Patent foramen ovale (PFO) is a condition in which the foramen ovale opening between the right and left atria of the heart, which should close after birth, remains open. While this anatomical opening may be asymptomatic in some individuals, it can be associated with clinical conditions such as paradoxical embolism and stroke.
Symptoms of patent foramen ovale are not prominent in most patients and it is often detected incidentally. However, clinical suspicion increases in individuals with a history of cryptogenic stroke, migraine with aura, transient ischemic attack, and rarely systemic embolism. Findings may vary depending on accompanying cardiovascular risk factors.
The diagnosis of patent foramen ovale is made with transthoracic echocardiography and especially contrast transesophageal echocardiography. The method known as the bubble test provides high sensitivity in demonstrating the presence of a right-to-left shunt. Neurological evaluations are also important in the diagnostic assessment process.
Treatment of patent foramen ovale is planned according to the patient’s clinical condition and embolic risk profile. While follow-up may be sufficient in asymptomatic cases, percutaneous closure may be performed in selected patients with a history of stroke. Antiplatelet or anticoagulant therapy is arranged according to an individual risk assessment.
| What You Need to Know | Information |
| Definition | Patent Foramen Ovale (PFO) is a condition in which an intracardiac opening called the foramen ovale, which normally should close after birth, remains open. The foramen ovale is a physiological opening during fetal life that allows blood to bypass the lungs and enter the systemic circulation. |
| Embryological Origin | During the fetal period, the foramen ovale located between the right and left atria (atria) closes functionally after birth as left atrial pressure increases with the onset of pulmonary circulation. In some individuals, this closure is not fully completed. |
| Prevalence | PFO may be present in approximately 20–25% of the population. Most cases are asymptomatic and detected incidentally. |
| Pathophysiology | In the presence of a PFO, a transient or permanent right-to-left shunt may occur from the right atrium to the left atrium. This becomes more pronounced especially when intrathoracic pressure increases (for example, during the Valsalva maneuver). |
| Clinical Significance | It causes no clinical symptoms in most individuals. However, in some cases it may be associated with paradoxical embolism, cryptogenic stroke, and systemic embolic events. |
| Association With Risk Factors | PFO may be detected more frequently particularly in patients who have experienced unexplained (cryptogenic) stroke at a young age. It may also increase the risk of diving-related illness (decompression sickness). |
| Symptoms | It is usually asymptomatic. In possible cases, it may be associated with stroke symptoms (sudden speech impairment, loss of strength), transient ischemic attack, or rarely migraine. |
| Diagnostic Methods | Transthoracic echocardiography (TTE), transesophageal echocardiography (TEE), and the bubble test (saline contrast study) are used for diagnosis. TEE is more sensitive for diagnosing PFO. |
| Treatment Options | In most asymptomatic cases, treatment is not required. In selected patients with a history of stroke, medical therapy (antiplatelet or anticoagulant) or percutaneous closure may be considered. |
| Prognosis | In most individuals it remains uneventful throughout life. Prognosis is generally good in patients who have not developed clinical events. |

Prof. Dr. Kadriye Kılıçkesmez
Cardiology, Interventional Cardiologist – Interventional Cardiologist
Prof. Dr. Kadriye Orta Kılıçkesmez is one of the leading names in the field of Turkish cardiology. She was born on January 24, 1974, in Tekirdağ. After completing her undergraduate education at Istanbul University Cerrahpaşa Faculty of Medicine, she chose cardiology as her specialty and received her specialist training at the Cardiology Institute of the same university.
After working for a short period at Çorlu State Hospital and Turkish Kidney Foundation Service Hospital, she returned to the I.U. Cardiology Institute. Continuing her academic career there, Kadriye Kılıçkesmez became an associate professor in 2012. She then worked at Royal Brompton on complex coronary interventions, CTO intracoronary imaging, and structural heart diseases, and wrote scientific articles. In 2015, she was appointed by the university to establish the Şişli Etfal cardiology clinic and Angio laboratory. Becoming a professor in 2017, Kadriye Kılıçkesmez established the cardiology clinic and Angio laboratory of Prof. Dr. Cemil Taşçıoğlu Hospital in 2020 and ensured that the clinic became a training clinic.
View MoreWhat Is Patent Foramen Ovale (PFO)?
Patent Foramen Ovale (PFO) is a condition in which an opening known as the oval window between the atria of the heart does not close after birth. Normally, this opening, which allows some of the blood going to the baby’s lungs in the womb to pass from the right side of the heart to the left side, usually closes after birth as the lungs begin to function. However, in some individuals this closure does not occur and this condition, called PFO, persists. This opening is present in the adult population at an average rate of 25% to 30%. PFO is generally an asymptomatic (symptom-free) condition, and many people may live their entire lives without realizing it. However, in some cases it can lead to serious complications, especially when blood clots pass through this opening and reach the brain or other organs. Therefore, understanding PFO and knowing its potential risks is of great importance.
