Carotid artery disease (carotid artery stenosis) is a serious vascular condition that occurs due to narrowing or occlusion caused by atherosclerotic plaque accumulation in the carotid arteries located on both sides of the neck, reducing blood flow to the brain and increasing the risk of stroke. Early diagnosis and appropriate treatment are of vital importance.
Symptoms of carotid artery stenosis include transient ischemic attack, sudden vision loss, speech impairment, weakness and numbness in the face or extremities. These findings develop due to insufficient blood supply to brain tissue and may serve as warning signs before a permanent stroke.
The diagnosis of carotid artery disease is made through imaging methods such as Doppler ultrasonography, magnetic resonance angiography, and computed tomography angiography. The degree of narrowing in the vascular lumen is determined, the stage of the disease is identified, and treatment planning is carried out accordingly.
Treatment of carotid artery disease includes lifestyle modifications, medical approaches such as antiplatelet and statin therapy, and in cases of advanced stenosis, carotid endarterectomy or stent placement. The aim is to reduce the risk of cerebrovascular events and preserve brain perfusion.
What You Need to Know | Information |
Definition | Carotid artery disease is the narrowing or occlusion of the carotid arteries located on both sides of the neck and responsible for carrying blood to the brain, due to atherosclerosis (hardening of the arteries). This condition leads to reduced blood flow to the brain and an increased risk of stroke. |
Anatomy | The right and left common carotid arteries divide in the neck into the internal and external carotid arteries. The internal carotid artery carries blood to the brain and is the region most frequently associated with stroke. |
Causes | The most common cause is atherosclerosis. Risk factors include hypertension, diabetes, hyperlipidemia, smoking, obesity, sedentary lifestyle, advanced age, and family history. |
Risk Factors | Male gender, age over 65, presence of coronary artery disease, peripheral artery disease, high LDL cholesterol, low HDL cholesterol, and metabolic syndrome are important risk factors. |
Pathophysiology | Plaque forms as a result of lipid accumulation and inflammation in the vessel wall. As the plaque progresses, the vascular lumen narrows. Plaque rupture or thrombus formation on its surface may cause embolism by occluding cerebral vessels. |
Symptoms | It is usually asymptomatic in the early stage. When symptoms develop, transient ischemic attack (TIA) or stroke findings are observed: sudden loss of strength, speech impairment, facial asymmetry, vision loss or blurred vision, loss of balance. |
Transient Ischemic Attack (TIA) | Characterized by neurological symptoms that completely resolve within less than 24 hours. It is a serious warning sign for stroke. |
Diagnostic Methods | Carotid Doppler ultrasonography is the first-line imaging method. If necessary, CT angiography (CTA), MR angiography (MRA), or digital subtraction angiography (DSA) may be performed. |
Physical Examination | A carotid bruit may be heard in the neck. However, absence of a bruit does not exclude the disease. Neurological examination is important to assess stroke findings. |
Staging | Classified according to the percentage of stenosis: mild (<50%), moderate (50–69%), severe (≥70%). Clinical decisions are generally based on the degree of stenosis and the presence of symptoms. |
Complications | The most important complication is ischemic stroke. Permanent neurological deficits, cognitive impairment, and rarely death may also occur. |
Medical Treatment | Antiplatelet drugs (for example acetylsalicylic acid), statins, antihypertensive therapy, and blood glucose control are the main approaches. Lifestyle modifications are an important part of treatment. |
Surgical Treatment | Carotid endarterectomy is the preferred surgical method in certain degrees of stenosis, especially in symptomatic patients. The plaque is surgically removed. |
Endovascular Treatment | Carotid artery stenting may be applied as an alternative to surgery. It is particularly preferred in patients with high surgical risk. |
Treatment Indications | Interventional treatment may be considered in symptomatic patients with ≥50% stenosis. In asymptomatic patients with ≥70% stenosis, evaluation is made according to patient characteristics. |
Prevention | Smoking cessation, regular exercise, healthy nutrition, control of cholesterol and blood pressure, and diabetes management reduce disease progression. |
Prognosis | With early diagnosis and appropriate treatment, the risk of stroke can be significantly reduced. The risk of stroke is high in untreated severe stenosis. |
Follow-Up | The degree of stenosis is monitored with Doppler ultrasonography at regular intervals. Adherence to medical treatment and control of risk factors determine long-term outcomes. |

Prof. Dr. Kadriye Kılıçkesmez
Cardiology, Interventional Cardiologist – Interventional Cardiologist
Prof. Dr. Kadriye Orta Kılıçkesmez is one of the leading names in the field of Turkish cardiology. She was born on January 24, 1974, in Tekirdağ. After completing her undergraduate education at Istanbul University Cerrahpaşa Faculty of Medicine, she chose cardiology as her specialty and received her specialist training at the Cardiology Institute of the same university.
