the Decision for Angiography Made?
Not every chest pain, every palpitation, or every shortness of breath directly means that there is a problem in the heart vessels. Stomach disorders, muscle pain, stress, or cervical disc herniation can also cause pain in the chest area that mimics a heart attack. Therefore, before deciding on angiography, the patient’s complaints are listened to and some preliminary tests are usually performed. ECG recording, checking cardiac enzymes in the blood, treadmill stress testing, or examining the heart with scintigraphy are parts of this process. If these tests raise strong suspicions that the heart is not being adequately nourished, the advanced examination stage is initiated for a definitive diagnosis. In addition, if the patient has complaints that begin suddenly and do not go away, they may need to be taken directly to the procedure room without losing any time.
The main symptoms to pay attention to are as follows:
- Feeling of pressure in the chest
- Pain spreading to the left arm
- Numbness radiating to the jaw
- Unexplained cold sweating
- Sudden shortness of breath
- Burning radiating to the back
- Fatigue that increases with exertion
If these symptoms especially occur during physical activity and resolve with rest, they are considered a serious sign of narrowing in the heart vessels. When the severity of the symptoms and the test results indicate risk, it becomes necessary to create a detailed map of the heart.
What Should Be Considered During the Preparation Process Before Angiography?
Going through a proper preparation process is very important for the safety of the procedure. During this procedure, a special iodine-containing contrast dye is administered into the vessel to make the heart vessels visible on the X-ray device. This substance is filtered from the body through the kidneys and excreted in the urine. In order for the kidneys to handle this load comfortably, the patient’s kidney functions must be checked with blood tests before the procedure.
There are some rules that the patient must carefully follow before the day of the procedure. Since having plenty of water in the body makes the kidneys’ job easier, it is recommended to drink slightly more water than usual the day before the procedure. The procedure is not performed under general anesthesia, meaning the patient is not fully put to sleep; however, the stomach is still required to be empty. For this reason, the patient is asked not to eat or drink anything for a certain period before the appointment time. A plan must be made regarding how regularly used blood pressure, heart, or diabetes medications should be taken that day. Especially for patients using blood thinners, the medication plan is adjusted completely according to the individual situation.
The preparation steps before the procedure are as follows:
- Blood tests
- Kidney function tests
- Medication dose planning
- Adjustment of fasting duration
- Increasing water consumption
- Allergy questioning
When all these preparations are completed fully, the procedure can begin in an extremely safe and comfortable manner.
Should Angiography Be Performed Through the Wrist or the Groin?
To reach the heart vessels, it is necessary to enter the vascular system from outside the body. There are two main entry gates in the body that can be used for this. One is the radial artery in the wrist, where we feel our pulse, and the other is the larger femoral artery located in the groin area. Today, medical approaches and technological developments have brought one of these two methods much more to the forefront in terms of patient comfort and safety.
Procedures performed through the wrist are one of the most comfortable points reached by modern medicine. Because the wrist artery is very close to the skin surface, closing the small entry hole in the vessel after the procedure is extremely easy. With a simple pressure bandage applied there, the risk of bleeding is brought close to zero. The best part is that the patient can stand up immediately after the procedure, eat their meal, and walk home within a few hours.
The groin vessel is the traditional route. Since the vessel diameter is much wider, it is still a lifesaving gateway in some special and complex procedures when many large devices need to be sent to the heart. However, because the groin vessel is deep, special effort is required to stop bleeding after the procedure. The patient must lie completely still on their back for at least four to six hours, not bend the leg, and carry a heavy sandbag on that area. This process can be quite troublesome for those with lower back pain or those who cannot lie down for a long time. Therefore, unless it is necessary, the first choice is always the wrist.
How Does the Angiography Procedure Take Place Step by Step?
Patients are usually excited or anxious because they will enter an environment similar to an operating room. The procedure is performed in a very clean, cool room called a “catheter laboratory,” with a movable bed in the middle and advanced X-ray cameras and monitors around it. When the patient is placed on the bed, they are connected to devices that continuously monitor heart rhythm, blood pressure, and oxygen level in the blood.
