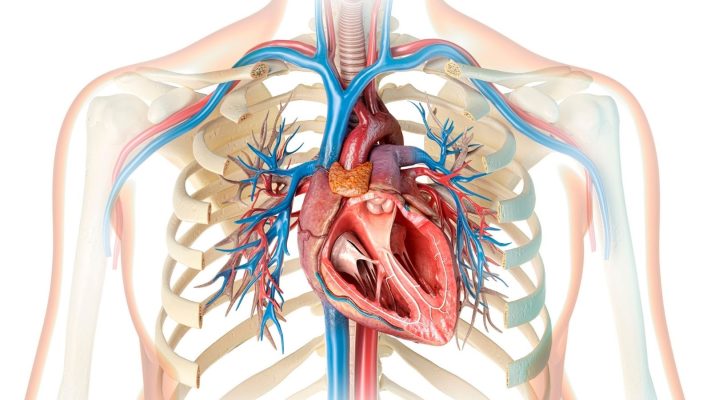
Chronic Total Occlusion (CTO) is an advanced vascular disease characterized by complete blockage of a coronary artery for at least three months. This condition leads to insufficient blood flow to the heart muscle and may cause clinical findings associated with myocardial ischemia.
Symptoms of chronic total occlusion most commonly present as chest pain that increases with exertion, shortness of breath, and decreased exercise capacity. In some patients, symptoms may be mild due to the development of collateral circulation; however, the underlying severe coronary artery disease persists.
The diagnosis of chronic total occlusion is definitively established by coronary angiography, where complete obstruction of the vessel lumen is visualized. Non-invasive imaging methods and stress tests play a complementary role in evaluating myocardial viability and ischemia.
Treatment of chronic total occlusion may include medical therapy, percutaneous coronary intervention, or coronary artery bypass surgery. The choice of treatment is determined according to the patient’s clinical condition, severity of symptoms, and anatomical features; the aim is symptom control and improvement of quality of life.
What You Need to Know | Information |
Definition | Chronic Total Occlusion (CTO) is the condition in which complete blockage of a coronary artery (heart vessel) persists for at least 3 months. This blockage usually occurs due to atherosclerotic plaque and superimposed thrombus. |
Prevalence | CTO can be detected in approximately 15–30% of patients undergoing coronary angiography. It is most commonly seen in the right coronary artery but can develop in all epicardial coronary arteries. |
Mechanism of Formation | As a result of atherosclerosis, plaque accumulates in the vessel wall. Over time, the plaque progresses and completely occludes the vessel lumen. In long-standing occlusion, a fibrotic and calcified structure develops in the vessel segment. |
Risk Factors | Smoking, hypertension, diabetes mellitus, hyperlipidemia, obesity, advanced age, and male gender are significant risk factors. |
Symptoms | Stable angina (exertional chest pain), shortness of breath, and decreased exercise capacity may occur. In some patients, symptoms may be mild or absent due to well-developed collateral circulation. |
Collateral Circulation | In long-standing occlusion, collateral vessels developing from neighboring arteries partially supply blood to the heart muscle. This may reduce the severity of symptoms but does not provide complete protection. |
Diagnostic Methods | Coronary angiography is the gold standard for diagnosis. In addition, CT coronary angiography, stress tests, and myocardial perfusion imaging methods may be used. |
Angiographic Features | Complete occlusion, TIMI 0 flow, and marked fibrosis and calcification in the occluded segment are typical. Proximal and distal cap structures affect procedural success. |
Treatment Options | Medical therapy (antianginal drugs, antiplatelets, statins), percutaneous coronary intervention (PCI), and in suitable patients, coronary artery bypass grafting (CABG) may be performed. |
PCI Characteristics | CTO-PCI is technically a complex procedure. Special guidewires, microcatheters, and advanced techniques (antegrade, retrograde approaches) are used. |
Treatment Goals | The goals are to reduce symptoms, improve quality of life, preserve myocardial viability, and in some patients, improve left ventricular function. |
Possible Complications | Perforation, dissection, contrast nephropathy, arrhythmia, and rarely myocardial infarction may occur. |
Prognosis | Successful revascularization may reduce symptoms and increase functional capacity. However, prognosis depends on concomitant vascular disease, left ventricular function, and the patient’s overall risk profile. |
Follow-Up | Regular cardiology follow-up, aggressive management of risk factors (blood pressure, lipid, glycemic control), lifestyle modifications, and continuation of medical therapy are required. |

Prof. Dr. Kadriye Kılıçkesmez
Cardiology, Interventional Cardiologist – Interventional Cardiologist
Prof. Dr. Kadriye Orta Kılıçkesmez is one of the leading names in the field of Turkish cardiology. She was born on January 24, 1974, in Tekirdağ. After completing her undergraduate education at Istanbul University Cerrahpaşa Faculty of Medicine, she chose cardiology as her specialty and received her specialist training at the Cardiology Institute of the same university.