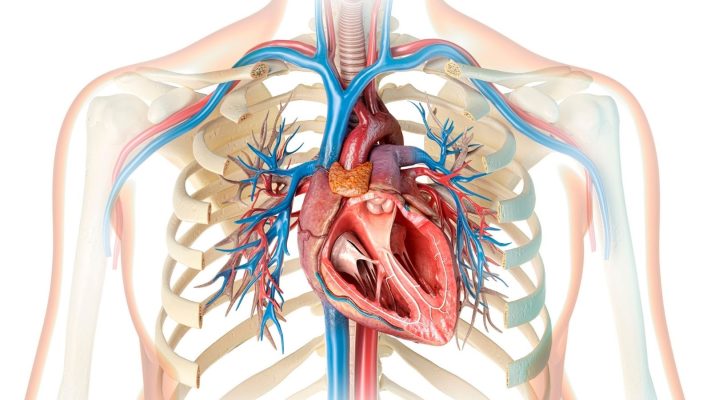
- Heart Structure and Fetal Circulation
The heart is a complex organ consisting of four chambers: the right atrium, right ventricle, left atrium, and left ventricle. Blood returns from the body to the right atrium, is pumped from the right ventricle to the lungs, where it is oxygenated and returns to the left atrium. It is then pumped from the left ventricle to the rest of the body. In babies in the womb, however, the lungs are not yet functioning, so oxygenated blood needs to mix with blood coming from the placenta and be distributed to the body. In this process, an opening called the Foramen Ovale allows direct passage from the right atrium to oxygenated blood in the left atrium. In addition, there is also a connection called the Ductus Arteriosus between the pulmonary artery and the aorta. With birth, when the lungs begin to breathe, these openings are expected to close. The condition in which the Foramen Ovale does not close is PFO.
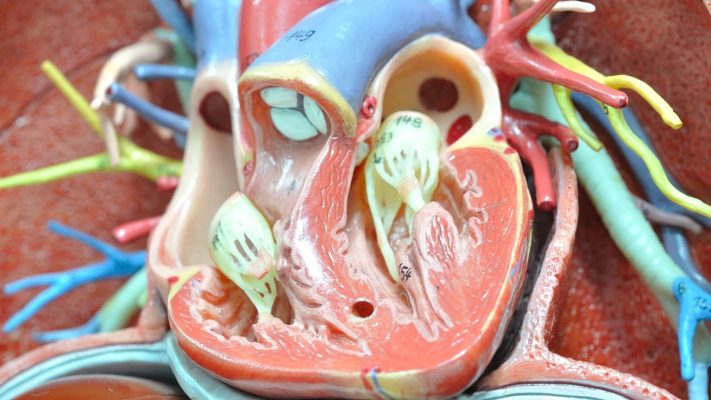
- Anatomical Features of PFO
PFO occurs as a result of incomplete fusion of the walls called the septum primum and septum secundum between the two atria. This opening usually acts as a bridge between the left atrium and the right atrium. The size of the opening can vary from person to person; in some it is millimetric, while in others it may be several millimeters in diameter. The presence of this opening allows blood from the right atrium to mix with oxygenated blood in the left atrium. This becomes more pronounced especially when right atrial pressure is higher than left atrial pressure (for example, during coughing, sneezing, or straining). The presence of a PFO alone may not pose a problem, but risks may increase when combined with other underlying heart conditions or a tendency to form blood clots.
PFO Causes: Is It a Congenital Condition?
PFO is essentially a type of congenital heart opening and is thought to occur as a result of a combination of genetic predisposition and developmental factors. Failure of this opening to close during fetal circulation is the main cause of PFO. However, the reasons why this closure does not occur are not always clear. Some research has shown that certain genetic mutations may increase the risk of developing PFO. In addition, some maternal infections during pregnancy or medications used by the mother may indirectly affect this process, but definitive evidence is limited. Most PFO cases develop spontaneously without a specific trigger. The complex structure of the circulatory system in the womb and the incomplete occurrence of physiological changes after birth play a role in the development of this condition. In the development of PFO, small deviations in the embryological development process are more determinative than environmental factors.
