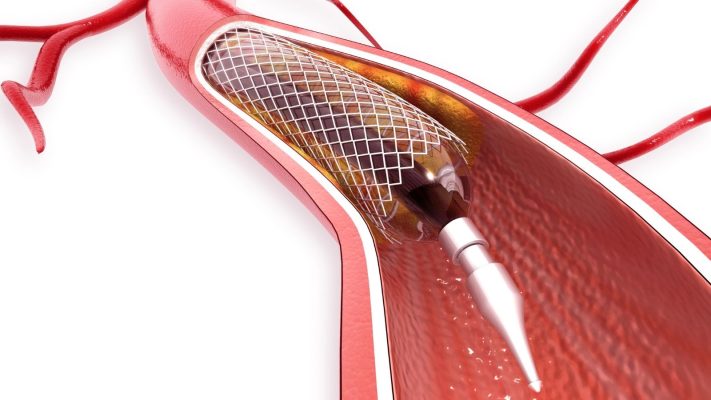
Interventional treatment of peripheral artery disease is a minimally invasive method that enables narrowed or occluded arteries to be reopened using balloon angioplasty and stent placement. This technique aims to increase blood flow, thereby reducing pain, walking limitation, and the risk of tissue loss.
Balloon angioplasty is based on the principle of mechanically expanding the atherosclerotic plaque within the vessel. The balloon placed via a catheter is inflated in a controlled manner to open the vessel lumen and improve peripheral circulation. The procedure is generally performed under local anesthesia.
Peripheral artery stenoses requiring stent placement are preferred in cases of elastic recoil or the presence of advanced plaque. Metal or drug-eluting stents provide support to the vessel wall, reduce the risk of re-narrowing, and aim to maintain long-term vessel patency.
The follow-up process after interventional treatment includes regulation of antiplatelet therapy and control of risk factors. Smoking cessation, lipid level regulation, and diabetes management increase treatment success. Regular clinical and imaging follow-ups reduce the risk of complications.
What You Need to Know | Information |
Definition | Interventional treatment of peripheral artery disease refers to minimally invasive endovascular procedures aimed at reopening narrowed or occluded peripheral arteries (most commonly lower extremity arteries) through balloon angioplasty and/or stent placement. |
Purpose | To increase blood flow, reduce rest pain, extend walking distance, prevent tissue loss, and reduce the risk of limb loss. |
Indications | Persistent intermittent claudication despite lifestyle changes and medical therapy, rest pain, non-healing wounds or gangrene (critical limb ischemia), and significant arterial stenosis or occlusion detected by imaging. |
Contraindications | Active infection, uncontrolled bleeding diathesis, severe contrast material allergy, inability to obtain suitable vascular access, or a general condition of the patient that cannot tolerate the procedure. |
Pre-Procedure Evaluation | Detailed history and physical examination, ankle-brachial index (ABI), Doppler ultrasonography, CT angiography or MR angiography; evaluation of renal function tests and coagulation parameters. |
Type of Anesthesia | Usually performed under local anesthesia and sedation; rarely, general anesthesia may be required. |
Procedure Process | A catheter is inserted via the femoral artery (or alternatively radial/brachial artery), advanced to the stenotic area with a guidewire, the vessel is dilated by inflating a balloon; a stent is placed if necessary. |
Balloon Angioplasty | The procedure of pushing the atherosclerotic plaque toward the vessel wall and expanding the lumen by controlled inflation of a balloon catheter placed at the site of stenosis. |
Drug-Coated Balloon | Use of balloons coated with antiproliferative drugs (for example paclitaxel) to reduce the risk of restenosis; may be preferred especially in long-segment stenoses. |
Stent Placement | In vessels with elastic recoil or dissection, a metal mesh stent is placed to maintain vessel patency. Self-expanding or balloon-expandable stent types are available. |
Procedure Duration | Generally varies between 30–120 minutes depending on the length and number of lesions. |
Length of Hospital Stay | Most patients are discharged the same day or within 1 day; the duration may be prolonged in the presence of complications. |
Success Rates | Depends on the location and length of the lesion and the patient’s comorbidities; technical success rates are high in short and focal lesions. Success and patency rates are lower in long-segment and calcified lesions. |
Possible Complications | Bleeding, hematoma, pseudoaneurysm, vessel perforation, dissection, thrombosis, distal embolization, contrast nephropathy, allergic reaction. |
