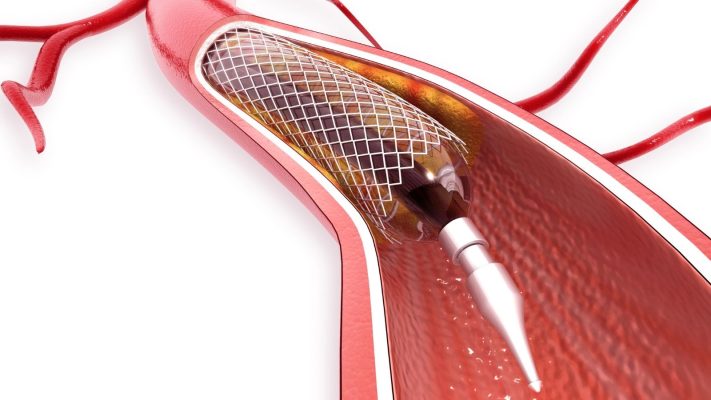
Non-surgical ASD closure is the procedure of closing an atrial septal defect using a catheter method without the need for open surgery. This method enables controlled closure of the hole in the heart with a special closure device advanced through the femoral vein and offers a safe treatment option in suitable patients.
The non-surgical ASD closure method is particularly preferred in secundum type atrial septal defects and is performed in the angiography laboratory. The device advanced under fluoroscopy and echocardiography guidance is placed in the defect area and provides permanent closure by grasping the septum from both sides thanks to its double-disc structure.
Among the advantages of catheter-based ASD closure are short hospital stay, no requirement for general anesthesia, and a rapid recovery process. Avoiding opening of the chest reduces the risk of infection and bleeding, while also providing significant cosmetic superiority and shortening the return-to-daily-life period.
The follow-up process after non-surgical ASD closure includes regular cardiological check-ups, and the position of the device is monitored with echocardiographic evaluation. Antiplatelet therapy is administered for a certain period after the procedure, and the patient’s return to physical activity is planned according to physician recommendations.
What You Need to Know | Information |
Definition | Non-surgical ASD (Atrial Septal Defect) closure is the procedure of closing the hole between the right and left atria of the heart without open-heart surgery, using a special closure device delivered via catheter. |
What Is ASD? | Atrial Septal Defect is a condition among congenital heart diseases characterized by an opening in the septum between the atria. This opening causes oxygenated blood to pass from the left atrium to the right atrium. |
Suitable ASD Types | It is most commonly applied in secundum type ASDs. Primum type, sinus venosus type, and coronary sinus type ASDs usually require surgical treatment and are not suitable for the catheter method. |
Indications | It is recommended in patients with right heart chamber enlargement, significant left-to-right shunt, exercise intolerance, easy fatigability, shortness of breath, recurrent lung infections, and a history of paradoxical embolism. |
Who Is Not Suitable? | It may not be suitable in cases of very large defects, insufficient septal rim tissue, presence of severe valvular heart disease, or other cardiac anomalies requiring surgery. |
How Is the Procedure Performed? | It is usually performed by entering through the femoral vein in the groin and advancing a catheter to the heart. A special double-disc closure device is placed in the defect area and closes the hole by attaching to both sides of the septum. |
Type of Anesthesia | It is mostly performed under general anesthesia or deep sedation. Imaging is performed during the procedure with transesophageal echocardiography (TEE) or intracardiac echocardiography. |
Procedure Duration | It lasts on average between 30–90 minutes and may vary depending on the patient’s anatomical characteristics. |
Length of Hospital Stay | Usually 1 day of hospital observation is sufficient. If no complications develop, discharge may occur the next day. |
Advantages | It is less invasive compared to open-heart surgery, the sternum is not cut, recovery time is short, there is less pain, and the risk of infection is lower. |
Possible Risks | Complications such as device embolization, heart rhythm disorders, vascular injury, pericardial effusion, thrombus formation, residual shunt, and rarely device erosion may occur. |
Success Rate | When appropriate patient selection is made, the success rate is above 95%. Long-term outcomes are generally favorable. |
Post-Procedure Follow-Up | Regular cardiology follow-up is recommended during the first 6 months. Device position and the presence of residual shunt are evaluated by echocardiography. |
