Arrhythmia (heart rhythm disorder) is a condition in which the heart beats too fast, too slow, or irregularly due to a disturbance in the heart’s normal electrical conduction system. This condition may affect the heart’s ability to pump blood effectively throughout the body and, in some patients, may lead to serious cardiovascular complications.
Symptoms of arrhythmia may present with clinical findings such as palpitations, irregular heartbeat, dizziness, shortness of breath, and chest discomfort. In some cases, fainting, weakness, or decreased performance during exercise may be observed. The severity of symptoms varies depending on the type of arrhythmia and the patient’s overall health condition.
Causes of arrhythmia include cardiovascular diseases, high blood pressure, heart valve diseases, and congenital abnormalities of the heart’s conduction system. In addition, factors such as electrolyte imbalances, thyroid diseases, certain medications, and intense stress may also affect the heart’s electrical regulation and contribute to the development of arrhythmia.
Risk factors for arrhythmia are closely associated with advanced age, diabetes, obesity, smoking, and chronic heart diseases. For early diagnosis, electrocardiography, Holter monitoring, and other cardiological evaluations may be used. The appropriate treatment plan may include medication, interventional procedures, or lifestyle modifications depending on the type of arrhythmia.
| What You Need to Know | Information |
| Disease Definition | Arrhythmia is a condition in which the heart beats too fast (tachycardia), too slow (bradycardia), or irregularly due to disruption of the heart’s normal electrical rhythm. |
| Types of Arrhythmia | – Tachycardia: Heart beats more than 100 times per minute – Bradycardia: Heart beats less than 60 times per minute – Atrial fibrillation: Irregular and rapid electrical activity in the atria – Ventricular tachycardia/fibrillation: Life-threatening rhythm disorders originating from the lower chambers |
| Symptoms | – Palpitations – Chest discomfort or pain – Dizziness or fainting (syncope) – Shortness of breath – Weakness – Feeling of irregular heartbeat |
| Causes | – Coronary artery disease – High blood pressure (hypertension) – Heart failure – Heart valve diseases – Congenital heart anomalies – Thyroid disorders (especially hyperthyroidism) – Electrolyte imbalances (especially potassium, calcium, magnesium) – Stress, anxiety disorders – Alcohol, caffeine, nicotine, or certain medications |
| Risk Factors | – Advanced age – Family history of arrhythmia – Diabetes – Sleep apnea – Excessive alcohol or substance use – Severe physical or emotional stress |
| Diagnostic Methods | – ECG (Electrocardiogram) – Holter monitoring (24–72-hour ECG recording) – Exercise stress test – Electrophysiological study (EPS) – Echo (echocardiography) |
| Possible Complications | – Stroke (especially associated with atrial fibrillation) – Heart failure – Sudden cardiac death (especially in ventricular arrhythmias) |
What Is Arrhythmia (Heart Rhythm Disorder)?
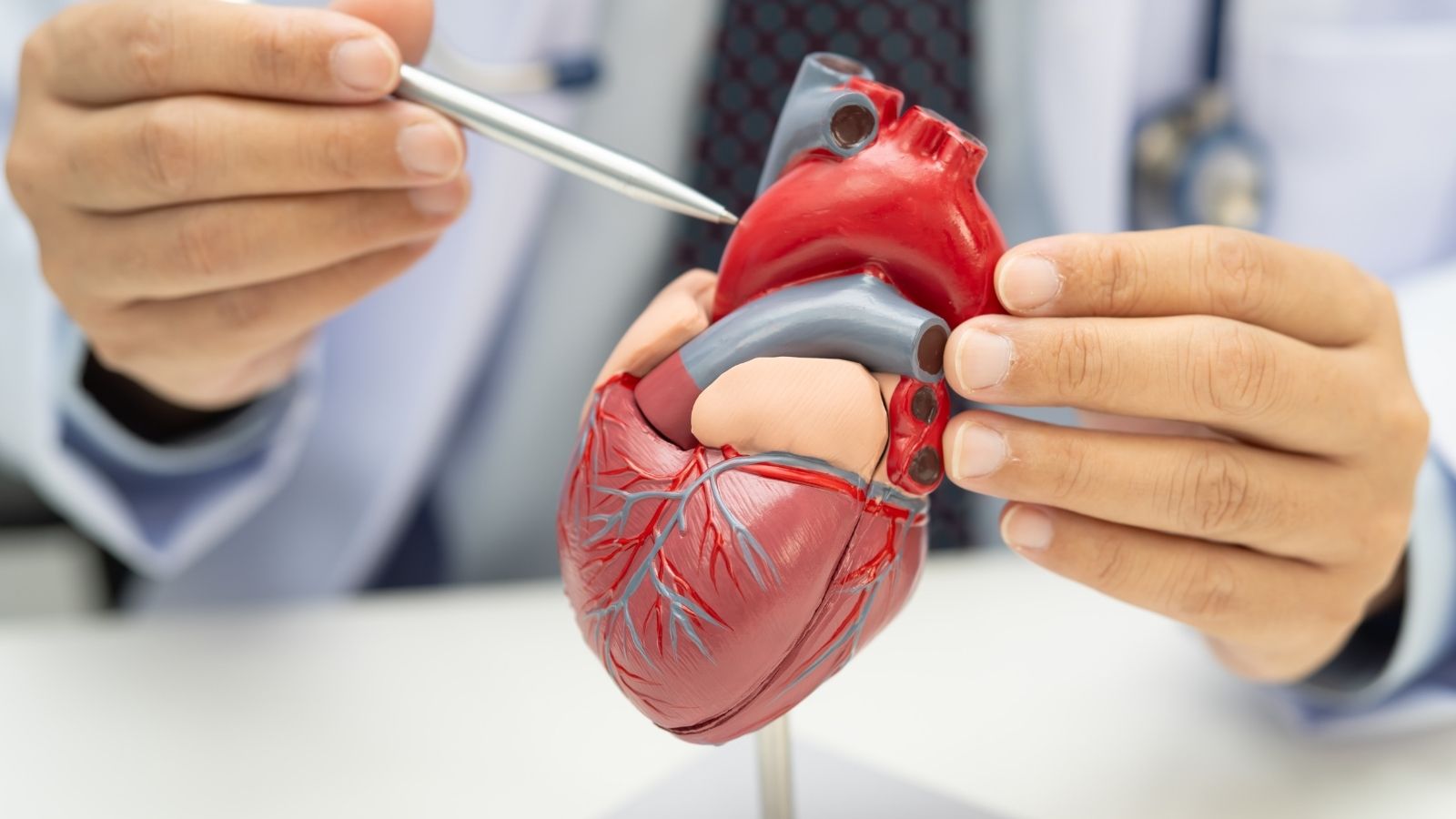
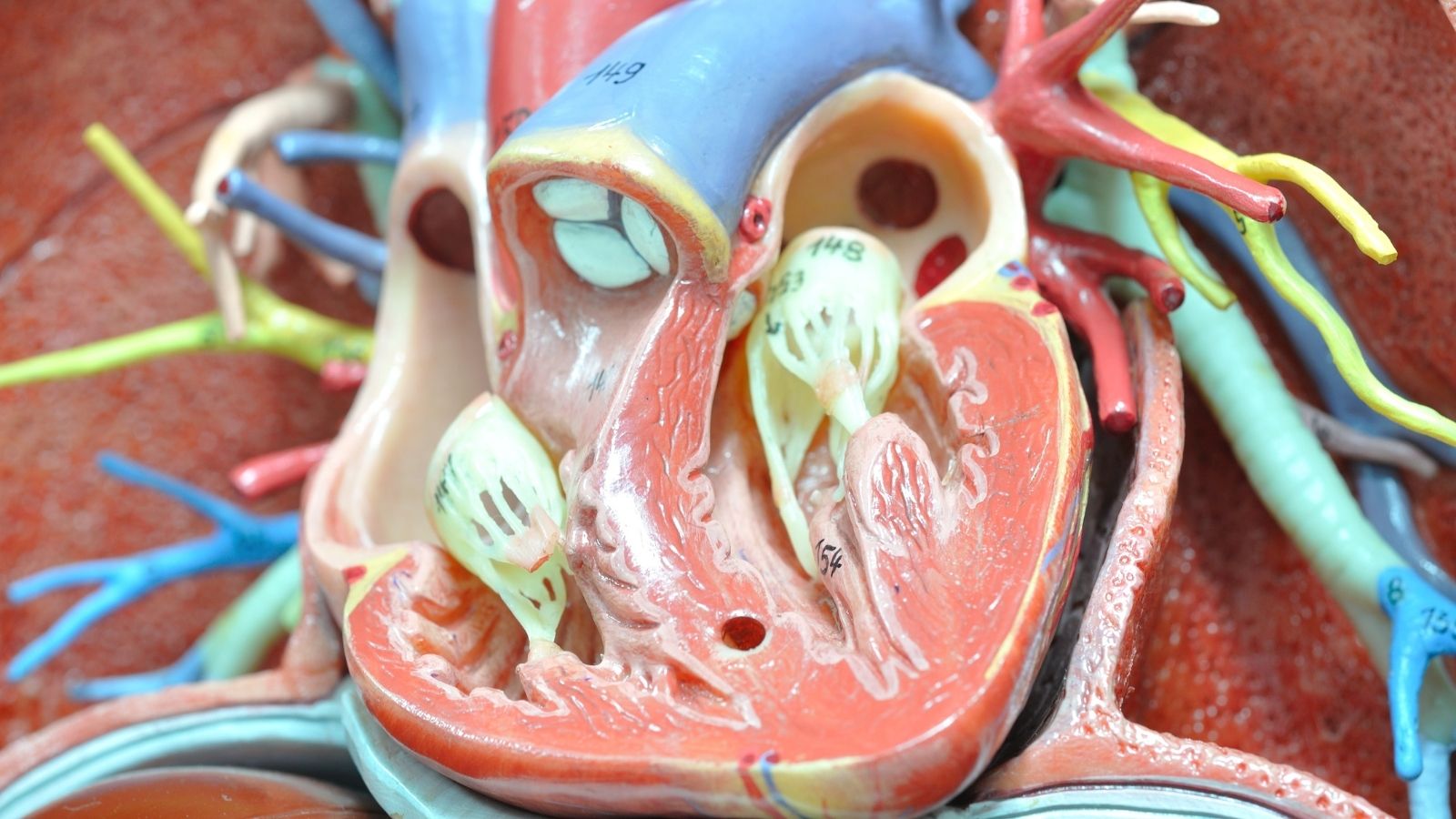