After working for a short period at Çorlu State Hospital and Turkish Kidney Foundation Service Hospital, she returned to the I.U. Cardiology Institute. Continuing her academic career there, Kadriye Kılıçkesmez became an associate professor in 2012. She then worked at Royal Brompton on complex coronary interventions, CTO intracoronary imaging, and structural heart diseases, and wrote scientific articles. In 2015, she was appointed by the university to establish the Şişli Etfal cardiology clinic and Angio laboratory. Becoming a professor in 2017, Kadriye Kılıçkesmez established the cardiology clinic and Angio laboratory of Prof. Dr. Cemil Taşçıoğlu Hospital in 2020 and ensured that the clinic became a training clinic.
View MoreWhat Is Chronic Total Occlusion (Cto)?
Chronic total occlusion (CTO) is the condition in which a coronary artery has been completely blocked for at least three months. It usually develops as a result of atherosclerosis and may cause chest pain (angina) and shortness of breath by reducing blood flow to the heart muscle. Diagnosis is made by coronary angiography. Treatment options include medical therapy, percutaneous coronary intervention, or surgical revascularization in suitable patients. Early evaluation is important in preventing cardiac complications.
Causes and Risk Factors of CTO
Multiple factors play a role in the development of CTO. The most common cause is the process called atherosclerosis, in which fatty plaques accumulate on the vessel walls. These plaques grow over time, narrow the vessel, and may eventually cause complete blockage. The main factors that accelerate the development of CTO or increase its risk include:
- Age: The risk of arterial hardening increases with advancing age.
- Genetic Predisposition: A family history of early heart disease.
- High Blood Pressure (Hypertension): Persistent excessive pressure applied to vessel walls.
- High Cholesterol (Hyperlipidemia): Especially elevated LDL (“bad”) cholesterol levels.
- Diabetes (Diabetes Mellitus): High blood sugar levels can damage vessels.
- Smoking: Smoking damages vessel walls and triggers plaque formation.
- Obesity: Excess weight negatively affects blood pressure and cholesterol levels.
- Sedentary Lifestyle: Lack of physical activity.
- Chronic Inflammation: Long-term inflammatory processes in the body.
The coexistence of these risk factors significantly increases the likelihood of developing CTO. In some cases, CTO may also develop in patients who previously underwent successful angioplasty or bypass surgery. This may occur due to re-occlusion of implanted stents over time or failure of bypass grafts.
CTO Symptoms: What Should Be Observed?
The symptoms of Chronic Total Occlusion may vary from person to person depending on the location and size of the blockage and how well the heart adapts to the condition. While some patients experience no obvious symptoms, others may face serious complaints. The most common symptoms include:
- Chest Pain (Angina Pectoris): This is the most common symptom. It occurs during situations when the heart muscle’s oxygen demand increases, such as physical activity, stress, or cold weather. The pain is usually felt in the center of the chest and may radiate to the arm, neck, jaw, or back. Angina typically subsides with rest.
- Shortness of Breath (Dyspnea): Especially during exertion or while lying down, it may be a sign that the heart cannot pump sufficient blood.
- Fatigue and Weakness: A general decrease in energy may occur due to inadequate oxygen delivery by the heart.