Medication Use | After the procedure, antiplatelet therapy (for example acetylsalicylic acid) is generally recommended for 3–6 months. In some patients, a second antiplatelet drug may additionally be prescribed. |
Return to Daily Life | Most patients can return to normal daily activities within a few days. The timing for heavy physical activities is determined according to the physician’s recommendation. |
Long-Term Prognosis | After successful closure, right heart load decreases, symptoms regress, and quality of life improves. Closure procedures performed early reduce the risk of long-term complications. |

Prof. Dr. Kadriye Kılıçkesmez
Cardiology, Interventional Cardiologist – Interventional Cardiologist
Prof. Dr. Kadriye Orta Kılıçkesmez is one of the leading names in the field of Turkish cardiology. She was born on January 24, 1974, in Tekirdağ. After completing her undergraduate education at Istanbul University Cerrahpaşa Faculty of Medicine, she chose cardiology as her specialty and received her specialist training at the Cardiology Institute of the same university.
After working for a short period at Çorlu State Hospital and Turkish Kidney Foundation Service Hospital, she returned to the I.U. Cardiology Institute. Continuing her academic career there, Kadriye Kılıçkesmez became an associate professor in 2012. She then worked at Royal Brompton on complex coronary interventions, CTO intracoronary imaging, and structural heart diseases, and wrote scientific articles. In 2015, she was appointed by the university to establish the Şişli Etfal cardiology clinic and Angio laboratory. Becoming a professor in 2017, Kadriye Kılıçkesmez established the cardiology clinic and Angio laboratory of Prof. Dr. Cemil Taşçıoğlu Hospital in 2020 and ensured that the clinic became a training clinic.
View MoreWhat Is Atrial Septal Defect (ASD)?
Atrial Septal Defect (ASD) is an opening in the septum, the wall between the atria of the heart. Normally, deoxygenated blood returning to the right atrium and oxygenated blood entering the left atrium are kept separate. In the presence of ASD, these two blood flows mix. This mixing increases the workload of the heart and may lead to various health problems in the long term.
Causes of ASD
The exact cause of ASD is often unknown. However, genetic factors, infections during pregnancy, or exposure to certain teratogens are thought to play a role. In some cases, ASD may show familial transmission. Additionally, its frequency may increase when associated with genetic abnormalities such as Down syndrome.
Types of ASD
ASDs are classified according to their location and size in the septum:
- Secundum ASD: The most common type. It is located in the middle part of the septum, at the posterior part of the atria.
- Primum ASD: Located in the lower part of the septum, near the tricuspid and mitral valves.
- Sinus Venosus ASD: Located near the entry of the superior vena cava or inferior vena cava into the atrium.
- Coronary Sinus ASD: A rare type that involves a defect of the coronary sinus.
Symptoms of ASD
Small ASDs may not cause symptoms and may be diagnosed incidentally. However, larger defects or defects that enlarge over time may cause the following symptoms:
- Shortness of breath: Especially during exertion.
- Fatigue: Decreased energy levels.
- Palpitations: Irregular heartbeats.
- Frequent respiratory infections: Especially in children.
- Growth retardation: In infants and children.
- Stroke: In rare cases, it may occur due to blood clots passing from right to left.
Diagnosis of ASD
ASD is usually diagnosed through methods such as physical examination, electrocardiography (ECG), echocardiography (ECHO), and rarely cardiac catheterization. After evaluating your symptoms and medical history, your doctor will determine the appropriate diagnostic methods.
- Echocardiography (ECHO)
Echocardiography is the most commonly used method in the diagnosis of ASD. It uses ultrasound waves to visualize the structure, size, and blood flow of the heart. This provides detailed information about the location, size, and severity of the defect.
