Cardiovascular occlusion is the narrowing or complete blockage that occurs when cholesterol, fat, and calcium accumulate on the inner walls of the coronary arteries that carry the blood required for the heart to work continuously. In this process, also defined as coronary artery disease, the heart muscle cannot be nourished sufficiently; this brings along chest pain, getting tired quickly, and in serious cases, the risk of heart attack. Today, thanks to advanced angiography techniques provided by interventional cardiology and new-generation drug-eluting stent applications, these vital vessels can be opened safely without the need for surgery. These modern treatment methods extend patients’ life expectancy while allowing them to return quickly to their daily activities.
How Does the Process of Cardiovascular Occlusion Begin Inside Our Vessels?
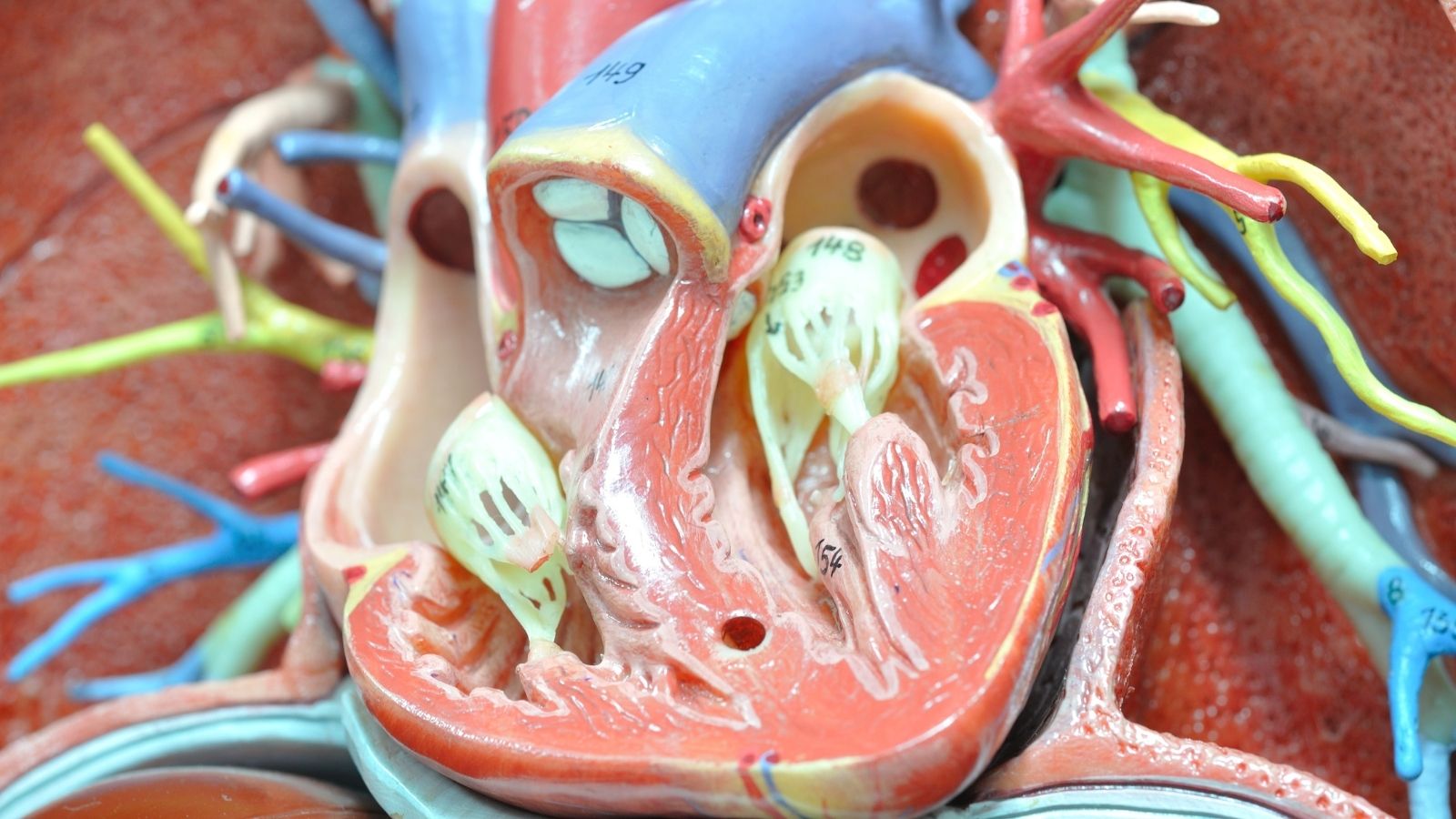
The inside of our vessels is not actually a completely straight, lifeless pipe as commonly thought. There is a very thin, intelligent, and living membrane layer there that allows blood to flow smoothly like oil and prevents clotting. This membrane layer is a magnificent system that can even regulate the widening or narrowing of the vessel by itself. However, over the years, external factors such as the physical pressure created by high blood pressure, toxic chemicals entering the body through cigarette smoke, or uncontrolled blood sugar begin to damage this sensitive membrane. When the membrane is damaged, bad cholesterol particles circulating in the blood leak through these cracks and settle inside the vessel wall.