Arrhythmia, the medical term for heart rhythm disorder, is when your heart beats at a different rate than normal or in an irregular pattern. The heart pumps blood throughout the body by contracting regularly with electrical impulses. In arrhythmia, a problem occurs in these electrical signals. This problem may arise from signals being generated too quickly, too slowly, blocked in the conduction pathways, or deviating from normal pathways, leading to disruption of the heart’s normal rhythm. The normal heart rate is typically between 60 and 100 beats per minute. A rate below this range is called bradycardia (slow heart rhythm), while a rate above it is called tachycardia (fast heart rhythm). However, arrhythmia is not only related to speed; irregularity of the heartbeat is also an important type of arrhythmia.
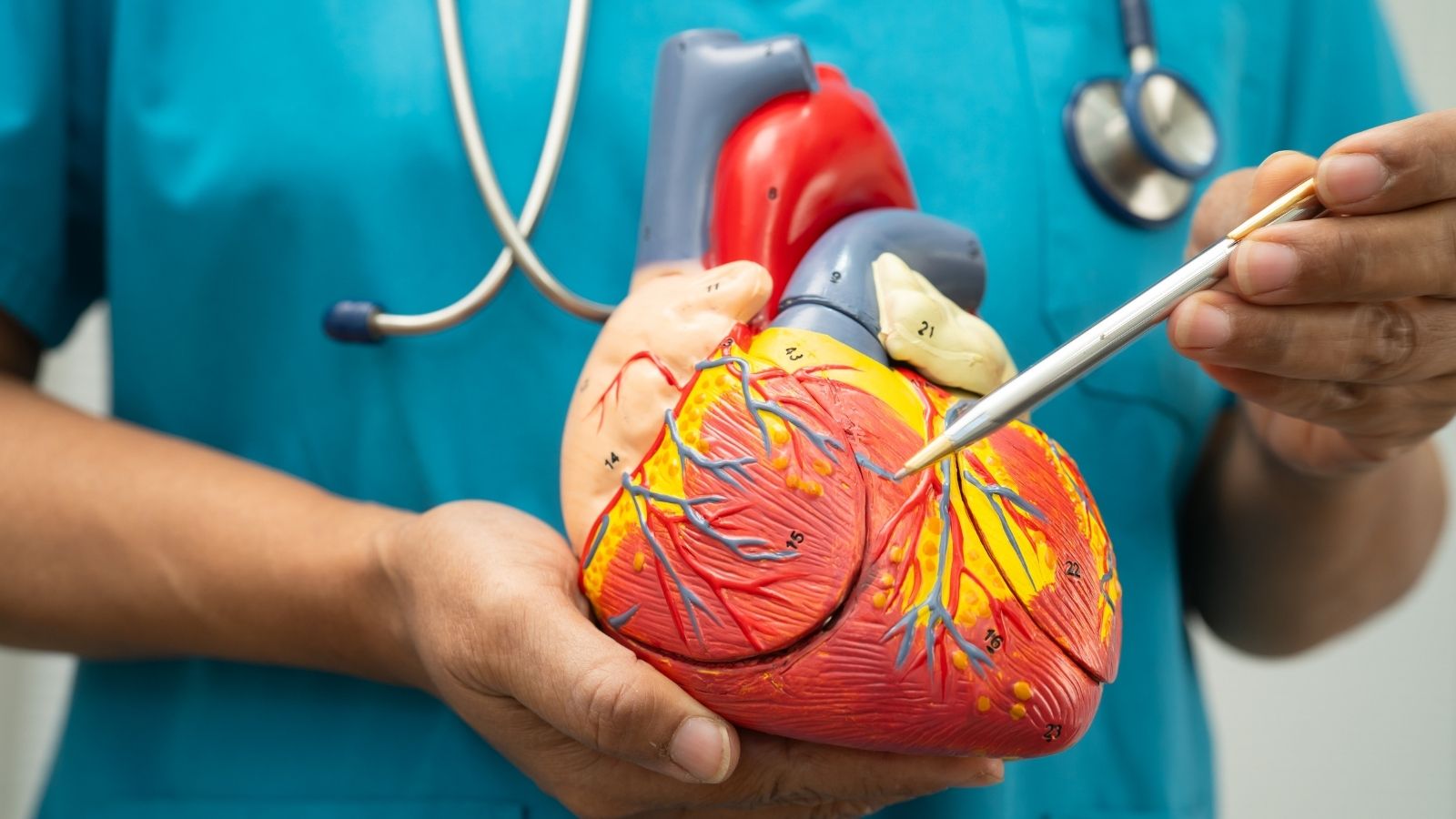
The heart is a complex pump system. It consists of four chambers: two atria and two ventricles. The sinoatrial (SA) node located in the right atrium acts as the natural pacemaker of the heart and initiates regular electrical impulses. These impulses travel from the atria to the ventricles, allowing the heart to contract. Any disruption in this electrical conduction process may cause arrhythmia. The impulses originating from the SA node first stimulate the atria and then reach the ventricles through another gateway called the atrioventricular (AV) node. The AV node ensures that impulses are transmitted to the ventricles in a controlled manner. Delays or premature triggers of signals during this process may lead to rhythm disorders.