- Transesophageal Echocardiography (TEE)
In some cases, echocardiography performed through the esophagus (TEE) may be preferred to obtain clearer images. This method allows closer and more detailed visualization of the heart.
- Cardiac Magnetic Resonance Imaging (MRI) and Computed Tomography (CT)
These imaging methods may be used to provide additional information, especially in complex ASD cases or during surgical planning.
Traditional ASD Treatment: Surgical Methods
In the past, ASD treatment relied almost entirely on surgical methods. In open-heart surgery, the sternum (breastbone) is cut to access the heart, and the hole is closed with special patches or the patient’s own tissue. These methods are effective but meant longer recovery time, more pain, and a higher risk of infection for patients.
- Open-Heart Surgery
In this method, the surgeon opens the chest cavity to directly access the heart. Depending on the size and location of the ASD, a synthetic patch or autologous pericardium is used. The recovery period after surgery usually lasts several weeks, and returning to physical activity may take time.
- Minimally Invasive Surgery
With technological advancements, minimally invasive surgical techniques performed through smaller incisions instead of fully opening the chest have also been developed. These methods may shorten recovery time and provide better cosmetic results. However, they still require surgical intervention.
Non-Surgical ASD Closure: Percutaneous Methods
In recent years, non-surgical ASD closure methods have shown significant development. These methods fall within the field of percutaneous interventional cardiology and are generally performed by accessing a small vessel through the groin or neck. In this way, ASD can be closed without the need for open-heart surgery.
Percutaneous ASD Closure Devices
These devices, which form the basis of non-surgical ASD closure, are specially designed implants. They are generally made of biocompatible metals such as nitinol and have a foldable design. The devices are advanced into the body via a catheter and placed over the ASD to close the hole.
Structure and Working Principle of the Devices
These devices usually consist of two discs. When delivered over the ASD through a catheter, the discs open and settle on both sides of the hole, blocking blood flow. Over time, the body envelops the device and allows it to integrate with the heart’s natural tissue. The devices are designed not to damage heart tissue and remain permanently in the body.
Device Application Process
- Preparation: The patient undergoes a detailed examination and necessary imaging tests before the procedure.
- Anesthesia: Local anesthesia and sedation are generally sufficient. General anesthesia is rarely used.
- Vascular Access: A small incision is made in the femoral artery or vein in the groin area, and a thin sheath is inserted.
- Catheter Placement: Through this sheath, a special catheter is advanced to the ASD. The catheter position is continuously monitored with imaging methods such as echocardiography or fluoroscopy.
- Defect Measurement: The size and shape of the ASD are precisely measured.
- Device Selection and Placement: An ASD closure device appropriate to the measurements is selected. The device, folded at the tip of the catheter, is positioned over the ASD. After confirming correct positioning, it is slowly deployed and placed.
- Control: After placement, it is checked that blood flow has completely stopped and that the device is stable.
- Sheath Removal: The sheath is removed, and pressure is applied to the entry site to stop bleeding.
Different ASD Closure Devices
There are various ASD closure devices offered by different manufacturers on the market. Some of these include:
- A-Seed (Lifetech): A disc-shaped device designed especially for secundum ASDs.
- M-Closer (Lifetech): An option available in different sizes and shapes, suitable for a wide range of ASDs.
- Cardio-SEAL (NMT Medical): This device is also widely used in the closure of secundum ASDs.
- AMPLATZER Septal Occluder (St. Jude Medical/Abbott): A reliable device used for many years in the field of ASD closure.
Each of these devices may have unique advantages and application techniques. The device to be used is determined by the physician according to the patient’s anatomy and the characteristics of the defect.
Advantages of Percutaneous ASD Closure
Non-surgical ASD closure methods have many significant advantages compared to traditional surgery:
- Less Invasiveness: No need for open-heart surgery, meaning less tissue damage.
- Faster Recovery: Patients are usually discharged the same day or the next day. Return to physical activity is much quicker.
- Less Pain: Since there are no surgical incisions, the level of pain is lower.