Our body’s defense system perceives these fat deposits as an enemy and sends cells to the area to destroy them. However, these cells swallow so much fat that they themselves swell there and accumulate. As a result of this silent war lasting for years, plaques form in the vessel wall, filled inside with cholesterol paste and inflammation, and covered outside with a hard sheath. When calcium is added to this structure over time, the vessel loses its beautiful elasticity and the tunnel through which blood passes gradually begins to narrow.
What Are the Main Factors That Increase the Risk of Cardiovascular Occlusion?
This process does not appear suddenly; it is usually the combined result of various risk factors that accumulate over the years. The main factors that prepare the ground for the disease are as follows:
- Advancing age
- Male sex
- Genetic predisposition
- Diabetes
- High blood pressure
- High cholesterol
- Smoking
- Obesity
- Sedentary lifestyle
- Excessive stress
The first three factors listed above are conditions that are not in our hands, that we are born with or inevitably encounter over time. If heart problems occurred at an early age in our family, especially in our mother or father, this indicates that we need to be more careful genetically. However, all the remaining items on the list are completely related to our daily habits and lifestyle. While blood pressure that remains constantly high tires the vessel wall almost by sanding it, smoking is the most dangerous habit that instantly triggers clotting. A sedentary body and increasing weight accelerate this process continuously by increasing general inflammation in the body.
How Do Diabetes and Female Sex Affect the Process of Cardiovascular Occlusion?
Diabetes is like a silent but very destructive storm for the entire vascular network in the body. Sugar circulating constantly at high levels in the blood rusts the vessels from the inside. In diabetic patients, narrowings are generally seen not only at a certain point but much more diffusely and calcified from the beginning to the end of the vessel. This is an important detail that makes the treatment procedures to be performed more difficult.
In women, the estrogen hormone produced by the body before menopause acts as a wonderful protective shield for the vessels. Thanks to this shield, this disease starts at later ages in women compared to men. However, when this natural protection disappears with menopause, the risk level rises very rapidly. Moreover, since women’s vessel structures are thinner than men’s, when the disease starts, it unfortunately tends to progress faster most of the time.
With Which Symptoms Does Cardiovascular Occlusion First Show Itself?
When the vessel gradually begins to narrow, the person may not feel any complaint while resting or sitting because the heart’s blood need is low. However, when physical effort is made, the picture changes. The commonly encountered first symptoms are as follows:
- Pressure in the center of the chest
- Pain spreading to the left arm
- Aching radiating to the jaw
- A feeling of heaviness in the back
- Tightness in the neck area
When the person climbs stairs, goes uphill, or walks after a heavy meal, the heart needs to pump more blood and consume more oxygen. Those narrowed pathways cannot meet this intense demand. The muscle tissue deprived of oxygen transmits this situation to the brain as pain. This pain is often described as a heavy stone sitting right in the middle of the chest, a vise-like tightness, or a serious burning sensation. When the person stops walking and rests, the workload of the heart decreases, so these complaints calm down and disappear spontaneously within a few minutes.
Where Exactly Is a Heart Attack in the Process of Cardiovascular Occlusion?
A heart attack is the event in which those plaques formed over the years can no longer withstand the pressure and suddenly crack or rupture. The membrane layer covering these plaques, which are filled with fat and inflammation, is sometimes very thin. At a moment of extreme stress or a sudden spike in blood pressure, this thin membrane tears. When a tear occurs, the blood inside the vessel comes into contact with this damaged tissue, and the body thinks there is bleeding in that area and piles clot-forming blood cells there within seconds to repair it.