First, the entry area, namely the wrist or groin, is completely cleaned with special antiseptic solutions and disinfected from germs. Sterile drapes are placed over you. Then, just as dentists do, a local anesthetic is injected into that area with a thin needle. In this way, only the few-centimeter area where entry will be made becomes completely numb. During the rest of the procedure, no pain or ache is felt; the patient is awake and can talk comfortably.
A very thin, short, valve-tipped plastic sheath is placed into the vessel from the numbed area. The materials to be used throughout the procedure pass through this sheath and reach the heart, so the patient’s vessel is not damaged. Through this sheath, hollow and very flexible tubes, about the thickness of spaghetti, are slowly advanced through the vascular system toward the heart. Since there are no pain nerves inside human vessels, patients absolutely do not feel this advancement. When the tip of the tube is positioned at the starting point of the vessels feeding the heart, the special dye substance is injected through the tube. At the same time, the X-ray device rotates around the patient and records videos from different angles. The flow of the dye inside the vessel appears instantly on the screen; if there is narrowing or blockage in the vessel, the passage of the dye appears like a thin thread or stops completely. This diagnostic stage usually takes only ten to fifteen minutes.
How Are Blocked Vessels Opened with Balloon and Stent During Angiography?
After the images are obtained, if a serious narrowing is detected in the vessels, the patient’s condition and the structure of the blockage are quickly evaluated. In suitable cases, an uninterrupted transition is made from the diagnostic stage to the treatment stage on the procedure table. This process is called “percutaneous coronary intervention” and is a very valuable technology that saves the patient from open-heart surgery.
To open the narrowed vessel from the inside, first a very special, soft-tipped guidewire slightly thicker than a strand of hair is sent through the tube and passed across the narrowing to the other side. This wire acts as a kind of railway track inside the vessel. Then, a deflated balloon is advanced over this wire and positioned exactly at the point of narrowing. Liquid is injected into the balloon under high pressure from outside with a special syringe mechanism. When the balloon inflates, it crushes the hard cholesterol plaque blocking the vessel path and compresses it toward the vessel wall, opening a tunnel through which blood can pass.
However, when the balloon is deflated and withdrawn, the vessel carries the risk of narrowing again due to its elastic structure or the crushed plaques inside sagging and blocking the passage again. This is where stents come into play. The structure we call a stent is a scaffold in the form of a miniature tube woven from very thin metal wires. The stent is sent into the vessel compressed onto a deflated balloon. When it reaches the correct location, the balloon is inflated again; as the balloon inflates, the stent expands and embeds firmly into the vessel wall. When the balloon is deflated and removed, that metal scaffold remains inside the vessel for life. Thanks to that steel cage, the vessel no longer collapses at that point and blood flow completely returns to normal.
What Are the Types of Stents Used in Angiography?
Stent technology is one of the fastest developing fields of medicine. At first, while only structural solutions that prevented the vessel from collapsing again were sought, today advanced technology products that respond at the cellular level are used. Different types of stents may be preferred according to the structure of the vessel, the length of the narrowing, and the patient’s characteristics.
Common stent groups are as follows:
- Bare-metal stents
- Drug-eluting stents
- Dissolving stents
Bare-metal stents are first-generation stents made only from special steel or cobalt alloys. Although they are successful in mechanically keeping the vessel open, after a while the body perceives that metal as a foreign substance. While trying to cover the stent with its own cells, it sometimes produces excessive cells, and this can cause the inside of the stent to narrow again within months.
To solve this problem, drug-eluting stents are now used as standard. The surface of these stents is coated with a special polymer and drug layer that stops cell proliferation. After the stent is placed in the vessel, it slowly releases this drug into the surrounding tissue for months. Thus, the risk of the inside of the stent narrowing by producing tissue on its own is tremendously reduced. Dissolving stents are the newest generation products that, after doing their job and allowing the vessel to heal, completely dissolve and disappear inside the body after a few years, restoring the vessel to its natural structure; however, they are not suitable for every vessel structure.