After working for a short period at Çorlu State Hospital and Turkish Kidney Foundation Service Hospital, she returned to the I.U. Cardiology Institute. Continuing her academic career there, Kadriye Kılıçkesmez became an associate professor in 2012. She then worked at Royal Brompton on complex coronary interventions, CTO intracoronary imaging, and structural heart diseases, and wrote scientific articles. In 2015, she was appointed by the university to establish the Şişli Etfal cardiology clinic and Angio laboratory. Becoming a professor in 2017, Kadriye Kılıçkesmez established the cardiology clinic and Angio laboratory of Prof. Dr. Cemil Taşçıoğlu Hospital in 2020 and ensured that the clinic became a training clinic.
View MoreWhat Is Carotid Artery Disease?
The carotid arteries are large vessels located on both sides of the neck that carry blood to the brain. Medically known as the arteria carotis communis, these vessels are branches of the main artery (aorta) emerging from the heart and ascend upward, dividing near the brainstem into two branches: the internal carotid artery (which carries blood to the inner parts of the brain) and the external carotid artery (which carries blood to the face, scalp, and other regions of the neck).
Carotid artery disease is the narrowing or complete occlusion of these vessels due to plaque accumulation (atherosclerosis) in their walls. These plaques are usually composed of cholesterol, fat, calcium, and other substances. Plaque accumulation may progressively obstruct blood flow over time. In addition, the surface of these plaques may become rough, and clots forming on them may detach and travel to the brain. These clots can block smaller vessels in the brain, leading to ischemic stroke. Stroke occurs when brain tissue is damaged due to lack of oxygen and nutrients.
According to data from the World Health Organization (WHO), stroke is the second leading cause of death worldwide and one of the most common causes of disability. For example, in 2019, approximately 12.2 million new stroke cases were reported, and 6.5 million of these cases resulted in death. Carotid artery disease is responsible for a significant portion of these cases.
Atherosclerosis and Plaque Formation
Atherosclerosis is a chronic disease characterized by the accumulation of cholesterol and other substances in the inner walls of arteries. This buildup hardens over time and forms structures called plaques. The process of plaque formation includes the following steps:
- Endothelial Injury: It begins with damage to the endothelial layer lining the inner surface of the artery wall. Factors such as smoking, high blood pressure, high cholesterol, and diabetes may cause this damage.
- Lipid Accumulation: Low-density lipoprotein (LDL) cholesterol passes through the damaged endothelial layer, enters the vessel wall, and becomes oxidized.
- Inflammation: The immune system initiates an inflammatory response to this foreign substance. Immune cells called macrophages ingest oxidized LDL, forming foam cells.
- Plaque Formation: Foam cells and other substances accumulate to form plaques. These plaques grow over time and narrow the vessel.
- Plaque Stabilization or Rupture: The surface of plaques may be smooth and stable or rough and unstable (prone to rupture). Unstable plaques carry a higher risk of clot detachment and vascular occlusion.
Plaque accumulation in the carotid arteries leads to serious consequences by reducing or completely blocking blood flow to the brain. This condition may result in transient ischemic attack (TIA) or stroke.
