Heart rhythm disorder (arrhythmia) is a condition in which heartbeats become much faster than normal, much slower, or completely irregular as a result of disruptions in the heart’s electrical network. When the bio-electrical stimulators that enable the flawless contraction of this miraculous engine inside our rib cage are interrupted, the regular blood flow needed by the body is put at risk. A healthy sinus rhythm being replaced by chaotic signals creates a mechanical weakness that directly reduces the heart’s blood-pumping capacity. This condition, which means much more than a simple skipped-beat sensation, is a serious electrical malfunction that deeply affects overall cardiovascular health and tires the heart muscle when not treated in time.
What Is Heart Rhythm Disorder (Arrhythmia) and What Kind of Electrical System Does Our Heart Have?
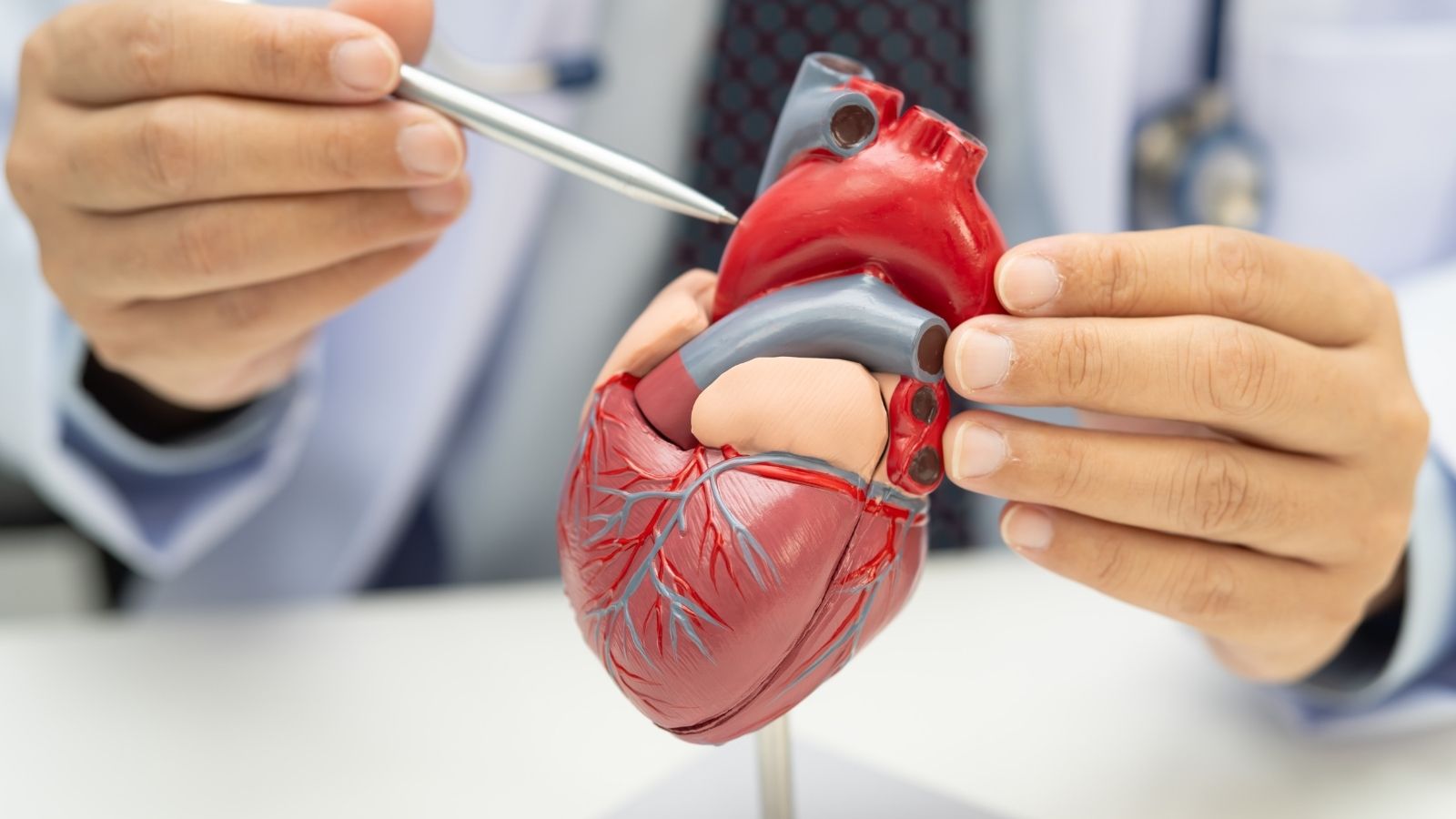
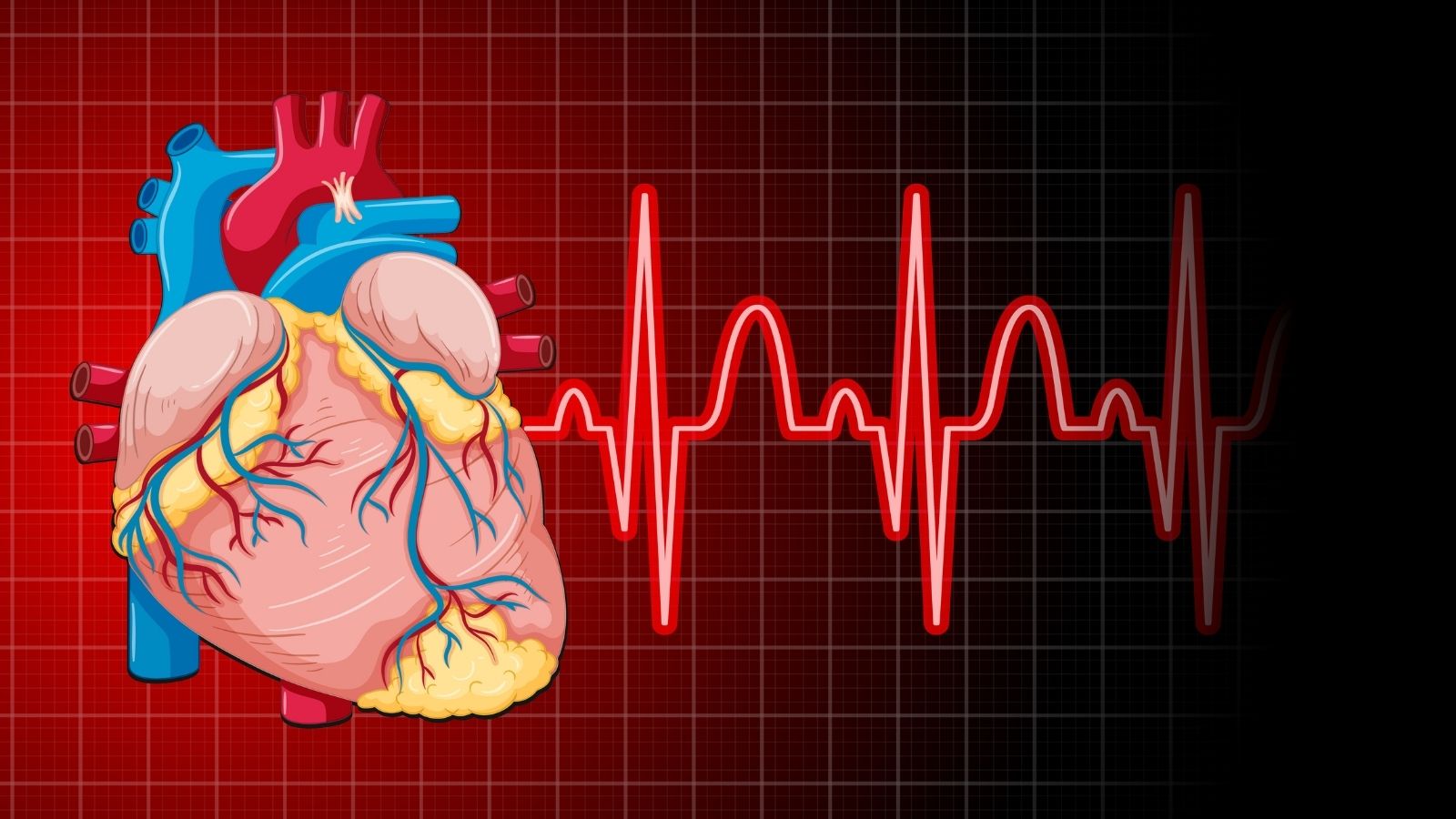
To understand this problem, it is first necessary to take a close look at the heart’s magnificent internal architecture and electrical map. Anatomically, our heart is like a two-story house. On the upper floor, there are two small chambers called atria; on the lower floor, there are two large and powerful chambers called ventricles, which pump blood to the entire body and to the lungs. In a healthy person at rest, the heart beats on average between sixty and one hundred times per minute in an extremely regular harmony. This order is called “sinus rhythm.”