Which Special Methods Are Used Together with Angiography in Very Hard Vessels?
Sometimes the plaques inside the vessel remain there for so long that intense calcium accumulates inside them, turning them almost into concrete or stone. Trying to inflate only a balloon in such a vessel results in failure; no matter how much the pressure is increased, the petrified structure does not stretch, and if forced too much, the balloon may even burst. In order to open such very hard and complex vessels, advanced special methods must be used instead of standard tools.
At the top of these special methods are plaque shaving devices. A head about the size of an olive pit, with microscopic diamond dust at its tip, is sent into the vessel. This head rotates inside at an incredible speed of one hundred and fifty thousand revolutions per minute and dissolves that petrified calcium by turning it into very fine sand, into dust. After this shaved hard area softens, the stent can be placed easily.
In some cases, the two-dimensional X-ray film taken by angiography is not enough for us to understand the true severity of the narrowing. At suspicious moments when the vessel appears to be 50% narrowed from outside, it is necessary to measure whether the heart muscle is really deprived of oxygen. For this, very sensitive pressure-measuring wires are sent into the vessel, and the blood pressure before and after the narrowing is measured with millimetric precision. In addition, by sending very thin ultrasound devices or microscopic cameras working with laser light into the vessel, the vessel wall is examined from the inside in 360 degrees and three dimensions. In this way, whether the stent fits the vessel perfectly is checked flawlessly. These advanced imaging and measurement devices are the greatest aids that minimize the margin of error of the procedure.
Which Treatments Can Be Performed with the Angiography Method in Heart Valve Diseases?
The opportunities offered by interventional cardiology are not limited to opening blocked vessels. Thanks to advancing technology, even the repair or replacement of the doors between the chambers of the heart, namely the heart valves, can now be performed without splitting the chest. Especially for elderly patients, patients with lung or kidney problems, and patients too weak to tolerate open-heart surgery, these methods are almost like a miracle.
When the aortic valve, the main exit gate through which blood is pumped from the heart to the body, becomes calcified and narrowed, a new biological valve is advanced to the heart through a thin tube by entering through the patient’s groin. This new valve, placed inside the old valve, opens like an umbrella and immediately begins to perform its function, and the patient can stand up the next day. Likewise, loosened mitral valves that leak blood backward can be reached by the angiography method, and a small clip can be attached to the ends of the valve. In this way, progression toward heart failure can be largely stopped. All these procedures have opened a brand-new page in heart health management.
What Are the Possible Risks and Side Effects of the Angiography Procedure?
In medicine, every intervention performed on a patient, every step taken, and every medication given has its own risk profile. Just as even inserting a needle into the skin may have small consequences, it would not be correct to say that intervening inside the heart vessels carries absolutely zero risk. However, one thing must be known very clearly: when performed with proper preparation, an experienced team, and in a modern laboratory environment, the serious life-threatening risks of this procedure are at the level of one in thousands, meaning extremely low. Most situations that may be encountered are temporary side effects that do not leave permanent damage.
Possible risks and side effects are as follows:
- Bleeding at the entry site
- Bruising under the skin
- Swelling in the procedure area
- Itching related to contrast substance
- Rash and allergy
- Temporary kidney sensitivity
- Fluctuation in heart rhythm
Mild bruising and small swellings due to blood leakage at the wrist or groin where the procedure is performed are the most common situations, and the body completely absorbs these on its own within a few weeks. If the body reacts allergically to the dye, the problem is solved immediately with medications. If the patient has a known kidney failure beforehand, the kidneys are protected with careful fluid therapy after the procedure. Major problems such as heart attack or stroke are very rarely seen extreme situations, usually in very severe vascular diseases, and all emergency equipment in the procedure room is kept ready at all times against these possibilities.
What Should Be Considered During the Recovery Period After Angiography?