Causes and Risk Factors of Carotid Artery Disease
Multiple factors play a role in the development of carotid artery disease. The most important cause is atherosclerosis. However, atherosclerosis itself develops as a result of the combination of various risk factors. Understanding these risk factors is critical for prevention and early diagnosis.
Main Risk Factors
- Age: The risk of developing atherosclerosis increases with age. It is more common in individuals over 50.
- Gender: It tends to occur earlier and more frequently in men than in women. However, after menopause, this risk in women equals or exceeds that in men.
- Family History: Individuals with a family history of early heart or vascular disease (especially stroke or heart attack) have a higher risk.
- High Blood Pressure (Hypertension): Uncontrolled high blood pressure damages vessel walls and accelerates the atherosclerosis process. Worldwide, hypertension is one of the leading risk factors for heart disease and stroke. Approximately 1 billion people worldwide have hypertension.
- High Cholesterol (Hyperlipidemia): Especially high LDL (bad cholesterol) levels and low HDL (good cholesterol) levels trigger plaque formation. High cholesterol is responsible for approximately 20% of heart diseases worldwide.
- Diabetes: Diabetes damages blood vessels and worsens atherosclerosis. Uncontrolled blood glucose levels cause loss of elasticity in vessel walls and plaque accumulation.
- Smoking: Smoking damages vessel walls, increases blood clotting tendency, and raises blood pressure. It is one of the leading causes of preventable deaths worldwide and causes more than 8 million deaths annually.
- Obesity: Excess weight increases the risk of high blood pressure, high cholesterol, and diabetes, indirectly raising the risk of carotid artery disease.
- Physical Inactivity: Lack of regular exercise may lead to weight gain and increased blood pressure and cholesterol levels.
- Unhealthy Diet: Diets high in saturated fats, trans fats, salt, and sugar increase the risk of atherosclerosis.
- Atrial Fibrillation (AF): A condition in which the upper chambers of the heart beat irregularly and rapidly. AF may cause clot formation in the heart, and these clots traveling to the brain significantly increase stroke risk. AF affects approximately 33 million people worldwide.
Many of these risk factors can be controlled or managed through lifestyle changes. Therefore, knowing these factors and taking steps to reduce them is crucial in preventing carotid artery disease.
Specific Conditions Leading to Carotid Artery Disease
- Trauma: Blows to the neck region or surgical interventions may cause damage to the carotid arteries.
- Fibromuscular Dysplasia (FMD): A rare vascular disease that causes abnormal cell growth in artery walls, leading to narrowing, enlargement, or tears. It may also affect the carotid arteries.
- Arteritis: Inflammation of the vessels. Conditions such as Takayasu arteritis or giant cell arteritis may involve the carotid arteries and cause narrowing.
Symptoms of Carotid Artery Disease
Carotid artery disease usually does not cause symptoms until the narrowing reaches a certain level. This silent progression makes the disease more dangerous. Symptoms generally appear when blood flow to the brain is significantly reduced or when a plaque breaks off and sends a clot to the brain. These conditions manifest as transient ischemic attack (TIA) or stroke.
Symptoms of Transient Ischemic Attack (TIA)
TIA, also known as a “mini-stroke,” occurs due to a temporary interruption of blood flow to the brain. Symptoms usually last from a few minutes to one hour and resolve completely. However, TIA is an important warning sign for a future stroke; approximately 15% of individuals who experience TIA have a stroke within one year. TIA symptoms may include:
- Sudden speech impairment: Difficulty finding words, speaking incoherently, or inability to understand speech.
- Sudden vision loss: Temporary blindness in one or both eyes, blurred or double vision.
- Sudden weakness or numbness: Sudden loss of strength or sensation on one side of the body (face, arm, or leg), often unilateral.
- Sudden loss of balance or coordination: Difficulty walking, dizziness, lightheadedness.
- Sudden severe headache: Sudden and severe headache without a clear cause.