So what starts this rhythm? There is a natural generator, barely visible to the eye but vitally important, located on the ceiling of the upper right chamber of the heart. This is called the “sinus node.” This generator produces electrical sparks according to your mood, physical activity, and the oxygen needs of your body. While you are in deep sleep, the generator slows down and lowers the rhythm; when you climb stairs or become excited, it immediately accelerates to meet the body’s increased demand.
This first electrical signal produced spreads through the upper chambers of the heart, just like the waves created by a stone thrown into water, and enables them to contract. Then this signal reaches a “relay station” (AV node) located exactly in the middle of the heart, the only passage point between the upper floor and the lower floor. The task of this station is great. It holds the signal for a very short time, about one-tenth of a second, delays it, and then releases it downward. Thanks to this brief pause, the blood in the upper chambers has the opportunity to completely fill the lower chambers. When the signal reaches the lower chambers, it rapidly spreads through special distribution cables, creating that powerful contraction, and blood is pumped into the body. Heart rhythm disorder (arrhythmia) is the general name for malfunctions that occur anywhere in this perfectly working generator, relay station, or distribution cables.
What Are the Causes of Heart Rhythm Disorder (Arrhythmia) and Why Does the Electrical Network Malfunction?
Over time, due to genetic predispositions or environmental factors, these electrical pathways inside the heart may wear out. Sometimes, congenital extra microscopic cables become active later in life and cause short circuits. Sometimes a previous heart attack leaves a scar in the heart muscle. This scar turns into an obstacle that is difficult for the electrical signal to cross; the signal circles around this obstacle and forces the heart to beat much faster than normal.
In addition, when the main generator loses control and goes out of circuit, ordinary cells in completely different corners of the heart may begin to produce electricity on their own, as if rebelling. These escape foci disrupt the regular beating of the heart. With the aging process, calcifications or wear may occur in the conduction pathways, causing the signal to fail to pass to the lower chambers and the heart to slow down dangerously.
Common causes of rhythm disorder are as follows:
- Advanced age
- High blood pressure
- Coronary artery diseases
- Previous heart attacks
- Heart valve problems
- Congenital heart anomalies
- Inflammation of the heart muscle
- Overactivity of the thyroid gland
- Diabetes
- Chronic lung diseases
- Sleep apnea
- Excessive caffeine consumption
- Heavy alcohol use
- Use of tobacco products
- Chronic stress and anxiety
- Side effects of some prescription medications
- Mineral imbalance in the blood
Many of these factors strain the physical structure of the heart, causing the chambers to enlarge or the walls to thicken. When the physical structure deteriorates, the electrical system laid inside it also becomes strained, stretched, and eventually loses its function, paving the way for rhythm problems.
What Are the Symptoms of Heart Rhythm Disorder (Arrhythmia) and What Do Patients Feel?
Every person’s body reacts differently. Some people may have very serious rhythm disorders without any complaints, and this condition may be discovered completely by chance on a heart tracing taken during a routine examination. However, in the great majority, this electrical chaos manifests itself with very concrete sensations that directly affect daily life and cause serious concern.