Arrhythmias are classified according to where they originate in the heart, their speed, and their cause. One of the most common types of arrhythmia is atrial fibrillation. In this condition, the atria quiver rapidly and irregularly, leading to irregular signals being sent to the ventricles. Other common types of arrhythmia include supraventricular tachycardia (SVT), ventricular tachycardia (VT), and ventricular fibrillation (VF). While SVT originates from abnormal electrical circuits above the ventricles, VT and VF are more serious rhythm disorders originating from the ventricles. VF is a life-threatening condition in which the heart cannot pump blood effectively and requires immediate intervention.
Symptoms of Arrhythmia (Heart Rhythm Disorder)
Symptoms of arrhythmia may vary greatly from person to person. While some individuals experience no symptoms, others may experience quite disturbing and even dangerous signs. Acceleration, slowing, or irregular beating of the heart may lead to a series of changes in the body. These symptoms vary depending on the type and severity of the arrhythmia and the overall health condition of the individual. Being aware of the symptoms is critically important for early diagnosis and intervention.
One of the most common symptoms is palpitations. Palpitations refer to the sensation of the heart beating rapidly, forcefully, fluttering in the chest, or being more noticeable than usual. This sensation may last from a few seconds to several hours. Sometimes, a person may feel as if the heart has stopped and then started again. This is commonly seen especially in irregular rhythms.
Another common symptom is shortness of breath. When the heart cannot pump enough oxygenated blood to the body, shortness of breath may occur due to fluid accumulation in the lungs or insufficient oxygen supply. This condition may become more noticeable especially during exertion or while lying down. The person may feel as if they cannot get enough air.
- Dizziness and fainting (syncope) are also important symptoms of arrhythmia. When sufficient blood flow cannot be delivered to the brain, dizziness, lightheadedness, or visual dimming may occur. If the blood flow to the brain decreases suddenly and significantly, the person may faint. Fainting is especially seen in more serious types of arrhythmia such as ventricular tachycardia or bradycardia and requires emergency medical intervention.
- Chest pain or discomfort may also be associated with arrhythmia. This pain may resemble heart attack pain but may also have a different character. It is usually felt in the center or left side of the chest and may be described as pressure, tightness, or burning. In some cases, this discomfort may spread to the neck, jaw, arm, or back.
- Fatigue and weakness may occur due to insufficient blood and oxygen reaching the body. The person may tire more quickly than usual, have difficulty performing daily activities, and feel a general sense of exhaustion. This symptom is especially common in individuals with slow heart rhythm (bradycardia).
Additionally, some individuals may experience less specific symptoms such as sweating, nausea, or a feeling of anxiety. These symptoms may be related to the body’s stress response or the involvement of the autonomic nervous system.
Variation of Symptoms
Symptoms may vary depending on the type of arrhythmia:
- Bradycardia (Slow Heart Rhythm): Usually causes symptoms such as fatigue, dizziness, fainting, and shortness of breath. These symptoms become more pronounced when the heart rate falls below 40–50 beats per minute.
- Tachycardia (Fast Heart Rhythm): May present with palpitations, shortness of breath, chest pain, dizziness, and sometimes fainting. Heart rates above 150–200 beats per minute may trigger these symptoms.
- Atrial Fibrillation: Palpitations are the most prominent symptom. Shortness of breath, fatigue, and increased risk of stroke may also be observed. This is associated with the heart’s inability to pump blood effectively and an increased risk of clot formation.
- Ventricular Tachycardia and Fibrillation: These conditions usually have a sudden onset and cause severe symptoms. Chest pain, severe palpitations, shortness of breath, dizziness, fainting, and even sudden cardiac arrest may occur. These types of arrhythmia require emergency medical intervention.