- Lower Risk of Infection: Since there is no surgical field, the risk of infection is significantly reduced.
- Cosmetic Advantages: No large incision scar remains on the chest.
- Lower Cost: In the long term, cost-effectiveness may increase due to shorter hospital stays and reduced complications.
- Sufficiency of Local Anesthesia: In most cases, general anesthesia is not required.
Disadvantages and Risks of Percutaneous ASD Closure
As with any medical procedure, non-surgical ASD closure methods have potential risks and disadvantages:
- Device Thrombosis: Although rare, blood clots may form on the surface of the device. This may lead to stroke or other embolic events. Patients may need to use blood thinners for a certain period after the procedure.
- Device Displacement: In very rare cases, the device may shift after placement. This may require additional intervention.
- Incomplete Closure of Atrial Septal Defect (Residual Shunt): Despite device placement, a small amount of blood leakage may persist. This is usually clinically insignificant but may require follow-up in some cases.
- Risk of Endocarditis: The presence of the device may theoretically increase the risk of infective endocarditis. Therefore, patients are advised to follow hygiene rules and consult a doctor if signs of infection occur.
- Atrioventricular Conduction Blocks: Rarely, the position of the device may affect conduction pathways and cause temporary or permanent blocks.
- Complications Related to Large Vascular Sheath: Complications such as bleeding, hematoma (blood collection), or pseudoaneurysm may occur at the access vessel.
- Inadequate Anatomical Suitability: Not every ASD patient is suitable for percutaneous closure. Factors such as defect size, location, or vascular structure may prevent application of the method.
Complication Rates
The complication rates of percutaneous ASD closure are quite low. Success rates are generally above 95%. Major complications (stroke, death, major bleeding, etc.) occur in less than 1%. These rates may vary depending on the experience of the center and the technology used. For example, a meta-analysis conducted in 2018 showed that the overall success rate of percutaneous ASD closure was 97.6% and the serious complication rate was 0.7% (Source: Journal of the American College of Cardiology).
Who Is a Candidate for Non-Surgical ASD Closure?
The non-surgical ASD closure method is an ideal treatment option for patients who meet certain criteria. These candidates generally include:
- Patients with Secundum ASD: Percutaneous methods are most effective in closing secundum ASDs.
- Symptomatic Patients: ASDs causing symptoms such as shortness of breath, fatigue, and palpitations.
- Hemodynamically Significant Defects: ASDs that increase the workload of the heart and cause enlargement of the right heart chambers.
- Patients with Surgical Risk: Elderly patients, those with severe lung disease or other chronic conditions who carry high risk for open-heart surgery.
- Anatomically Suitable Patients: Patients whose defect size, shape, and rim structure are suitable for percutaneous device placement.
Which ASD Types Can Be Closed with Percutaneous Methods?
Percutaneous methods are primarily used for closing secundum ASDs. Since this type is located in the central part of the septum, it provides a suitable area for device placement. Other ASD types such as primum ASD, sinus venosus ASD, and coronary sinus ASD generally require surgical intervention. However, with technological advancements, research continues on percutaneous closure of these types using specially designed devices.
Is There an Age Limit?
There is no specific age limit for non-surgical ASD closure. The method can be successfully applied in both infants and elderly patients. However, in infants and young children, the size of the device and the patient’s overall condition are taken into account. In children, the decision to close an ASD is generally based on the size of the defect and the patient’s symptoms. In adults, it may be primarily preferred in patients with high surgical risk or those who refuse surgery.
Pre- and Post-Procedure Process of Non-Surgical ASD Closure
Pre-Procedure Evaluation
Before the procedure, the patient undergoes a detailed cardiological evaluation. This evaluation includes:
- Medical History and Physical Examination: The patient’s overall health status, existing diseases, and complaints are assessed.
- Echocardiography (ECHO): The location, size, rim structure, and hemodynamic significance of the ASD are determined.
- Electrocardiography (ECG): Heart rhythm and possible electrical abnormalities are evaluated.