- Palpitations: Irregular or rapid heartbeats may be felt.
- Nausea and Sweating: Although rare, these symptoms may occur especially during a heart attack.
- Dizziness or Fainting: May occur when insufficient blood reaches the brain.
Chest pain that has been ongoing for a long time and increases with exertion is a serious warning sign and a cardiology specialist should be consulted. In some patients, collateral circulation may develop, providing alternative blood flow to the area supplied by the blocked artery. These collaterals may reduce the severity of symptoms but do not eliminate them completely. Therefore, even in the absence of symptoms, the presence of CTO carries a significant risk.
Chronic Total Occlusion (CTO) Diagnostic Methods
The diagnosis of CTO is made using the patient’s medical history, physical examination, and various cardiac imaging techniques. Accurate diagnosis is critical in determining the most appropriate treatment method.
- Medical History and Physical Examination
The cardiologist thoroughly questions the patient’s complaints, family history, lifestyle, and existing health problems. The characteristics, duration, triggering factors, and relieving elements of chest pain are evaluated. During physical examination, blood pressure, pulse, and heart and lung sounds are assessed. This initial evaluation may strengthen suspicion of CTO and guide further testing.
- Electrocardiography (ECG)
ECG is a simple and painless test that records the electrical activity of the heart. In CTO, nonspecific changes may often be seen on ECG. However, it can help evaluate damage to the heart muscle or overall cardiac health. Even if resting ECG is normal, tests such as exercise ECG or Holter monitoring may reveal signs of ischemia during exertion.
- Echocardiography (ECHO)
ECHO is a method that uses ultrasound images to evaluate the structure, size, and function of the heart. In the presence of CTO, areas of the heart with reduced or absent blood flow (wall motion abnormalities) can be detected with ECHO. It also provides information about the overall pumping function of the heart (ejection fraction).
- Stress Tests (Exercise ECG, Scintigraphy, Stress ECHO)
These tests evaluate the heart’s performance under physical stress. While the patient walks or runs at a certain pace (exercise ECG) or the heart rate is increased with medication, ECG, myocardial scintigraphy, or echocardiography are used to monitor blood flow to the heart muscle and wall motion. In the presence of CTO, signs of ischemia (ECG changes, decreased blood flow, impaired wall motion) may appear during or after exertion. These tests are important in determining disease severity and exercise capacity.
- Coronary Angiography (Cardiac Catheterization)
Coronary angiography is considered the gold standard in the diagnosis of CTO. In this invasive method, a thin catheter (plastic tube) inserted through the groin or arm is advanced to the aortic root and then to the coronary arteries. Through this catheter, contrast material (a special dye visible on X-rays) is injected into the coronary arteries. X-ray images (fluoroscopy) taken during contrast injection clearly show the internal structure of the coronary arteries, the location, length, severity of blockages, and the overall condition of the vessel. The presence, length, typical features (for example, blunt stump, calcification), and possible collateral circulation pathways of CTO are definitively determined by angiography. This information is vital for treatment planning.
- Computed Tomography Angiography (CT Angio) and Magnetic Resonance Angiography (MR Angio)
CT angiography and MR angiography are non-invasive imaging methods used to evaluate coronary arteries. CT angiography provides high-resolution cross-sectional images, while MR angiography does not involve radiation and may provide additional information about the vessel wall. These methods may be used especially in patients unsuitable for angiography or to obtain preliminary information about the blockage. However, coronary angiography is used to evaluate the complex structure and treatability of CTO, while CT Angio may also be used to complement it.
Chronic Total Occlusion (CTO) Treatment: Modern Approaches
Although CTO treatment has traditionally been quite challenging, success rates have significantly increased in recent years thanks to advanced technologies and techniques. The primary goal of treatment is to restore blood flow to the heart by reopening the blocked artery, thereby relieving symptoms, improving quality of life, and reducing the risk of future cardiac events.