Symptoms of Stroke
Stroke symptoms are similar to TIA symptoms but are more severe and cause permanent damage. Stroke symptoms occur suddenly and require urgent medical intervention. The FAST (Face-Arm-Speech-Time) rule is an effective method to recognize stroke symptoms:
- F (Face): Ask the person to smile. Does one side of the face droop?
- A (Arm): Ask the person to raise both arms. Does one arm drift downward?
- S (Speech): Ask the person to repeat a simple sentence. Is speech slurred, unclear, or strange?
- T (Time): If any of these signs are present, call emergency services immediately. Time is critical to save brain tissue.
Other possible stroke symptoms may include:
- Sudden numbness or weakness on one side of the body.
- Sudden confusion, difficulty understanding or speaking.
- Sudden vision problems in one or both eyes.
- Sudden difficulty walking, dizziness, loss of balance or coordination.
- Sudden and unexplained severe headache.
If you or someone near you experiences any of these symptoms, seek emergency medical attention without delay. Timing is vital in stroke treatment.
Diagnosis of Carotid Artery Disease
The diagnosis of carotid artery disease is made through a combination of the patient’s medical history, physical examination, and various imaging methods. Early diagnosis significantly increases treatment success and reduces the risk of stroke.
Medical History and Physical Examination
The doctor will inquire about the patient’s general health status, existing conditions (such as hypertension, diabetes, high cholesterol), smoking habits, family history, and any previous history of stroke or TIA. During physical examination, the doctor may listen for an abnormal sound called a bruit over the carotid arteries in the neck. This bruit results from turbulent blood flow through a narrowed vessel. However, absence of a bruit does not mean there is no stenosis; in some cases of severe narrowing or complete occlusion, no bruit may be heard.
Imaging Methods
The main imaging methods used in diagnosis are as follows:
- Carotid Ultrasonography (Doppler Ultrasound): This is the most commonly used, painless, and harmless method in diagnosing carotid artery disease. Using sound waves, it visualizes vessel structure and blood flow velocity. This allows detection of the degree of stenosis (percentage of narrowing) and presence of plaques. Ultrasound may also provide information about plaque characteristics (for example, whether the plaque is stable).
- Computed Tomography Angiography (CT Angiography): In this method, contrast material is injected into the body followed by a CT scan. CT angiography provides detailed three-dimensional images of the carotid arteries and shows stenoses, occlusions, and plaques with high accuracy. It is particularly used to determine the degree of stenosis and for surgical planning.
- Magnetic Resonance Angiography (MR Angiography): Similar to CT angiography, MR angiography is used to obtain detailed images of vessels. This method uses magnetic fields and radio waves and therefore does not involve radiation. MR angiography may provide additional information about plaque structure and possible brain tissue damage.
- Conventional Angiography (Seldinger Technique): This is an invasive method and is generally preferred when a definitive diagnosis cannot be made with other methods or when treatment (stent or surgery) is planned. A catheter (thin tube) is inserted through the groin and advanced to the carotid artery, then contrast material is injected and X-ray images are taken. This method most accurately determines the location and degree of stenosis but carries higher risks.
Brain MRI and Computed Tomography (CT)
These imaging methods do not directly visualize the carotid arteries but are used to determine the extent and location of brain damage in patients who have experienced a stroke. They may also detect other vascular problems in the brain or other conditions causing stroke.
Additional Tests
- Electrocardiogram (ECG): Used to detect heart rhythm disorders (for example atrial fibrillation), which may increase stroke risk.
- Echocardiography (ECHO): Used to evaluate heart structure and function. It may help determine the risk of clots in the heart traveling to the brain.
- Blood Tests: Performed to check values such as cholesterol, blood glucose, and coagulation factors.
The doctor will determine the most appropriate diagnostic methods according to the patient’s condition. Early and accurate diagnosis is essential for establishing an effective treatment plan.
Treatment of Carotid Artery Disease
Treatment of carotid artery disease is determined based on factors such as the patient’s overall health status, degree of stenosis, presence of symptoms, and risk of stroke. The main goal of treatment is to ensure adequate blood flow to the brain, stabilize plaques, and minimize the risk of stroke.