This is where the real disaster begins. The already narrowed vessel becomes completely and suddenly blocked due to this rapidly growing blood clot. Blood flow to the heart muscle drops to zero all at once. The chest pain experienced during a heart attack no longer goes away with rest. The pain is much more severe, may last for hours, and brings with it a very intense fear of death. Every minute the vessel remains closed means that millions of heart cells die irreversibly.
Can Cardiovascular Occlusion Crises Occur Without Any Chest Pain?
This is one of the most dangerous and confusing aspects of this disease. The classic picture of collapsing while holding the chest, as we see in movies, does not always happen. Some patient groups may go through this process very silently without experiencing the classic symptoms at all. The groups at risk are as follows:
- Older individuals
- Diabetic patients
- Female patients
Especially diabetes that continues for years damages the nerve endings in the body. Since the nerve endings become blunted, the patient cannot feel that their heart is deprived of oxygen as pain or ache. We call this silent ischemia. When the patient exerts effort, they may only experience unexplained shortness of breath, extreme fatigue, or darkening of vision. When the vessels feeding the lower surface of the heart become blocked, the pain may radiate to the stomach; the patient may think they are only experiencing heartburn, indigestion, or gas pain. Since such atypical symptoms may delay applying to the hospital on time, they are issues that require extreme attention.
Which Preliminary Tests Are Performed When Going to the Hospital with Suspicion of Cardiovascular Occlusion?
In a person presenting with complaints, the diagnostic process begins with the fastest and least harmful methods. The primary methods applied at this stage are as follows:
- Electrocardiography
- Blood test
- Echocardiography
- Exercise test
- Virtual angiography
The first step of the process is always electrocardiography. Thanks to ECG, the current electrical map of the heart is obtained within seconds and it is understood whether there is an active heart attack. If there is suspicion, hourly blood tests are performed to check for a very special protein called troponin in the blood. When heart cells are damaged, they leak this protein inside them into the blood. With echocardiography, the contraction strength of the heart and its valves are examined using ultrasound waves. If the patient has complaints but resting tests are normal, the exercise test, in which we stress the heart by having the person walk on a treadmill, is used. Beyond all these, the virtual angiography method, which maps the heart with tomography by giving a medication only through an arm vein without entering the vessels at all, has provided great convenience in diagnosis in recent years.
How Is Angiography for Cardiovascular Occlusion Applied for Definitive Diagnosis?
If all the preliminary tests show that the risk is high or if the person arrives directly with a heart attack picture, classic angiography is performed to see the definitive situation. This procedure is absolutely not a surgery. The patient is fully awake and only the small area where the procedure will be performed is numbed with local anesthesia. Very thin, flexible tubes are used to enter through the arteries and advance all the way to the exact starting point of the vessels feeding the heart.
After this point, a special colored liquid is injected into the vessels and a moving film of the heart is taken under an X-ray device. Thanks to this film, answers to questions such as where the blockage is in the vessels, what percentage of narrowing there is, and how long the blocked area is are revealed with millimetric precision. No pain is felt during the procedure, and it is often completed in a short time such as ten or fifteen minutes.
What Are the Differences Between Angiographies Performed Through the Groin and Through the Wrist for Cardiovascular Occlusion?
In past years, angiography was almost always performed through the large artery in the groin area. However, today, wrist angiography, which is a much more comfortable method, is preferred. The main advantages provided by using the wrist are as follows:
- Low bleeding risk
- Ability to stand up immediately after the procedure
- No need for a sandbag
- Often being discharged on the same day
In procedures performed through the groin, because the vessel is very deep and wide, stopping bleeding is quite difficult. After the procedure, the patient must lie on their back for hours, motionless, with a heavy sandbag on top. This is a great ordeal, especially for those with a herniated disc or older individuals. However, the vessel in the wrist is just under the skin, and since there is a hard bone underneath it, when the procedure ends, bleeding is stopped instantly with a small bandage. The patient can get up from the table, walk to their room, eat their meal, and return home walking within a few hours.
Which Sensitive Measurements Are Used in Borderline Cardiovascular Occlusion Cases?
Sometimes when we take the angiography film, we see that the narrowing in the vessel remains between forty percent and seventy percent. It is difficult to understand by simply looking whether a narrowing at this level truly impairs the blood going to the heart. Just as we do not want to place a stent unnecessarily, we also cannot leave the patient untreated. In this case, a technology called intravascular pressure measurement is used.