Causes of Arrhythmia (Heart Rhythm Disorder)
Heart rhythm disorders may occur as a result of a complex chain of factors. Disruptions in the electrical system that maintains the heart’s normal rhythm may be triggered by underlying health problems or lifestyle factors. Understanding the causes of arrhythmia is of great importance for both prevention and treatment strategies. The origins of arrhythmia range from genetic predisposition to environmental influences.
One of the most common causes is heart disease. Conditions such as coronary artery disease, a history of heart attack, heart valve problems, heart muscle diseases (cardiomyopathy), and heart failure may disrupt the heart’s electrical conduction pathways and lead to arrhythmia. Damage or scar tissue in the heart muscle may create a basis for abnormal electrical impulses. For example, scar tissue formed after a heart attack may cause electrical currents to deviate from their normal path and trigger dangerous arrhythmias such as ventricular tachycardia.
High blood pressure (hypertension) increases the workload of the heart and over time may lead to thickening of the heart muscle (hypertrophy) and changes in electrical conduction. This condition increases the risk of atrial fibrillation. Long-term uncontrolled hypertension alters the structure of the heart and creates a favorable environment for rhythm disorders.
Thyroid gland disorders may cause arrhythmia in both overactive (hyperthyroidism) and underactive (hypothyroidism) conditions. Hyperthyroidism usually leads to increased heart rate and palpitations, while hypothyroidism may rarely trigger rhythm disorders. Thyroid hormones directly affect metabolism and therefore heart rate.
Diabetes may increase the risk of arrhythmia due to both fluctuations in blood sugar levels and vascular damage caused by the disease. Diabetes also increases the risk of other conditions that may lead to arrhythmia, such as heart attack and heart failure.
Side effects of certain medications may cause arrhythmia. Especially blood pressure medications, heart medications, antidepressants, and some respiratory drugs may trigger rhythm disorders. Therefore, it is important to discuss the medications you use with your doctor.
- Alcohol and stimulants (such as caffeine, nicotine, cocaine) may also trigger arrhythmia. Nicotine and illicit stimulants increase heart rate and constrict blood vessels, thereby increasing the risk of arrhythmia.
- Electrolyte imbalances, especially abnormal changes in potassium and magnesium levels, may disrupt the heart’s electrical activity. These imbalances may occur due to vomiting, diarrhea, kidney diseases, or certain medications.
- Genetic predisposition is also among the causes of arrhythmia. Individuals with a family history of arrhythmia may experience rhythm disorders more frequently due to certain genetic mutations. Genetic conditions such as familial hypercholesterolemia or certain types of cardiomyopathy increase the risk of arrhythmia.
- Sleep apnea is a condition characterized by repeated pauses in breathing during sleep and may increase the risk of arrhythmia. Sleep apnea stresses the heart by lowering oxygen levels in the body and increasing blood pressure.
- Aging causes electrical and structural changes in the heart, increasing the risk of arrhythmia. The gradual wear of cells in the heart’s conduction system may lead to rhythm disorders.
- Stress and intense emotional states may activate the sympathetic nervous system, increasing heart rate and triggering arrhythmia in some individuals. This is especially more pronounced in individuals with underlying heart conditions.
Classification of Causes
Arrhythmia causes can generally be classified as follows:
- Structural Heart Diseases:
Coronary artery disease and history of heart attack Cardiomyopathies (heart muscle diseases) Heart valve diseases Congenital heart anomalies Heart failure
- Systemic Diseases:
Hypertension (High Blood Pressure) Thyroid diseases (Hyperthyroidism, Hypothyroidism) Diabetes Sleep apnea Kidney failure
- Electrical Problems:
Conduction system disorders (e.g., Wolff-Parkinson-White syndrome) Inherited arrhythmic syndromes (e.g., Long QT syndrome)
- External Factors and Lifestyle:
Medications (side effects) Alcohol, smoking, caffeine, stimulants Electrolyte imbalances (potassium, magnesium) Intense stress and emotional trauma Excessive exercise (in some cases) Aging
Diagnosis of Arrhythmia (Heart Rhythm Disorder)
Diagnosis of arrhythmia is the first and most important step in reaching the correct treatment. Doctors determine the type, cause, and severity of arrhythmia by listening to the patient’s medical history, performing a physical examination, and using various diagnostic tests. The diagnostic process usually begins with a detailed understanding of the patient’s symptoms. Recording the electrical activity of the heart plays a key role in this process.
- Medical History and Physical Examination
Your doctor will first conduct a detailed interview with you. During this interview, questions will be asked about your symptoms (when they started, how long they lasted, what triggers them), family history of heart disease, medications you use, lifestyle habits (smoking, alcohol, caffeine consumption), and other existing health conditions (blood pressure, diabetes, thyroid, etc.). This information helps the doctor form an initial idea about possible causes.