Restenosis | Re-narrowing may develop within the vessel over time; the risk depends on lesion characteristics and the patient’s risk factors. |
Post-Procedure Follow-Up | Antiplatelet therapy (usually acetylsalicylic acid and/or clopidogrel), regular clinical follow-up, ABI measurement, and monitoring with Doppler ultrasonography if necessary. |
Lifestyle Modifications | Smoking cessation, regular exercise program, healthy diet, and effective control of diabetes, hypertension, and hyperlipidemia. |
Alternative Treatments | Medical therapy and exercise programs, open surgical bypass operation; treatment selection is determined according to lesion characteristics and the patient’s overall condition. |
Prognosis | With early diagnosis and appropriate treatment, significant improvement in symptoms can be achieved; long-term success depends on control of risk factors and regular follow-up. |

Prof. Dr. Kadriye Kılıçkesmez
Cardiology, Interventional Cardiologist – Interventional Cardiologist
Prof. Dr. Kadriye Orta Kılıçkesmez is one of the leading names in the field of Turkish cardiology. She was born on January 24, 1974, in Tekirdağ. After completing her undergraduate education at Istanbul University Cerrahpaşa Faculty of Medicine, she chose cardiology as her specialty and received her specialist training at the Cardiology Institute of the same university.
After working for a short period at Çorlu State Hospital and Turkish Kidney Foundation Service Hospital, she returned to the I.U. Cardiology Institute. Continuing her academic career there, Kadriye Kılıçkesmez became an associate professor in 2012. She then worked at Royal Brompton on complex coronary interventions, CTO intracoronary imaging, and structural heart diseases, and wrote scientific articles. In 2015, she was appointed by the university to establish the Şişli Etfal cardiology clinic and Angio laboratory. Becoming a professor in 2017, Kadriye Kılıçkesmez established the cardiology clinic and Angio laboratory of Prof. Dr. Cemil Taşçıoğlu Hospital in 2020 and ensured that the clinic became a training clinic.
View MorePeripheral Artery Disease: The Silent Threat and Its Symptoms
Peripheral artery disease (PAD) is the narrowing or blockage of the arteries in the arms and legs. This narrowing usually occurs due to atherosclerosis (hardening of the arteries). Atherosclerosis is the accumulation of fat, cholesterol, and other substances on the vessel walls, forming plaque. Over time, these plaques can grow and obstruct blood flow. As a result, sufficient oxygen and nutrients cannot reach the affected limbs. This condition can cause pain, cramping, fatigue, and even ulcers, especially in the legs. Factors such as smoking, diabetes, high blood pressure, high cholesterol, and a family history of PAD increase the risk. Early diagnosis and treatment are vital to stop disease progression and prevent limb loss. Many patients may not show clear symptoms in the early stages of the disease, which is why it is referred to as a “silent threat.” However, as the disease progresses, symptoms become more pronounced.
What Are the Symptoms?
The most common symptom of PAD is cramp-like pain felt in the legs during walking. This pain subsides with rest but reappears with activity. In medical literature, this condition is called intermittent claudication. Other common symptoms include:
- Fatigue and Heaviness in the Legs: Especially felt during activity.
- Skin Changes: Coldness, paleness, shininess, hair loss, or thickening of the nails may be observed in the feet and legs.
- Delayed Wound Healing: Small cuts, abrasions, or ulcers on the feet or legs may heal slowly.
- Erectile Dysfunction: In men, sexual dysfunction may occur if the arteries in the pelvic region are affected.
- Advanced Stage Symptoms: In advanced stages of the disease, leg pain may occur even at rest, night cramps may develop, and even gangrene (tissue death) may occur. Gangrene is a serious condition that can lead to limb loss.
What Are the Risk Factors?