- Chest X-ray and Blood Tests: Information about general health status is obtained.
- Other Imaging Methods if Necessary: Additional tests such as TEE, MRI, or CT may be requested.
During the Procedure
The procedure is usually performed in the interventional cardiology laboratory under sterile conditions. The physician administers local anesthesia and sedation according to the patient’s condition. The procedure lasts on average 30–60 minutes. During the procedure, the patient’s vital signs (pulse, blood pressure, oxygen saturation) are continuously monitored.
Post-Procedure Care and Follow-Up
After the procedure, patients are usually kept under observation for several hours. They are generally discharged the same day or the next day. After discharge, the following should be considered:
- Rest: Heavy physical activities should be avoided during the first few days.
- Medication Therapy: Blood thinners recommended by the physician (such as aspirin, clopidogrel) should be used regularly. These medications are important to prevent clot formation on the device.
- Wound Care: The entry site should be kept clean and monitored for signs of infection.
- Follow-Up Appointments: Medical check-ups are performed at certain intervals after the procedure (usually at 1, 3, 6, and 12 months). During these visits, echocardiography is used to evaluate the condition of the device and whether the ASD has completely closed.
- Dental Treatments: To reduce the risk of infective endocarditis, it is recommended to consult your doctor before invasive dental treatments and receive necessary antibiotic prophylaxis.
The Future of Non-Surgical ASD Closure
Non-surgical ASD closure methods have provided significant advancement in the field of cardiology. Even greater developments are expected in this area in the future:
- More Advanced Device Designs: More compatible, safer, and easier-to-place devices for different ASD types will be developed.
- Biodegradable Devices: In the future, devices that are not permanent and are absorbed over time in the body are targeted for development.
- Applicability to a Wider Patient Group: Research is ongoing to enable treatment of ASD types that currently require surgery with percutaneous methods.
- Artificial Intelligence and Robotic Applications: Integration of AI-supported imaging and robotic surgical systems may be considered to increase precision and reduce complications during the procedure.
Frequently Asked Questions
Non-surgical ASD closure is generally applied in secundum type atrial septal defects. The size of the hole, adequacy of rim tissues, and heart structure are determining factors for the procedure. In very large defects or anatomically unsuitable cases, surgery may be preferred.
Non-surgical ASD closure is performed through a thin catheter inserted from the groin. The special closure device is positioned on both sides of the hole in the heart, opens like an umbrella, and closes the defect. The procedure is generally performed under angiography and echocardiography guidance.
After non-surgical ASD closure, clot formation on the device may rarely occur. Therefore, blood-thinning medications are used for a certain period after the procedure and regular follow-ups are performed. With appropriate monitoring, the risk is quite low.
Non-surgical ASD closure may be recommended in childhood if there is heart enlargement, frequent infections, or decreased exercise capacity. Early intervention reduces the risk of future heart failure and rhythm disorders.
In patients who do not undergo non-surgical ASD closure, increased pulmonary pressure, heart enlargement, rhythm disorders, and heart failure may develop over time. In the long term, quality of life may decrease and serious cardiac problems may arise.
After non-surgical ASD closure, patients are generally discharged within 1–2 days. Return to daily life is possible within a few days. Heavy exercise should be avoided for the period recommended by the physician.
Non-surgical ASD closure can be safely performed in adult patients as well. However, in long-untreated cases with elevated pulmonary pressure, detailed evaluation is required. In suitable patients, the success rate is quite high.
Non-surgical ASD closure reduces cardiac load associated with increased blood volume during pregnancy. Performing the closure before pregnancy significantly lowers the risk of rhythm disorders and heart failure in the expectant mother.
Heavy activities are not recommended in the first weeks after non-surgical ASD closure. If follow-up is normal, most patients can gradually engage in sports. Cardiology evaluation is important for professional athletes.
Non-surgical ASD closure provides over 95% success in suitable patients. The device integrates with heart tissue over time and offers a permanent solution. Long-term results are generally satisfactory and quality of life improves.