During the physical examination, your doctor will listen to your heart sounds using a stethoscope. They will check whether the heartbeat is regular and whether there are abnormal sounds (such as murmurs). In addition, your pulse will be checked to evaluate heart rate and rhythm. Blood pressure will be measured, and your general physical condition will be observed. Visible signs such as changes in skin color (paleness, cyanosis) or swelling in the legs may also provide important clues.
- Electrocardiography (ECG or EKG)
Electrocardiography (ECG) is the most basic and most important tool used in the diagnosis of arrhythmia. ECG records the electrical activity of the heart graphically. Electrical signals generated by the heart are recorded through small electrodes attached to your skin. This test usually takes a few minutes and is painless. ECG evaluates the heart’s rhythm, rate, and conduction of electrical impulses. Abnormal rhythms, heart attack, or heart muscle damage may become evident on ECG. However, some types of arrhythmia occur only briefly and may not always be detected on a standard ECG.
- Holter Monitor (24-Hour or Long-Term ECG)
If arrhythmia is not detected on a standard ECG but symptoms persist, your doctor may recommend using a portable ECG device called a Holter monitor. This device continuously records ECG data for 24 to 48 hours or sometimes longer (up to 7 days). The device is worn while performing daily activities. The Holter monitor is very effective in capturing arrhythmias that occur intermittently or are triggered during specific activities. At the end of the recording, the device provides detailed information about your heart rhythm to your doctor.
- Event Recorder
In cases requiring longer monitoring than a Holter monitor, an event recorder is used. These devices are manually activated by the patient when symptoms occur and record ECG data for a certain period. Some event recorders may also automatically record when an abnormal rhythm is detected. These devices may be used for weeks or months and are ideal for documenting infrequent but important arrhythmia episodes.
- Exercise Stress Test
The exercise stress test is used to diagnose arrhythmias that occur or worsen during physical exertion. During this test, ECG is recorded while the patient walks on a treadmill or rides a bicycle. ECG, blood pressure, and heart rate are continuously monitored as exercise intensity increases. The doctor evaluates rhythm disorders, chest pain, or other ECG changes that occur during exercise. This test helps understand the heart’s performance under physical stress.
- Electrophysiological Study (EPS)
Electrophysiological study (EPS) is a more invasive diagnostic method and is generally used to determine the cause and location of complex or treatment-resistant arrhythmias. In this procedure, thin, flexible wires (catheters) are inserted into a vessel through the groin or arm and advanced to the heart. Through these catheters, the electrical activity inside the heart is mapped in detail, and mild electrical stimuli are applied to different areas of the heart to try to trigger arrhythmia. EPS plays a critical role in establishing a definitive diagnosis of many types of arrhythmia and in planning treatment methods such as ablation.
- Additional Imaging Methods
Echocardiography (ECHO): It is an ultrasonographic examination of the heart. It evaluates the structure, size, wall movements, valve functions, and pumping power of the heart. It helps identify underlying structural heart diseases (cardiomyopathy, valve problems) and understand the cause of arrhythmia.
Myocardial Perfusion Scintigraphy: It evaluates blood flow to the heart muscle. It may be used to determine the cause of arrhythmia, especially in cases of ischemia (reduced blood supply) due to coronary artery disease.
Computed Tomography (CT) or Magnetic Resonance Imaging (MRI): It shows the structure of the heart, vessels, and surrounding tissues in detail. It may be used to detect certain structural anomalies or heart tumors.
- Laboratory Tests
Blood tests are used to evaluate conditions that may cause or affect arrhythmia. These tests may include:
- Electrolyte Panel: Measures potassium, sodium, magnesium, and calcium levels. Imbalances in these electrolytes may trigger arrhythmia.
- Thyroid Function Tests: Measure TSH, T3, and T4 levels to evaluate thyroid gland activity.
- Kidney and Liver Function Tests: Provide information about general health by evaluating the function of these organs.
- Complete Blood Count: Used to detect conditions such as anemia.
- Cardiac Biomarkers: Used if there is suspicion of a heart attack (Troponin, CK-MB).
Treatment Methods for Arrhythmia (Heart Rhythm Disorder)
Treatment of arrhythmia is planned individually depending on the type, severity, cause of the arrhythmia, and the patient’s overall health condition. The main goals of treatment are to restore normal heart rhythm, control symptoms, reduce the risk of complications such as stroke, and improve the patient’s quality of life. Treatment options range from medication therapy to lifestyle changes, from surgical interventions to device therapies.
Lifestyle Changes and Control of Triggers
In many types of arrhythmia, lifestyle changes form the basis of treatment or are applied in addition to other treatments. These changes aim to eliminate factors that may trigger arrhythmia.
- Reducing Caffeine and Alcohol Consumption: These substances may trigger arrhythmia in some individuals. Reducing or completely stopping consumption may be beneficial.
- Quitting Smoking: Nicotine increases heart rate and constricts blood vessels, increasing the risk of arrhythmia. Quitting smoking improves overall heart health.