There are many factors that increase the risk of developing PAD. The most important among them is smoking. Smoking damages the vessel walls and accelerates the development of atherosclerosis. Diabetes is also a significant risk factor; high blood sugar levels can damage the vessels. High blood pressure (hypertension) and high cholesterol (hyperlipidemia) also contribute to the progression of atherosclerosis. The risk increases with advancing age; it is more commonly seen in individuals over 50 years of age. In addition, having a family history of PAD may indicate genetic predisposition. Obesity and a sedentary lifestyle also indirectly increase the risk. Managing these risk factors plays a critical role in preventing PAD or slowing its progression.
Interventional Treatments: Balloon Angioplasty and Stent
Non-surgical, minimally invasive methods are gaining increasing importance in the treatment of PAD. Among these methods, the most commonly used are balloon angioplasty and stent placement. These procedures can be performed under local anesthesia without the need for general anesthesia and usually require only a one-day hospital stay. This is a significant advantage compared to traditional surgery. The procedures are generally performed by advancing a thin catheter (tube) through an artery in the groin or arm. This catheter is used to reach the narrowed or blocked area. The success of the procedures depends on many factors such as the patient’s general health condition and the location and severity of the narrowing.
Balloon Angioplasty: The Art of Opening Narrowed Arteries
Balloon angioplasty is a technique used to widen a narrowed artery. During the procedure, a thin guidewire is placed into the narrowed arterial segment. Over this wire, a special catheter with an inflatable balloon at its tip is advanced. After the balloon is positioned within the narrowed artery, it is carefully inflated. This inflation pushes the arterial wall outward, widening the narrowed area and restoring blood flow. After the balloon is deflated and the catheter is removed, the artery is observed to be more open. Balloon angioplasty may be sufficient on its own or is often used together with stent placement. After a successful balloon angioplasty, the patient’s walking distance may increase and leg pain may decrease. The effectiveness of this procedure varies depending on how severely the artery is narrowed and the structure of the plaques. In some cases, the artery may narrow again after balloon angioplasty (restenosis). In such cases, stents come into play to prevent this condition.
Stent Placement: Providing Support to the Arteries
A stent is a small, tube-shaped metal structure placed to keep a narrowed artery open. Stents are generally made of memory alloys such as nickel-titanium. After the artery is widened with balloon angioplasty, the stent is placed in this area. The stent is expanded with the help of a balloon catheter and fixed to the artery wall. The stent prevents the artery from narrowing again and ensures continuous blood flow. Some stents release medication to further reduce the risk of restenosis (drug-eluting stents). The choice of stent is determined by the physician according to the patient’s condition and the characteristics of the narrowing. Stents play a critical role in maintaining long-term patency by supporting the structure of the artery. Stent placement can be performed together with balloon angioplasty or alone. After the procedure, the stent is gradually covered by the body and becomes a natural part of the vessel.
Procedure Process and Preparation
Interventional treatment of peripheral artery disease requires careful preparation and meticulous application. Before the procedure, the patient’s overall health status is evaluated, necessary blood tests are performed, and medications are reviewed. On the day of the procedure, patient comfort and safety are prioritized. In the post-procedure period, the patient’s recovery process is closely monitored. During this period, the medications to be taken and lifestyle changes are of great importance.
Pre-Procedure Evaluation and Preparations
Before deciding on interventional treatment, it is essential for the patient to undergo a comprehensive medical evaluation. The physician reviews the patient’s medical history in detail, questions existing diseases (diabetes, heart disease, kidney disease, etc.) and medications used. Peripheral pulses are checked with physical examination and the condition of the affected limbs is evaluated. Various imaging methods are used to support the diagnosis and determine the location, length, and severity of the narrowing. These include Doppler ultrasonography, Magnetic Resonance Angiography (MRA), and Computed Tomography Angiography (CT angiography). In some cases, Digital Subtraction Angiography (DSA) may also be performed for procedure planning. Blood tests are requested to evaluate kidney functions, coagulation status, and the presence of infection. A few days before the procedure, the use of blood-thinning medications (for example aspirin, clopidogrel) may be adjusted or temporarily discontinued under physician supervision. The patient may be required to fast the night before the procedure. Psychological support may also be provided to ensure the patient is comfortable and calm on the day of the procedure. Pre-procedure preparations form the basis for completing the procedure safely and successfully.