The most common arrhythmia symptoms are as follows:
- Palpitations
- Fluttering sensation in the chest
- Feeling of heartbeat in the neck
- Shortness of breath
- Dizziness
- Blackout of vision
- Fainting
- Feeling as if about to faint
- Pressure in the rib cage
- Chest pain
- Getting tired quickly
- Unexplained weakness
- Cold sweating
To explain in a little more detail how these sensations are experienced: it is quite common to feel as if a bird is fluttering inside the rib cage or as if the heart stops for a moment and then skips very strongly. Especially during sudden-onset rapid heartbeats, the person may become breathless even while sitting, as if they had run for kilometers. When the heart beats very fast, the chambers cannot fill with blood. The blood that cannot fill cannot be pumped sufficiently to the body and, most importantly, to the brain. These seconds-long reductions in blood flow to the brain cause patients to suddenly experience blackout of vision, lose balance, and in advanced cases completely lose consciousness and faint. Such fainting episodes (syncope) are alarms that must be taken very seriously and require the underlying mechanism to be investigated.
What Are the Types of Heart Rhythm Disorder (Arrhythmia) Originating from the Upper Chambers of the Heart?
Rapid rhythm problems originating from the anatomically upper part of the heart, that is, from the atria, are generally called supraventricular tachycardias. A large portion of these are disorders that seriously reduce quality of life and make the person feel constantly on alert, rather than creating a life-threatening situation.
The most frequently encountered condition in this group is “short circuits” that occur in the relay station in the middle of the heart. These attacks, which may appear even at a young age, begin suddenly and end suddenly, just like turning a switch on and off. While watching television or reading a book, the person’s heart may rise within seconds to one hundred fifty or two hundred beats per minute. The signal entering a loop through an extra conduction cable that exists congenitally in the heart and should normally not be there is the best-known mechanism of these short circuits.
The most insidious and most common member of this group in society is atrial fibrillation. This condition is not a simple short circuit but a full electrical storm breaking out in the upper chambers of the heart. The chambers that normally contract regularly with a single signal are bombarded with three hundred or four hundred impulses per minute during this storm. The heart tissue that cannot contract begins to tremble. This trembling state reduces the efficiency of the heart and creates incredible exhaustion and fatigue in the patient. However, the real major danger is not this. When the upper chambers cannot contract regularly, some of the blood pools in the blind spots of the chambers. Stagnant blood, just like still water growing algae, tends to clot over time. If this clot breaks loose and reaches the vessels feeding the brain through the bloodstream, it may lead to very severe consequences called stroke. Therefore, atrial fibrillation requires a comprehensive treatment approach in which not only the heart rate is corrected, but blood-thinning strategies are also planned with great care.
What Are the Life-Threatening Types of Heart Rhythm Disorder (Arrhythmia) Originating from the Lower Chambers of the Heart?
While the upper part of the heart determines the rhythm, the lower part (ventricles) is the real heavy worker that pumps life to the body. Therefore, when the source of the rhythm disorder is the lower chambers of the heart, the condition has the potential to turn into a life-threatening danger within seconds. Ventricular arrhythmias are very critical conditions that immediately disrupt hemodynamic balance, that is, blood pressure and oxygenation of the organs.
This condition usually appears as a legacy of previous infarctions that have left damage in the heart muscle. At the border between damaged dead tissue (scar) and healthy tissue, small current tunnels form due to differences in electrical conduction properties. When the electrical signal gets trapped inside these tunnels and begins to rotate continuously, the lower chambers of the heart completely disable the main generator and take control. When the heart is forced to beat more than two hundred times per minute, it can no longer fill itself with blood and only contracts in vain. Blood pressure drops rapidly, and the patient becomes unable to stand.
The more advanced and most frightening stage of this is ventricular fibrillation. Here, there is no longer any regular electrical cycle. The lower chambers of the heart merely tremble uncontrollably, just like a fish out of water. The heart has mechanically stopped, and no blood goes to any organ, including the brain. This condition is the most common cause of sudden cardiac death, and there is no return unless intervention is performed from outside with a high-energy electroshock device (defibrillator).
How Is Electrophysiological Study (EPS) Performed in the Diagnosis of Heart Rhythm Disorder (Arrhythmia)?
When you go to the hospital, the first thing the physician who listens to your complaints will do is take an electrocardiogram (ECG). ECG is a completely painless and very basic test that monitors the electrical map of the heart from the outside through patches attached to the chest wall. However, ECG has a major limitation; it only takes a snapshot of that moment. If you are not experiencing palpitations or skipped beats at that moment, the ECG may come out completely perfect. Even rhythm Holter devices that you carry on you for days may sometimes be insufficient to catch a hidden rhythm problem. The gold standard offered by medicine for definitive diagnosis is electrophysiological study, which is performed by entering directly into the heart.