With a wire as thin as a strand of hair, with a microscopic pressure sensor at its tip, we pass behind the narrowed area in the vessel. We accelerate the heart with special medications and digitally measure the blood pressure before and after the narrowed area. If the pressure drops too much, intervention is performed there. Apart from this, sometimes we enter the vessel with a camera and visualize the layers of the vessel and the exact structure of the plaque with sound- or light-based waves, determining the true size of the blockage millimetrically.
How Does the Balloon and Stent Procedure, Which Is a Non-Surgical Cardiovascular Occlusion Treatment, Progress?
If a serious narrowing or complete closure is detected in the vessel as a result of angiography, treatment is usually started in the same session. The first step is to slowly pass through that blocked narrow area with a very thin, steerable guidewire. This wire then serves as a railway track for the materials to be used afterward. A very small deflated balloon is slid over this wire and brought exactly to the point of narrowing, then inflated from the outside with high pressure.
When the balloon inflates, it crushes that calcified and fatty tissue toward the vessel wall and opens a tunnel through which blood can pass. However, when the balloon is deflated and removed, the vessel may tend to shrink again. To prevent this, a stent, which is a very thin wire mesh made of steel or very special metal alloys and resembles a ballpoint pen spring, is placed in the same area. The stent gives the vessel skeletal support and guarantees that the opened pathway remains permanently open.
What Are the Advantages of New-Generation Drug-Eluting Stents in the Treatment of Cardiovascular Occlusion?
In the bare metal stents used in the past, the body could perceive this metal as a foreign object and pile excessive cells over it, narrowing the vessel again within months. However, the new-generation drug-eluting stents offered by modern medicine have largely solved this problem. The innovations brought by these stents are as follows:
- Low re-occlusion rate
- The intravascular surface remaining smooth
- Special polymer coating on the surface
- The drug being released slowly for weeks
There is a plastic-like coating invisible to the eye on these stents, and very powerful drugs are absorbed into this coating. After the stent is placed in the vessel, it slowly releases this drug to the surrounding tissues for weeks. The drug stops the excessive proliferation of cells. Thus, the inside of the stent remains as smooth as a mirror, and the risk of re-narrowing decreases to almost zero levels. For patients, this technology has extended the lifespan of the treatment incredibly.
Can Cardiovascular Occlusion Cases That Have Remained Completely Blocked for Years Be Opened Without Surgery?
While a sudden vessel blockage causes a heart attack, a vessel may close slowly and remain that way for months or years. We call this condition chronic total occlusion. In the past, absolutely nothing could be done for these vessels, and the patient was sent directly to open surgery. Because the area that remained closed for a long time became almost concrete-like, and passing through that area with classic wires became impossible.
However, today, thanks to very advanced, finely engineered wires and advanced techniques, even these concrete-like pathways can be opened without surgery. Sometimes the blocked area is entered by applying pressure from the front with stiff wires, and sometimes the blockage is approached from the back, that is, in the opposite direction, by going around through the tiny collateral vessels that the heart has created by itself. This is a very difficult procedure that requires manual skill and patience, but when successfully opened, the patient’s quality of life suddenly returns to years earlier, to their healthiest periods.
Which Devices Are Used in Cases of Extremely Calcified and Stone-Like Cardiovascular Occlusion?
Sometimes the stage reached by the disease is so advanced that the inside of the vessel is covered not only with fat but with an intense layer of calcium, turning into a marble pipe. If you apply high pressure with a normal balloon to such a vessel, the balloon may burst or the stent you place may not open among the calcium rocks. In these very difficult cases, special devices that we can call intravascular drills come into play.
At the tip of this device, there is a head the size of an olive pit covered with microscopic diamond dust. This head, sent inside the vessel, rotates at an incredible speed of one hundred and eighty thousand revolutions per minute. Thanks to this rotation, those hard calcium rocks blocking the pathway are abraded and shaved until they become tiny grains of sand. After the vessel is cleaned and made suitable for stretching, the balloon and stent procedure is completed much more safely and flawlessly.
In Which Cardiovascular Occlusion Cases Should a Stent Be Chosen, and in Which Should Bypass Surgery Be Chosen?