- The Role of Genetic Factors
Genetics is an important factor that can play a role in the development of PFO. Individuals with a family history of PFO have a higher likelihood of having this condition. However, the inheritance pattern of PFO is not fully understood; that is, it cannot be said that a single gene is responsible. It is thought to arise as a result of the interaction of multiple genes or a combination of genetic predisposition with environmental factors. Some studies have investigated genetic variations that may be associated with PFO, but more research is needed in this area. Genetic predisposition may lead to abnormalities in the closure mechanism of the opening or small defects in the development of the heart walls. Therefore, it is recommended that individuals with a family history of PFO or related conditions (for example, stroke) be cautious.
- Abnormalities in the Fetal Development Process
During fetal development, the formation of the heart and great vessels is an extremely complex process. The closure of the Foramen Ovale is also part of this process. If a disruption occurs during this closure process, a PFO may form. The causes of these disruptions may vary; for example, small errors during cell migration or fusion, genetic factors, or certain environmental influences in the womb may affect this process. However, in most PFO cases, no clear teratogenic (development-disrupting) factor can be identified. This leads to PFO generally being considered a random developmental anomaly. These small deviations in the closure mechanism prevent the opening from closing spontaneously after birth.
PFO Symptoms: It Often Remains Silent
The most distinctive feature of PFO is that it often causes no symptoms. Therefore, many people live their entire lives without being aware of this condition. However, in some individuals PFO can lead to serious problems, especially if blood clots pass through this opening and reach the brain. When such complications occur, symptoms may be seen. PFO itself does not directly cause pain or discomfort; symptoms usually arise from secondary conditions caused by PFO. Therefore, PFO is usually diagnosed incidentally during the investigation of another medical condition.
- Association With Stroke (Cerebrovascular Event)
One of the most important and feared complications associated with PFO is stroke. Particularly in strokes seen at a young age (under 55) in people without known risk factors (such as hypertension, diabetes, high cholesterol), the role of PFO is investigated. PFO may cause a blood clot formed anywhere in the body (usually deep vein thrombosis – DVT in the legs) to pass from the right side of the heart to the left side and block brain vessels. This is called paradoxical embolism. Stroke symptoms include sudden speech impairment, weakness or numbness in the face, arm, or leg (usually on one side of the body), loss of vision, loss of balance, and severe headache. These symptoms require urgent medical attention.
- Migraine and PFO
In recent years, research has raised the possible relationship between PFO and migraine. PFO has been found more frequently especially in types of migraine known as migraine with aura, in which visual, auditory, or sensory disturbances accompany the migraine attack. There are various theories suggesting that PFO may trigger migraine attacks. One theory is that certain substances (for example, neuropeptides) that pass from the right atrium into oxygenated blood in the left atrium can affect blood vessels in the brain and trigger migraine. Another theory is that PFO disrupts the flow of venous blood returning from the brain, increasing migraine pain. The presence of PFO in migraine patients is considered as an option in treatment-resistant migraine cases.
PFO Diagnostic Methods: Reaching a Definitive Diagnosis
The diagnosis of PFO is made by using the patient’s medical history, physical examination findings, and various imaging methods together. Since symptoms are usually indirect, it is important to directly identify the PFO itself. This diagnostic process generally begins during the evaluation of stroke, migraine, or other suspected conditions. Doctors carefully assess the patient’s risk factors and symptoms and consider the possibility of a PFO. The main diagnostic methods used are as follows:
- Echocardiography (ECHO)
Echocardiography is the most commonly used method in the diagnosis of PFO. This method uses ultrasound waves to provide detailed imaging of the heart’s structure, chambers, valves, and blood flow. To detect the presence of a PFO, transesophageal echocardiography (TEE) is generally preferred. In TEE, a thin and flexible probe is placed into the esophagus, providing high-resolution images from a position closer to the heart. During this, a special dye (contrast agent) is administered intravenously. If there is a PFO, the passage of these contrast bubbles from the right atrium into oxygenated blood in the left atrium is observed. This finding definitively confirms the presence of a PFO. Transthoracic echocardiography (ECHO performed through the chest wall) can also be used, but it is not as sensitive as TEE in detecting PFO.
- Transcranial Doppler Ultrasound (TCD) and the Valsalva Maneuver
Transcranial Doppler Ultrasound (TCD) is a method used to evaluate blood flow in the brain vessels. In PFO diagnosis, TCD is usually used together with echocardiography. In this method, the patient is asked to perform the Valsalva maneuver. The Valsalva maneuver is the act of holding the breath and straining. During this maneuver, intra-abdominal pressure increases, which raises pressure on the right side of the heart. If there is a PFO, this increased pressure enhances the passage of blood from the right atrium into oxygenated blood in the left atrium. At the same time, the intravenously administered contrast agent can be detected in the brain vessels with the TCD device. TCD has high sensitivity and plays an important role in detecting PFO, especially in patients at risk of stroke. This method helps assess the potential of PFO to send clots to the brain.