This procedure is not a surgery but a special mapping method performed under angiography laboratory conditions. Only the patient’s groin area is numbed, and very thin flexible wires (catheters), whose tips are covered with special electrodes, are placed into the body through the large veins in this area. Using the vascular route like a highway, these wires are advanced into the heart. When the wires are carefully placed in the upper right corner, middle point, and lower chambers of the heart, a real-time, millisecond-by-millisecond sketch of that flawless electrical network inside the heart is reflected on the computer screen.
With impulses given from outside, the frightening palpitation that the patient experiences in daily life is triggered in the laboratory environment under the full control of the physician. The moment the palpitation begins, these smart wires inside determine exactly from which millimetric point the problem originates and whether there is a malfunction in the main cables or side pathways. This procedure is like catching that mischievous cell or faulty cable inside the heart red-handed. After the diagnosis is made, the treatment phase is usually started in the same session before the patient leaves the table.
With Which Methods Is Catheter Ablation Applied in the Treatment of Heart Rhythm Disorder (Arrhythmia)?
In the past, electrical problems in the heart were mainly attempted to be controlled with rhythm-regulating medications that had to be used every day for many years. However, medications do not eradicate the root of the problem; they only mask the disease and may cause some side effects over time. Modern cardiology can now offer permanent recovery (cure) with “catheter ablation,” which physically eliminates the center of the problem. Ablation is the process of permanently silencing that detected faulty short circuit or group of cells producing escape current by using different types of energy.
The basic technologies used for this silencing process have become quite diverse today. The first is radiofrequency ablation, the most commonly used method. When the problematic tissue is reached through a steerable catheter, a very low-voltage alternating current is delivered there. This current creates mild friction heat in the tissue (around approximately fifty degrees) and dries that tiny area as a small point, cutting off electrical conduction forever. This method has extraordinarily high success rates in palpitations that require point-targeted treatment.
Another technology, cryoablation, is based on the principle of treatment by freezing with the exact opposite mechanism instead of heating. It is applied especially through a special balloon placed at the opening of the pulmonary veins where problems such as atrial fibrillation enter the heart. The sub-zero gas sent into the balloon instantly freezes the opening of the vessel in a circular manner and disables the diseased tissues in that area.
The newest revolution creating excitement in the medical world is pulse field ablation (PFA) technology, which works at the cellular level. This method does not use heat or cold; instead, it sends very high-voltage electrical pulses in extremely short periods, as short as one-thousandth of a second. The greatest feature of these pulses is that they affect only heart muscle cells. While opening microscopic pores in the membrane of the problematic cell and rendering it nonfunctional, it does not harm neighboring tissues such as the esophagus or nerve networks. This tissue-selectivity feature has carried the safety of the procedure to unprecedented levels.
How Are Three-Dimensional Mapping Systems Used in the Treatment of Rhythm Disorder (Arrhythmia)?
Especially in dangerous arrhythmias that develop due to damage formed after a heart attack or in complex atrial fibrillation cases, it is not sufficient for the physician to perform the procedure by looking only at two-dimensional shadows under X-ray. The inside of the heart is like a complex cave that is uneven, three-dimensional, and constantly moving. This is where advanced mapping systems come into play.
You can think of these systems as GPS navigation devices used in our cars adapted to the inside of the heart. Thanks to magnetic fields placed under the patient bed and special sensor-equipped wires inside the heart, an exact three-dimensional, colored anatomical model of the heart is built on the computer screen. Moreover, these systems do not only draw the shape; they also show the electrical spread inside the heart live with color scales. The point where electricity starts earliest and shines in red is the very heart of the problem and the main target where ablation will be performed. In this way, procedures are performed with millimetric perfection, not by rote, but through a completely personalized map created for the individual, with zero margin of error.
Who Receives Pacemakers and Shock Devices (ICD) for Rhythm Disorder (Arrhythmia)?