Steps Followed During the Procedure
Interventional treatment is generally performed in a catheter laboratory or hybrid operating room. The procedure is carried out under local anesthesia, allowing the patient to remain awake. The procedure usually begins with a small incision in an artery in the groin area (femoral artery) or sometimes in an artery in the arm (brachial artery). A thin needle is inserted into this incision site and a guidewire is placed into the artery. This wire is advanced along the vessel to reach the area of narrowing or blockage. Then, a balloon catheter and/or stent catheter is placed over this guidewire. If balloon angioplasty is to be performed, the balloon catheter is positioned at the narrowing site and the balloon is inflated in a controlled manner to widen the vessel. If a stent is to be placed, the stent catheter is positioned at the narrowing site and the stent is expanded with the help of a balloon and fixed to the vessel wall. Continuous X-ray imaging (fluoroscopy) is used during the procedure to monitor the position of the catheters and stents. When necessary, contrast material is injected to visualize the vessels. After the procedure is completed, the catheters are removed and bleeding control is achieved by applying pressure to the incision site or using special devices. The procedure duration generally varies between 1 and 3 hours, but this may differ depending on the complexity of the intervention. Patient comfort and safety are prioritized at every stage of the procedure.
Post-Procedure Care and Recovery Process
The post-procedure period is of great importance for the patient to have a successful recovery. After the procedure, patients are usually kept under observation for several hours. Due to the risk of bleeding at the incision site, the patient may need to remain on bed rest for a certain period and avoid bending the leg. Appropriate pain relievers are administered for pain control. Hydration is ensured and returning to a normal diet as soon as possible is encouraged. Blood-thinning medications are generally prescribed for long-term use to prevent stents from becoming blocked by clots. Medications such as aspirin and clopidogrel are frequently used together. Regular use of the medications recommended by the physician is vital. Patients are informed about recognizing signs of complications such as infection (fever, redness, swelling, discharge) or bleeding (bleeding from the incision site, bruising). Generally, patients can return to normal activities within a few days to one week. However, avoiding heavy physical activities and sports is recommended. Regular physician follow-ups are critical to monitor the recovery process and detect potential problems early. Lifestyle changes such as quitting smoking, eating a healthy diet, and exercising regularly provide significant long-term benefits in preventing recurrence of the disease and improving overall health.
Advantages and Risks
Although interventional treatments offer many advantages compared to traditional surgery, they also carry certain risks as with any medical procedure. Knowing these advantages and risks helps patients make informed decisions. Physicians determine the most appropriate treatment method by evaluating each patient’s specific condition.
Advantages of Interventional Treatment
Interventional treatments, especially balloon angioplasty and stent placement, have provided significant advances in the treatment of PAD. The main advantages of these methods are as follows:
- Minimally Invasive: Performed with much smaller incisions compared to open surgery, meaning less pain and faster recovery. Hospital stay is generally shorter; most patients can be discharged after 1–2 days.
- Lower Risk of Complications: Since general anesthesia is not required and smaller incisions are used, the risk of surgery-related complications such as infection, bleeding, and wound healing problems is lower.
- Rapid Recovery Process: Patients can usually return to normal daily activities within a few days after the procedure. This allows quality of life to be regained quickly.
- Repeatability: If necessary, angioplasty or stent placement procedures can be applied again to the same area. This is an important advantage especially in cases of disease recurrence.
- High Success Rates: Especially in appropriate patients, these methods have high success rates in ensuring vessel patency and relieving symptoms. Long-term patency rates can reach 80–90% depending on the technology used and patient care.
- Limb Salvage Potential: In advanced cases such as critical limb ischemia (severely reduced blood flow to the limbs), these interventional methods can play a critical role in preventing limb loss.
Possible Risks and Complications
Although safe and effective, balloon angioplasty and stent placement procedures carry certain risks. These risks are generally low but important to know:
- Bleeding and Hematoma: Bleeding or bruising (hematoma) may occur at the procedure site. This is usually mild and resolves spontaneously, but rarely may require blood transfusion or additional intervention.