- Cardiac Magnetic Resonance Imaging (Cardiac MRI) and Computed Tomography (CT)
Advanced imaging techniques such as Cardiac Magnetic Resonance (MRI) and Computed Tomography (CT) can also be used in the diagnosis of PFO. Cardiac MRI provides high-resolution images of the heart’s detailed anatomical structure and functions. It is especially useful in evaluating the size, shape, and associated other cardiac anomalies of the PFO. CT angiography can be used to more clearly visualize the heart vessels and the PFO opening. These methods may be preferred especially when clear results cannot be obtained with echocardiography or before planning surgical treatment. However, these methods may generally be more costly and less accessible than echocardiography. In addition, CT involves radiation exposure.
PFO Treatment: A Journey From Observation to Surgery
PFO treatment is determined according to the patient’s age, the severity of symptoms, the size of the PFO, and the patient’s overall health status. Not every PFO case requires treatment. For many people, regular follow-up and observation may be sufficient. However, if there are serious complications caused by PFO (for example, stroke, recurrent migraine attacks), treatment options are considered. Treatment approaches may include medication therapy, minimally invasive methods, and rarely surgical intervention. Doctors carefully evaluate the patient’s individual risk factors and the benefit-risk ratio to create the most appropriate treatment plan.
- Medication Therapy and Lifestyle Changes
There is no specific medication therapy for PFO itself. However, blood-thinning medications (antiplatelet or anticoagulants) may be prescribed to prevent PFO-related complications. Especially in patients who have had a stroke, these medications are used to prevent new clot formation and to prevent clots from reaching the brain. Antiplatelet medications such as aspirin and clopidogrel, or warfarin, or new-generation anticoagulant agents are used on the doctor’s recommendation. In addition, lifestyle changes are important. Measures such as healthy nutrition, regular exercise, quitting smoking, limiting alcohol consumption, and weight control improve overall heart health and reduce the risk of possible complications. These measures become even more important especially in patients with a tendency to form blood clots.
- Percutaneous Closure Methods (Device Closure)
Percutaneous closure is the most commonly applied minimally invasive method in PFO treatment. In this method, the PFO opening is closed with the help of a special catheter inserted through the groin without a surgical incision. The procedure is usually performed in an angiography laboratory and under local anesthesia. Umbrella-like devices designed specifically for closure are used. These devices are placed into the PFO opening via the catheter and close the opening by attaching to both atrial walls. Over time, tissue grows around this device and the opening closes permanently. Percutaneous closure is an option that offers lower risk for patients, a faster recovery process, and a shorter hospital stay. This method is successfully applied especially in patients with recurrent stroke or severe migraine attacks. It has an average success rate of over 90%.
- Surgical Closure (Atrial Septal Defect Repair)
Surgical closure is a less preferred method in PFO treatment, but it may be necessary in some cases. This method is usually applied together with other cardiac surgeries or when percutaneous closure is not possible. Surgical closure can be performed as open-heart surgery. The chest is opened and the heart is repaired directly. Today, more minimally invasive surgical techniques are also used; for example, with thoracoscopic surgery, the PFO can be closed through small incisions. In surgical repair, the opening is usually closed with sutures or using a patch. This method may be more appropriate for patients with more complex PFO structures or other accompanying heart problems. However, surgical intervention carries a higher risk than percutaneous methods and the recovery process is longer.
Recent Developments in PFO Treatment and Future Perspectives
PFO treatment is continuously advancing with the development of technology. The widespread use of minimally invasive methods and the development of new devices offer safer and more effective treatment options for patients. In the future, personalized medicine approaches are expected to become even more important in PFO treatment. Thanks to genetic analyses and advanced imaging techniques, the unique characteristics of each patient’s PFO will be better understood and treatment plans will be optimized accordingly. In addition, better understanding of other conditions associated with PFO (for example, migraine, sleep apnea) and integrating these conditions with PFO treatment is one of the important areas of research for the future. Scientists are working on even more advanced closure devices and more precise diagnostic methods.
- Next-Generation Closure Devices
Devices used in percutaneous closure methods are continuously being improved. Next-generation devices are produced from more biocompatible materials, can be placed more easily, and can integrate better with tissue. The design of these devices focuses on reducing the risk of complications such as thrombosis (clot formation) and arrhythmia (heart rhythm disorder). Some new devices have more flexible and adaptable structures to ensure complete closure of the PFO opening. In addition, by increasing device size diversity, more suitable solutions are offered for different PFO sizes and anatomies. These developments make it possible for more patients to be treated without the need for surgery. For example, some devices are made from flexible, shape-memory metals such as nitinol (a nickel-titanium alloy), which makes placement easier.