Not all rhythm disorders can be treated with ablation. If the problem is not that the heart beats fast or short-circuits, but that the main cables break due to aging, calcification, or damage and the heart slows down too much, then the body needs external support.
Pacemakers consist of a tiny battery hidden under the skin just below the collarbone and very thin smart wires extending from there through the veins into the heart. These devices are actually not constantly active; they are silent guards that secretly monitor the heart’s rhythm. As long as the heart beats at a sufficient speed on its own, they wait; but if the generator falters or the rhythm becomes dangerously slow, they immediately activate, send small physiological impulses to the heart that are not felt, and ensure that life continues at its normal pace.
There are also shock devices (ICD) that resemble pacemakers in appearance but have a much greater function. These are like a small emergency unit placed in the body, designed for patients with severe damage in their heart and a risk of entering a fatal rhythm disorder at any moment. The second this device detects that chaotic trembling (fibrillation) originating from the lower chambers of the heart, it delivers a powerful electric shock from inside without waiting for a healthcare team to arrive from outside, resets the heart, and brings the patient back to life. Rather than treating, these devices are the strongest insurance that prevents sudden death in high-risk patients.
What Is the Recovery Process Like After Rhythm Disorder (Arrhythmia) Procedures?
The greatest concern of many patients is how difficult the process will be after an intervention on the heart. However, the greatest advantage of modern electrophysiology procedures is that they are performed entirely through the vessels (minimally invasive), without opening the rib cage. After ablation or pacemaker procedures, the patient can usually return home by walking to their loved ones on the same day or the next morning after being kept under observation for one night.
The vessel entered from the groin area heals very quickly. Patients can return to their daily routine activities and desk jobs within a few days after discharge. Mild skipped-beat sensations due to healing in the heart during the first weeks after the procedure are completely normal; this is the heart’s effort to adapt to the new order. What matters is using the medications prescribed by the physician exactly as instructed and following the recommended rest periods. Many people who have lived for years with fear and the anxiety of going to the hospital at any moment experience great psychological relief after a successful procedure and almost start life anew.
The basic steps to be considered after the procedure are as follows:
- Not straining the procedure area
- Not lifting heavy objects
- Consuming plenty of fluids
- Taking medications exactly on time
- Resting for the recommended period
- Not skipping follow-up ECGs
- Taking slow-paced walks
What Can Be Done in Daily Life to Reduce the Risk of Rhythm Disorder (Arrhythmia)?
Despite all these advances in medicine and miraculous technological solutions, the first step in protecting our heart health is in our own hands. The heart is not merely a mechanical pump made of cells; it is a very sensitive organ that instantly reacts to the food we eat, the air we breathe, the water we drink, and most importantly the emotional fluctuations we experience. Many of the factors that trigger rhythm disorders are actually modifiable lifestyle habits. Even if treatment is successful, if these underlying bad habits are not corrected, problems may reappear from another corner of the heart over time. Therefore, taking good care of your body forms the foundation of all advanced treatments to be applied.
Simple measures that can be taken in daily life are as follows:
- Regular brisk walking
- Reaching ideal weight
- Completely quitting smoking
- Restricting salt consumption
- Drinking enough water
- Limiting tea and coffee
- Sleeping regularly
- Practicing stress management
- Regular blood pressure measurement
- Controlling sugar levels
- Regular doctor check-ups
Especially the healing power of losing weight on arrhythmia is an indisputable scientific fact. Even a 10% reduction in body weight incredibly lightens the load on the heart and multiplies the long-term success of ablation procedures. Heart health is a whole that must be cared for not only when disease knocks on the door, but at every moment of life.

Prof. Dr. Kadriye Orta Kılıçkesmez is one of the leading figures in the field of Turkish cardiology. She was born on January 24, 1974, in Tekirdağ. After completing her undergraduate education at Istanbul University Cerrahpaşa Faculty of Medicine, she chose cardiology as her specialty and received her specialist training at the Cardiology Institute of the same university. In 2015, she was appointed by the university to establish the Şişli Etfal cardiology clinic and Angio laboratory. Becoming a professor in 2017, Kadriye Kılıçkesmez established the cardiology clinic and Angio laboratory of Prof. Dr. Cemil Taşçı Hospital in 2020 and ensured that the clinic became a training clinic.