After the procedure is successfully completed and a stent is placed or only imaging is performed, the patient is taken to the recovery room. The recovery process actually begins as soon as the procedure ends. If the procedure was performed through the wrist, the patient has a transparent plastic band on the arm, resembling a watch strap. This band is gradually loosened and removed. In procedures performed through the groin area, the patient must lie on their back and wait for hours with a sandbag on the groin to stop bleeding.
The first few days after returning home are a critical rest break for the body to recover. Drinking plenty of water that day is essential to ensure that the dye substance in the body is rapidly excreted through the kidneys. The patient is asked not to bathe for the first twenty-four hours and especially to keep the procedure area away from hot water. For at least two or three days, physical activities that will tire the arm or leg too much and carrying heavy bags or objects should be carefully avoided. A slight ache in the wrist or a chickpea-sized firmness in the groin may be considered normal; however, if sudden swelling, a feeling of warmth, severe pain, or bleeding leaking outward is noticed in these areas, the hospital should be contacted immediately. When these small rules are followed, return to normal life will be extremely fast and trouble-free.
Why Are the Medications Used After Angiography Very Important?
After a stent is placed inside a vessel, the biggest and most dangerous mistake patients can make is to feel completely healed and neglect their medications. No matter how advanced the stent technology is, it is ultimately a metallic foreign substance. Our body’s defense system perceives this metal mesh inside the vessel as an open wound or a thorn stuck in the body. The body’s first reaction is to quickly send platelets to that area and try to cover it with a clot. If this clotting occurs, the opened vessel becomes blocked within seconds much more severely than before, and a massive heart attack occurs.
To prevent this life-threatening danger, the patient is given very strong blood-thinning medications that prevent clotting. Depending on the type of stent, these medications must be taken every day, on time, for a certain number of months or years until the stent is completely covered by the body’s own natural cells and becomes “camouflaged.”
The main medication groups are as follows:
- Aspirin
- Second-generation blood thinners
- Strong cholesterol-lowering medications
- Blood pressure regulators
- Stomach protectors
- Rhythm regulators
Special attention must be paid especially to the period when two different blood thinners are used together. Skipping even one day of one of these medications without your doctor’s approval carries a life-threatening risk. If you need to undergo tooth extraction or a minor operation, blood thinners must never be stopped without communication between doctors.
Which Lifestyle Changes Should Be Made to Protect Heart Health After Angiography?
Opening the vessel with angiography and placing a stent is a mechanical repair procedure. We have cleaned the debris blocking the pipe and placed support there; however, we have not completely eliminated the way the factory that caused that debris to accumulate there works, namely the disease of atherosclerosis. If this disease is not treated, it will continue to progress in other vessels and even create new blockages in different parts of the existing stent.
At this point, responsibility passes to the patient. To protect heart health throughout life, placing healthy choices at the center of life is no longer a preference but a necessity. Smoking is the greatest enemy, damaging the inner vessel layer like a razor and increasing the stickiness of blood, and it must be removed from your life immediately and completely. Eating habits must be reviewed entirely, staying away from harmful fats that block the vessels and aiming for natural and clean foods that protect the heart.
Things to avoid are as follows:
- Tobacco products
- Solid fats and margarines
- Processed and packaged meat products
- Excessive salt
- Sugary foods and pastries
Recommended foods are as follows:
- Pure olive oil
- Fresh green vegetables
- Red and purple fruits
- Fatty fish
- Raw nuts

Prof. Dr. Kadriye Orta Kılıçkesmez is one of the leading figures in the field of Turkish cardiology. She was born on January 24, 1974, in Tekirdağ. After completing her undergraduate education at Istanbul University Cerrahpaşa Faculty of Medicine, she chose cardiology as her specialty and received her specialist training at the Cardiology Institute of the same university. In 2015, she was appointed by the university to establish the Şişli Etfal cardiology clinic and Angio laboratory. Becoming a professor in 2017, Kadriye Kılıçkesmez established the cardiology clinic and Angio laboratory of Prof. Dr. Cemil Taşçı Hospital in 2020 and ensured that the clinic became a training clinic.