- Healthy Nutrition: It is important to follow a balanced and heart-friendly diet (low in salt, saturated fat, and cholesterol, rich in fruits, vegetables, and whole grains).
- Regular Exercise: Regular physical activity at a level recommended by the doctor strengthens heart health. However, excessive or intense exercise may trigger some types of arrhythmia, so medical advice should be followed.
- Stress Management: Stress-reducing techniques such as yoga, meditation, and deep breathing exercises may be beneficial.
- Treatment of Sleep Apnea: If sleep apnea is present, controlling this condition with treatments such as CPAP devices may positively affect arrhythmia.
- Review of Medications: If there are medications that may cause or worsen arrhythmia, alternatives may be evaluated under medical supervision.
Medication Therapy
Medications are commonly used in the treatment of arrhythmia. Different groups of drugs help regulate heart rhythm through different mechanisms.
- Antiarrhythmic Drugs: These drugs regulate the heart’s electrical activity and help control rhythm disorders. Antiarrhythmics in different classes may slow heart rate, slow conduction, or reduce the excitability of the heart muscle. For example, beta blockers and calcium channel blockers work by reducing heart rate and slowing conduction through the AV node. Class I antiarrhythmics (e.g., flecainide, propafenone) work by blocking sodium channels, while Class III antiarrhythmics (e.g., amiodarone, sotalol) act by blocking potassium channels.
- Anticoagulants (Blood Thinners): Used especially in arrhythmias that increase the risk of clot formation such as atrial fibrillation, to reduce the risk of stroke. Traditional anticoagulants such as warfarin or DOACs (Direct Oral Anticoagulants – e.g., rivaroxaban, apixaban) are used. These drugs reduce the ability of blood to clot and lower the risk of stroke.
- Other Medications: Antihypertensives used to control blood pressure or medications used in the treatment of heart failure may also play a role in arrhythmia management.
Cardioversion and Defibrillation
These methods are used to terminate sudden and potentially dangerous fast and irregular rhythms (especially supraventricular tachycardia, ventricular tachycardia, and ventricular fibrillation).
- Cardioversion: It is the process of restoring abnormal heart rhythm to normal using electrical current or medications. It is usually performed in a planned manner, and mild sedation is applied to the patient. Electrical cardioversion works by delivering a synchronized shock to the heart.
- Defibrillation: It is an emergency intervention applied in life-threatening, unsynchronized ventricular fibrillation or pulseless ventricular tachycardia. A high-energy electrical shock resets the heart’s electrical activity and aims to restore normal rhythm. It may be performed in a hospital setting or through automated external defibrillators (AEDs).
Catheter Ablation
Catheter ablation is a procedure in which abnormal electrical pathways or tissues that cause arrhythmia are destroyed using radiofrequency energy, laser, or cryotherapy (freezing). After identifying the source of arrhythmia during an electrophysiological study (EPS), thin wires (catheters) are guided to the heart. The ablation catheter disables a small area of tissue causing arrhythmia by burning or freezing it. This method is highly effective, especially in conditions such as supraventricular tachycardia, atrial fibrillation, and ventricular tachycardia, and may provide permanent treatment in many patients.
Pacemaker Implantation
A pacemaker is used in cases where the heart beats too slowly (bradycardia) or cannot receive regular impulses due to conduction blocks. The device sends electrical impulses at regular intervals to ensure heart contraction. Pacemakers are usually implanted under the collarbone and connected to the atria or ventricles via thin wires.
Implantable Cardioverter-Defibrillator (ICD)
An implantable cardioverter-defibrillator (ICD) is used in patients at high risk of sudden cardiac arrest. The ICD continuously monitors heart rhythm and automatically delivers an electrical shock when it detects a dangerous arrhythmia (especially ventricular tachycardia or ventricular fibrillation) to restore normal rhythm. ICDs may also function as pacemakers. These devices are known for their life-saving properties and significantly reduce sudden death rates in high-risk patients.
Surgical Treatments
In some cases, especially when other treatment methods fail or when structural heart problems are present, surgical treatment may be required.
- Maze Procedure: It is generally used in the treatment of atrial fibrillation. Small incisions or radiofrequency/cryo lesions are created in the atria to block abnormal electrical impulses and reconstruct normal conduction pathways. This procedure may be performed through open-heart surgery or minimally invasive methods.
- Other Surgical Interventions: Surgeries such as valve repair or replacement and bypass surgery may positively affect rhythm by correcting structural problems that cause arrhythmia.
Next-Generation Treatments
- Wearable Pacemakers: Temporary pacemakers used in cases requiring short-term pacing support, attached to the skin or worn as chest bands.
- Robotic Catheter Ablation: Use of robotic systems for more precise and controlled ablation procedures.
- Advanced Imaging Techniques: 3D mapping systems increase the accuracy of EPS and ablation procedures.