- Personalized Treatment Approaches
Personalized approaches in PFO treatment refer to creating a treatment plan by considering the patient’s genetic structure, lifestyle, comorbidities, and the specific characteristics of the PFO. For example, more aggressive treatment strategies may be adopted in patients with a high genetic predisposition, while observation may be preferred in low-risk patients. 3D echocardiography and advanced MRI techniques reveal the anatomical characteristics of the PFO in much greater detail and help select the most appropriate closure device. In addition, other conditions affecting the patient’s quality of life (for example, severe migraine) are integrated into the treatment plan. This approach aims to increase treatment success while preventing unnecessary interventions.
The Impact of PFO on Quality of Life and Its Management
PFO itself generally does not directly affect quality of life. However, stroke, migraine, or other complications developing due to PFO can significantly reduce quality of life. Therefore, effective management of PFO and prevention of possible complications are of great importance. Regular doctor follow-ups, regular use of medications recommended by the doctor, and adopting healthy lifestyle habits help individuals with PFO live a higher-quality life. It is also important to maintain the level of physical activity while avoiding overly strenuous activities. Patients are advised to be aware of their health status and to consult their doctors immediately if any new symptom occurs.
- Patient Follow-Up and Doctor Check-Ups
After a PFO diagnosis is made, the patient needs to be followed regularly by their physician. The frequency of follow-ups is determined according to the patient’s condition, age, and whether there are any complications related to the PFO. During doctor visits, the patient’s general health status is assessed, and blood pressure and cholesterol levels are checked. If the patient is taking medication, the effectiveness of the medications and possible side effects are reviewed. In addition, it is asked whether the patient has experienced any new symptoms (for example, headache, vision changes, speech difficulty). When deemed necessary, imaging methods such as echocardiography may be repeated. This regular follow-up process enables early diagnosis of possible complications and timely intervention.
- Psychological Support and Education
Living with a chronic condition such as PFO may create anxiety and stress in some individuals. Psychological support is especially important in situations involving the risk of serious complications such as stroke. Having accurate and up-to-date information about PFO helps patients better understand and manage their condition. Family physicians, cardiologists, and neurologists play an important role in answering patients’ questions and alleviating their concerns. When necessary, support from a psychologist or psychiatrist may also be provided. Patient education programs and support groups also allow patients to share their experiences with each other and feel that they are not alone. Education encourages the patient’s active participation in the treatment process.
Frequently Asked Questions
PFO occurs when the foramen ovale channel, which is open in the womb, does not fully close after birth. This opening between the atria may allow right-to-left blood passage during pressure changes, creating a basis for clots to enter the systemic circulation.
PFO is an important factor especially in unexplained strokes in younger patients. Small clots formed in the leg veins can pass through the opening in the heart, block brain vessels, and lead to a condition called “paradoxical embolism.”
Some studies have found that PFO is more common especially in people with migraine with aura. Microemboli passing from right to left or chemicals in the circulation reaching the brain without being filtered are among the mechanisms thought to trigger migraine attacks.
The increased tendency for clotting during pregnancy may theoretically increase the risk of stroke in the presence of a PFO. However, most women with PFO have uncomplicated pregnancies. In high-risk situations, joint follow-up by obstetrics and cardiology specialists is important.
Gas bubbles that form during scuba diving are normally filtered in the lungs. In the presence of a PFO, these bubbles can pass to the brain and other organs, causing decompression sickness to have a more severe course.
In patients who have had recurrent unexplained strokes and have no other risk factors, cardiologists may recommend PFO closure. The decision is made individually based on age, clot history, and the anatomical characteristics of the opening.
The closure procedure performed via the groin generally allows discharge in a short time. Patients can return to daily life within a few days, but anticoagulant therapy for several months and regular follow-up are required for the device to fully settle.
Most PFOs remain asymptomatic throughout life. However, in high-risk individuals, stroke, transient ischemic attack, or rarely systemic embolism may occur. Therefore, personal risk analysis and regular medical follow-up are of great importance.
It is important to avoid prolonged immobility, drink enough fluids, and avoid habits such as smoking that increase clot risk. Using compression stockings on long flights and moving intermittently can be protective.
A PFO detected especially after a stroke may create anxiety and a sense of uncertainty in the patient. A detailed explanation of treatment options and a regular follow-up plan can help reduce the psychological burden by increasing the patient’s sense of control.