Treatment approaches are generally grouped under two main categories: medical treatment (drug therapy) and surgical/interventional treatment.
Medical Treatment (Drug Therapy)
Medical treatment is the fundamental approach in all patients, including those undergoing surgical or interventional procedures. The aim is to slow the progression of atherosclerosis, stabilize plaques, and prevent blood clot formation.
- Antiplatelet Drugs: Medications such as aspirin and clopidogrel prevent platelets from aggregating and forming clots. These drugs are highly effective in reducing stroke risk in patients with carotid artery disease, especially those with symptoms. For example, aspirin may reduce clot formation by 20–30%.
- Statins (Cholesterol-Lowering Drugs): Statins such as atorvastatin and rosuvastatin lower blood cholesterol levels, helping plaques shrink or stabilize. They also have anti-inflammatory effects and protect vessel walls, slowing the progression of atherosclerosis. Statins may reduce the risk of heart attack and stroke by approximately 25%.
- Antihypertensive Drugs: Controlling high blood pressure reduces vessel wall damage and slows the progression of atherosclerosis. ACE inhibitors, beta blockers, and calcium channel blockers may be used.
- Antidiabetic Drugs: In diabetic patients, maintaining blood glucose control is critical for vascular health.
- Lifestyle Modifications: Quitting smoking, healthy eating, regular exercise, and weight control are integral parts of medical treatment and enhance its effectiveness.
Surgical and Interventional Treatments
In patients at high risk of stroke despite medical treatment or in those with severe stenosis (generally 70% or more), surgical or interventional methods may be considered.
- Carotid Endarterectomy (CEA): This is the surgical removal of plaque from the carotid artery in the neck. During surgery, the carotid artery is opened, the plaque material inside is carefully removed, and the artery is sutured again. CEA significantly reduces stroke risk. In stenosis of 70% or more and in symptomatic patients, it may reduce stroke risk by about 25%. This operation has been successfully performed millions of times worldwide.
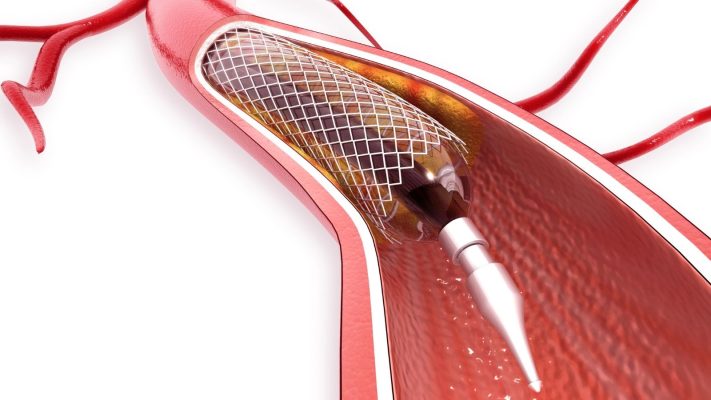
- Carotid Angioplasty and Stenting (CAS): This is a less invasive method. A catheter (thin tube) is inserted through the groin artery and advanced to the carotid artery. A balloon is placed at the narrowed area and inflated to widen the vessel (angioplasty). Then, a stent (a metal mesh tube) is placed to prevent re-narrowing. CAS may be preferred especially in patients with high surgical risk or certain anatomical conditions. CAS may provide results similar to CEA, but the long-term risk of clot formation within the stent may be higher.
Treatment selection should be made by a multidisciplinary team (neurologist, cardiovascular surgeon, interventional radiologist) considering the individual condition of the patient.
Ways to Prevent Carotid Artery Disease
Carotid artery disease is largely preventable. Awareness of risk factors and making lifestyle changes accordingly play a critical role in preventing or slowing disease progression. Healthy lifestyle habits help protect not only against carotid artery disease but also against heart disease, other types of stroke, and many chronic conditions.