Key Considerations in Arrhythmia Management
Management of arrhythmia is not limited to medical treatments; it also requires the patient’s lifestyle adjustments, regular follow-up, and a proactive approach to potential complications. Living with arrhythmia is possible with proper knowledge and support. Future developments have the potential to offer more personalized and effective solutions in arrhythmia treatment.
Regular Medical Follow-Up
It is vital for patients diagnosed with arrhythmia to visit their doctor regularly to evaluate treatment effectiveness and detect possible complications early. During these follow-ups, your doctor will assess:
- Evaluation of Symptoms: Changes in the severity and frequency of your symptoms.
- Effectiveness and Side Effects of Medications: Whether your medications are working and whether they cause any side effects.
- ECG and Other Tests: Periodic ECG or other diagnostic tests to monitor heart rhythm and overall heart health.
- Complication Screening: Especially in patients with atrial fibrillation, evaluation of stroke risk, adherence to anticoagulant therapy, and clot screening. Regular monitoring for signs of heart failure.
- Lifestyle Assessment: Progress and challenges related to diet, exercise, and stress management.
Prevention of Complications
One of the most important complications of arrhythmia is stroke. Especially in atrial fibrillation, the risk of stroke increases due to clots formed in the atria traveling to the brain. Regular use of anticoagulant medications significantly reduces this risk. Other potential complications include:
- Heart Failure: Long-term or untreated arrhythmia may weaken the heart over time and lead to heart failure.
- Sudden Cardiac Death: Life-threatening arrhythmias such as ventricular tachycardia and ventricular fibrillation may cause sudden cardiac arrest. ICD implantation reduces this risk.
- Blood Clot Formation: Clots may form due to stagnation of blood within the heart (especially in the atria).
Frequently Asked Questions
In which situations does arrhythmia occur more frequently?
Arrhythmia is more commonly seen in conditions such as heart disease, high blood pressure, diabetes, thyroid disorders, and intense stress. In addition, excessive caffeine consumption, smoking, and certain medications may also affect the heart’s electrical system and lead to rhythm disorders.
How can arrhythmia symptoms be recognized in daily life?
People with arrhythmia may experience palpitations, rapid or irregular heartbeats, a feeling of tightness in the chest, dizziness, and shortness of breath. In some individuals, sudden fatigue or fainting may also occur, making daily activities more difficult.
In which age groups is arrhythmia more common?
Arrhythmia may occur at any age but is more common in older adults. As age increases, the heart’s electrical system may weaken. However, rhythm disorders may also develop in young individuals with congenital heart disease or in those experiencing intense stress.
Can arrhythmia be triggered by stress and anxiety?
Intense stress and anxiety may increase heart rate and trigger rhythm irregularities. Hormones released during stress may affect the heart’s electrical activity and cause palpitations or irregular rhythm, especially in sensitive individuals.
What complications may occur if arrhythmia is not treated?
Untreated arrhythmias may increase the risk of heart failure, clot formation, and stroke over time. Especially in some rhythm disorders such as atrial fibrillation, the risk of clot formation increases and may lead to serious health problems.
Can arrhythmia be controlled with lifestyle changes?
Lifestyle changes such as healthy nutrition, regular exercise, quitting smoking, and reducing caffeine intake may help control some types of arrhythmia. In addition, stress management and regular medical check-ups play an important role in protecting heart health.
Why can arrhythmia occur during pregnancy?
During pregnancy, increased blood volume and hormonal changes may place additional strain on the heart. This condition may lead to temporary rhythm disorders in some women. Although usually harmless, cardiological evaluation is necessary if symptoms are severe.
Which tests are used to diagnose arrhythmia?
Electrocardiography (ECG), Holter monitoring, and exercise stress tests are commonly used in the diagnosis of arrhythmia. These tests help determine when and under what conditions irregular heartbeats occur by monitoring the heart’s electrical activity.
How is the ablation method applied in arrhythmia treatment?
Ablation treatment involves destroying or freezing the heart tissue responsible for the rhythm disorder using special catheters. This method may help restore normal rhythm by eliminating abnormal electrical pathways in the heart.
What should people with arrhythmia pay attention to while exercising?
Individuals diagnosed with arrhythmia should consult their doctor before exercising. Light to moderate exercise is generally safe, but intense and uncontrolled physical activity may trigger some rhythm disorders. Regular follow-up and an appropriate exercise plan are important.

Prof. Dr. Kadriye Orta Kılıçkesmez is one of the leading figures in the field of Turkish cardiology. She was born on January 24, 1974, in Tekirdağ. After completing her undergraduate education at Istanbul University Cerrahpaşa Faculty of Medicine, she chose cardiology as her specialty and received her specialist training at the Cardiology Institute of the same university. In 2015, she was appointed by the university to establish the Şişli Etfal cardiology clinic and Angio laboratory. Becoming a professor in 2017, Kadriye Kılıçkesmez established the cardiology clinic and Angio laboratory of Prof. Dr. Cemil Taşçı Hospital in 2020 and ensured that the clinic became a training clinic.