- Vessel Damage: During advancement of the catheter, damage such as tearing, perforation, or dissection (separation of vessel wall layers) may occur. These conditions may rarely require surgical intervention.
- Restenosis (Re-narrowing): Re-narrowing may develop over time at the site where the stent is placed. This results from excessive tissue growth inside the stent. Drug-eluting stents help reduce this risk.
- Stent Thrombosis (Clot Formation in the Stent): A rare but serious complication. A clot may form inside the stent and obstruct blood flow. This risk increases particularly if blood-thinning medications are not used regularly.
- Infection: Infection may develop at the procedure site or around the stent. This risk is minimized by using sterile techniques.
- Contrast Material Reactions: Allergic reactions to the contrast material used during the procedure or temporary impairment in kidney function may occur. Special precautions are taken in patients with kidney failure.
- Peripheral Artery Spasm: Temporary contraction (spasm) of the artery may occur during advancement of the catheter within the vessel. This is usually controlled with medication.
- Nerve Damage: Rarely, temporary or permanent numbness or weakness may occur due to involvement of nerves in the procedure area.
These risks are generally low, and physicians take all precautions to minimize them. It is important to discuss these risks in detail with your doctor before the procedure.
Medication Therapy and Lifestyle Changes
Although interventional treatments play an important role in PAD management, they are not sufficient on their own. Medication therapy and lifestyle changes are indispensable for stopping disease progression, preventing complications, and improving overall health. These approaches reinforce the success of interventional treatment and support the patient’s long-term health.
The Role of Medication Therapy
In PAD treatment, medications are used to relieve symptoms, slow disease progression, and reduce the risk of complications. The medications prescribed by your doctor may include:
- Antiplatelet Agents (Blood Thinners): Medications such as aspirin and clopidogrel prevent platelets from clumping together to form clots. This is especially vital in patients with stents to prevent stent thrombosis. They are generally used lifelong.
- Statins: Cholesterol-lowering medications. They lower LDL (“bad”) cholesterol levels, slow the progression of atherosclerosis, and help stabilize plaques on vessel walls. They are generally prescribed at high doses in high-risk patients.
- Antihypertensives (Blood Pressure Medications): Used to control high blood pressure. Keeping blood pressure within normal levels protects vascular health and reduces the risk of heart attack and stroke.
- Diabetes Medications: In patients with diabetes, maintaining blood glucose levels under control is critical to prevent vascular damage. Insulin or various oral diabetes medications may be used.
- Pain Relievers: Used especially to manage claudication pain. However, long-term use of opioid painkillers is not recommended. Some medications such as cilostazol may help increase walking distance by improving blood flow to the leg muscles.
The success of medication therapy depends on the patient taking medications regularly and as prescribed by the doctor. It is important to stay in communication with the physician regarding possible side effects.
The Importance of Lifestyle Changes
Lifestyle changes are one of the cornerstones of PAD treatment and are usually implemented together with medication therapy. These changes not only slow disease progression but also significantly improve overall health:
- Quitting Smoking: The most important and most effective lifestyle change for PAD. Smoking causes severe damage to the vessels and accelerates disease progression. Quitting smoking positively changes the course of the disease and significantly reduces the risk of complications. Nicotine replacement therapies or counseling services may help in this process.
- Healthy Diet: Adopting a diet low in saturated fat, low in cholesterol, and low in sodium, rich in fruits, vegetables, and whole grains helps control blood cholesterol and blood pressure. Dietary models such as the Mediterranean diet are recommended.
- Regular Exercise: With the doctor’s approval, regular walking and exercise help strengthen leg muscles, improve blood circulation, and increase walking distance. The exercise program should be individually designed according to the patient’s condition and disease severity. Low-impact exercises such as swimming and cycling are also beneficial.
- Weight Control: Being overweight or obese increases the risk of high blood pressure, diabetes, and high cholesterol. Achieving and maintaining a healthy weight improves overall cardiovascular health.
- Diabetes and Blood Pressure Control: Effective management of diabetes and high blood pressure is essential to protect vascular health. The treatment recommended by the doctor should be followed to achieve blood glucose and blood pressure targets.