Lifestyle Changes and Preventive Measures
- Quit Smoking: Smoking is one of the most harmful factors for vascular health. Quitting smoking reduces inflammation in vessels, decreases blood clotting tendency, and helps control blood pressure. Within the first year after quitting smoking, the risk of heart attack decreases by 50%.
- Healthy Nutrition: Adopting a diet low in saturated fat, trans fat, cholesterol, salt, and sugar is important. Consuming plenty of fruits, vegetables, whole grains, and healthy fats (such as olive oil and fish oil) supports vascular health. Dietary models such as the Mediterranean diet have positive effects on cardiovascular health.
- Regular Physical Activity: At least 150 minutes of moderate-intensity or 75 minutes of high-intensity aerobic exercise per week is recommended. Exercise helps control weight, lowers blood pressure, improves cholesterol levels, and supports overall vascular health.
- Maintain a Healthy Body Weight: Obesity increases risk factors such as high blood pressure, diabetes, and high cholesterol. Losing weight or maintaining a healthy weight reduces these risks.
- Control Blood Pressure: If you have high blood pressure, use medications regularly as prescribed and apply lifestyle modifications. The target is to maintain blood pressure below 130/80 mmHg.
- Manage Cholesterol Levels: If you have high cholesterol, controlling it with diet and medication is important. Maintaining LDL cholesterol at target levels slows the progression of atherosclerosis.
- Control Diabetes: If you have diabetes, regularly monitor blood glucose levels and adhere to treatment. Good glycemic control helps prevent vascular damage.
- Limit Alcohol Consumption: Excessive alcohol intake may raise blood pressure and cause weight gain. Keeping alcohol consumption at moderate levels is important.
Regular Health Check-Ups
If you have risk factors or are over the age of 50, regular medical check-ups are important. Your doctor can detect potential problems early by monitoring blood pressure, cholesterol levels, and blood glucose. If necessary, screenings such as carotid ultrasound may be performed.
Approach in Asymptomatic Patients
Even if carotid artery disease does not cause symptoms, if the degree of stenosis is high (for example 70% or more) and the patient has other risk factors, stroke risk is high. In these patients, lifestyle modifications and medical therapy (antiplatelets, statins) are applied. In some cases, surgical or stent treatment may also be considered.
Preventive measures and regular health check-ups enable early diagnosis and effective management of carotid artery disease, significantly reducing the risk of stroke.
Frequently Asked Questions
Plaques formed in the carotid arteries narrow the vessel lumen and reduce blood flow to the brain. In addition, plaque fragments may detach and block cerebral vessels, causing sudden stroke.
Smoking, hypertension, diabetes, and high cholesterol are the most important risk factors. Advanced age, obesity, and a family history of vascular disease also increase disease risk by accelerating plaque formation.
Genetic predisposition, familial hyperlipidemia, and uncontrolled diabetes may cause damage to the vessel wall at a young age. Heavy smoking and unhealthy nutrition may also trigger early plaque development.
Symptoms such as transient vision loss, speech impairment, and sudden weakness in the face or arm may indicate a transient ischemic attack. Even if these symptoms are brief, they are warning signs of serious stroke risk.
Most commonly, Doppler ultrasonography is used to evaluate intravascular stenosis. When necessary, CT angiography or MR angiography is used to examine plaque structure and degree of stenosis in more detail.
Surgery is recommended in patients with severe stenosis and a history of stroke. Carotid endarterectomy or stent placement aims to reduce stroke risk by increasing blood flow to the brain.
Most patients are discharged within a few days. Blood pressure control and regular medication use are important in the first weeks. Full recovery time varies depending on the patient’s overall health status.
If left untreated, recurrent transient attacks and permanent stroke may develop. In advanced cases, loss of consciousness and serious decline in quality of life may occur.
Quitting smoking, following a diet low in salt and saturated fat, and engaging in regular exercise protect vascular health. Controlling blood pressure, blood glucose, and cholesterol levels slows disease progression.
Fear of stroke and sudden events may cause anxiety in patients. Regular follow-up and proper information reduce uncertainty and improve treatment adherence and quality of life.