Although non-surgical procedures have developed greatly, they do not mean a miraculous solution for every patient. In some cases, open surgery, that is, bypass, is a much more permanent and correct option. When making this decision, cardiology and cardiac surgery teams come together and evaluate the patient’s condition from every aspect.
If the patient has narrowing in one or two vessels, calcification is low, and their general condition is good, the first option is always the stent procedure. However, if the patient has long-standing diabetes and has very widespread and extremely calcified blockages throughout all three main vessels of the heart, the situation changes. Since the lifespan of stents may be short in such cases, opening the rib cage and using completely healthy new vessels taken from the leg or chest to allow blood to bypass the blocked area and reach the heart is a much more reliable method that extends the person’s life.
Which Medications Should Be Used After a Stent Is Placed Due to Cardiovascular Occlusion?
Although the blockage has been physically opened by placing a stent in the vessel, the biological war has actually just begun. Until our body gets used to that foreign metal and covers it with a smooth cell layer, it is very eager to form a clot there. To prevent this, the medication groups that patients must use regularly are as follows:
- Blood-thinning medications
- Cholesterol-lowering medications
- Blood pressure-regulating medications
- Heart rate-slowing medications
The most vital medications in this group are dual blood-thinning therapies. Usually, Aspirin and a stronger second pill added alongside it must absolutely not be skipped during the first year. If the medication is forgotten even for one day, the inside of the stent may suddenly fill with a clot and cause a major heart attack. In addition, even if the patient’s cholesterol level appears normal, cholesterol-lowering medications must remain an inseparable part of lifelong treatment to freeze and harden the plaques in other vessels and prevent them from rupturing.
If Cardiovascular Occlusion Recurs After Treatment, What Kind of Intervention Is Performed?
Despite all these technological developments and drug-eluting stents, human biology can very rarely make surprises. Sometimes the body exaggerates the healing process and fills the inside of the stent with cells, narrowing the pathway again months or years later. The patient begins to feel the old tightness or shortness of breath again while climbing stairs.
In such a case, there is no need to panic at all. The patient undergoes angiography again. Most of the time, there is not even a need to place a new stent. Specially developed drug-coated balloons, whose surfaces are covered with intense medication, are used to inflate the narrowed area. The balloon leaves its drug on the walls, widens the tissue, and is removed. Thus, the inside of the vessel regains its former excellent fluidity.
Which Foods Should Be Consumed to Slow Down the Process of Cardiovascular Occlusion?
For the treatment to be permanent, we need to completely recreate our habits in the kitchen. The main foods that protect and repair vascular health and that we should not leave out of our tables are as follows:
- Olive oil
- Walnuts
- Almonds
- Salmon
- Spinach
- Broccoli
- Oatmeal
- Fresh fruits
- Legumes
Saturated fats, solid fats, and processed packaged foods should definitely be avoided. These products are the direct raw material of plaques inside the vessels. Instead, omega-3-rich fish, green leafy vegetables containing natural antioxidants, and nuts containing healthy fats listed above should be consumed. Olive oil in particular is our most valuable food source that reduces inflammation on the inner vessel surface and suppresses clot formation.
What Should We Change in Our Lifestyle in the Fight Against Cardiovascular Occlusion?
All those miraculous procedures, balloons, and stents performed in the hospital are actually only like repairing a collapse in the road. Preventing that road from collapsing again is entirely related to how firmly you take the wheel of your own life. The real and lasting success of the treatment is hidden in the steps you take after leaving the hospital.
Even staying away from environments where smoking occurs is the biggest step to stop the progression of this disease. Taking brisk walks for just half an hour a day enables the heart to create new collateral vessels and helps the vessels gain elasticity. Taking medications on time and not neglecting regular doctor check-ups is the golden rule of the process.

Prof. Dr. Kadriye Orta Kılıçkesmez is one of the leading figures in the field of Turkish cardiology. She was born on January 24, 1974, in Tekirdağ. After completing her undergraduate education at Istanbul University Cerrahpaşa Faculty of Medicine, she chose cardiology as her specialty and received her specialist training at the Cardiology Institute of the same university. In 2015, she was appointed by the university to establish the Şişli Etfal cardiology clinic and Angio laboratory. Becoming a professor in 2017, Kadriye Kılıçkesmez established the cardiology clinic and Angio laboratory of Prof. Dr. Cemil Taşçı Hospital in 2020 and ensured that the clinic became a training clinic.