- Foot Care: Patients with PAD are more prone to infection due to loss of sensation or slow-healing wounds in their feet. Regular inspection of the feet, keeping them clean and dry, wearing appropriate footwear, and careful nail trimming are important. In case of wound formation, a doctor should be consulted immediately.
These lifestyle changes play a major role not only in the management of PAD but also in improving overall quality of life.
Future Technologies and Research
There is continuous development in the interventional treatment of peripheral artery disease. Scientists and engineers are working intensively to develop more effective, safer, and less invasive treatment methods. These innovations have the potential to further improve patients’ quality of life.
Next-Generation Stents and Materials
In addition to traditional metal stents, significant research is being conducted on biodegradable (absorbable) stents. These stents are gradually absorbed by the body over time and completely disappear, which may reduce the long-term risk of restenosis and stent thrombosis. In addition, drug-loaded stents coated with anticoagulant (anti-clotting) or anti-inflammatory medications are being developed. These drugs accumulate around the stent, suppress inflammation and cell proliferation, thereby reducing restenosis rates. New-generation coatings aim to reduce blood clotting by modifying the surface properties of stents. As an alternative to traditional metal stents, polymer-based stents are also being investigated. These stents may be more flexible and better adapt to the natural movements of the vessel.
Minimally Invasive Interventional Techniques
With advances in technology, even less invasive methods are being developed. Techniques such as rotational atherectomy mechanically fragment or remove plaques to clear the vessel. This can be especially useful in cases of hard and calcified plaques where balloon angioplasty and stent placement are difficult. Laser atherectomy uses laser energy to vaporize plaques. Ultrasonic and shockwave therapies are used to break calcifications in the vessel wall and widen the artery. These techniques may reduce the need for stents or facilitate stent placement. In addition, robotic surgical systems may allow surgeons to perform more precise and controlled movements, making procedures safer.
Biological Therapies and Gene Therapy Potential
In the long term, biological therapies and gene therapy also show promise in the treatment of PAD. Researchers aim to create new blood pathways around blocked arteries by using growth factors or proteins that promote new vessel formation (angiogenesis). Stem cell therapy is also being investigated as a potential approach to repair damaged vascular tissue and support the growth of new vessels. In gene therapy, the goal is to modify the genetic structure of vascular wall cells to prevent or reverse the development of atherosclerosis. Although these fields are still in the experimental stage, they have the potential to revolutionize PAD treatment in the future. Such therapies may open new doors of hope in cases where medications and stents are insufficient.
Frequently Asked Questions
Interventional treatment is applied in patients whose walking pain persists despite medication and exercise, who develop rest pain, or whose wound healing is impaired. If arterial narrowing is severe and quality of life is affected, it may be the primary option.
A thin catheter is advanced to the narrowed area through the groin or below the knee. The balloon is inflated to press the plaque against the vessel wall and increase blood flow. If necessary, a stent is placed to maintain vessel patency.
Smoking, diabetes, high cholesterol, and long-segment stenoses increase the risk of re-narrowing. Regular use of medications and lifestyle changes reduce the likelihood of in-stent narrowing.
Most patients are discharged the same day or the next day. The access site in the groin may be sensitive for a few days. Starting a walking program early contributes to improved circulation and long-term success.
The risk of complications may increase in individuals with advanced kidney failure, uncontrolled diabetes, widespread vascular calcification, and bleeding disorders. Therefore, a detailed evaluation is performed before the procedure.
After stent placement, blood-thinning and antiplatelet medications are generally prescribed. This therapy prevents clot formation within the stent and helps maintain vessel patency.
In advanced stages, restoring blood flow in patients with non-healing wounds increases tissue nourishment. In appropriate patients, timely intervention can significantly reduce the risk of amputation.
Smoking cessation, regular walking, weight control, and lowering cholesterol directly affect treatment success. These measures help prevent the development of new arterial narrowings.
In diabetic patients, vascular structure may be more diffuse and calcified. This may create technical challenges, but successful outcomes can be achieved with appropriate planning and follow-up.
After the procedure, Doppler ultrasound checks are performed at specific intervals. Increases in symptoms, decreased walking distance, or wound formation are evaluated early to detect possible re-narrowing in time.