CTO Treatment with Percutaneous Coronary Intervention (PCI)
PCI is the most commonly used method in the treatment of CTO. This procedure is performed in a coronary angiography laboratory, usually under local anesthesia. The procedure generally includes the following steps:
- Preparation of the Access Site: A thin sheath is placed into two vessels, usually in the groin (femoral artery) or wrist (radial artery).
- Catheter Placement: Specially designed guidewires and catheters are used to reach the blocked artery.
- Crossing the Occlusion (Antegrade and Retrograde Approaches): The most challenging stage of CTO treatment is crossing the blocked segment by advancing from the beginning of the occluded artery (antegrade) or by progressing through alternative vessels in a reverse manner (retrograde). At this stage, specially designed guidewires, microcatheters, and advanced imaging techniques (IVUS, OCT) are used.
Antegrade Approach: Advancement is attempted from the proximal end of the occlusion. This is the most commonly used method. Retrograde Approach: The blocked artery is accessed in reverse, usually via another coronary artery or an internal mammary artery graft. This method is preferred when the antegrade approach fails or is very challenging.
- Balloon Angioplasty: After crossing the occlusion, a balloon catheter is placed in the blocked area and inflated to widen the vessel.
- Stent Placement: To prevent re-narrowing of the vessel, drug-eluting stents (DES) are usually placed in the blocked segment and expanded with a balloon to fix them to the vessel wall.
- Control Angiography: At the end of the procedure, it is checked whether the vessel is open and whether blood flow is sufficient.
Special Technologies Used in CTO PCI:
- Microcatheters: Very thin and flexible catheters that allow advancement in areas where the guidewire cannot progress.
- Imaging Technologies (IVUS and OCT): Intravascular Ultrasound (IVUS) and Optical Coherence Tomography (OCT) play a critical role in evaluating the internal structure of the vessel, the character of the occlusion, plaque composition, and the accuracy of stent placement.
- Rotational Atherectomy (Rotablator): Used in very hard and calcified lesions to thin the vessel and facilitate balloon and stent placement.
Bypass Surgery (CABG)
In some CTO cases, especially when there are severe blockages in multiple vessels or when stent placement is not feasible or is risky, coronary artery bypass grafting (CABG) may be a more appropriate treatment option. In this surgical method, vessel segments taken from another part of the body (usually a leg vein or chest artery) are sutured above the healthy part of the blocked coronary artery and below the blockage to create a new pathway for blood flow. In CTO treatment, bypass surgery may be preferred especially in patients with left main coronary artery occlusion or widespread vascular disease.
Medication Therapy and Lifestyle Changes
After both treatment methods (PCI and CABG), or in patients in whom other treatment methods have failed, lifelong medication therapy is required. These medications include blood thinners (antiplatelets), cholesterol-lowering agents (statins), blood pressure regulators, and beta-blockers. In addition, lifestyle changes such as quitting smoking, healthy nutrition, regular exercise, and weight control are vital to stop disease progression and protect overall cardiovascular health.
Success Rates and Challenges in CTO Treatment
Chronic Total Occlusion treatment, especially Percutaneous Coronary Intervention (PCI), has made significant progress in recent years. However, there are still certain challenges and factors affecting success rates.
Current Success Rates
Success rates in CTO interventions performed by specialized teams in experienced centers are quite high. Success is generally defined as complete reopening of the blocked artery and restoration of adequate blood flow. According to current literature, CTO PCI success rates in experienced centers are reported to be between 80–95%. These rates are directly related to advanced techniques used, equipment quality, and the physician’s experience. After a successful intervention, chest pain symptoms decrease or disappear completely in the majority of patients, exercise capacity increases, and quality of life improves.
Challenges Encountered in CTO Treatment
Due to the nature of CTO lesions, treatment is highly complex and involves various challenges:
- Length and Structure of the Occlusion: CTO lesions are often long (more than 30 mm) and may have a hard, calcified, or fibrotic structure. This makes advancement with guidewires difficult.
- Blunt Stump Formation: Long-standing occlusions may create a blunt proximal cap. This blunt end may prevent the guidewire from advancing in the correct direction.
- Calcification: Dense calcification in the vessel wall makes guidewire passage more difficult and may prevent full expansion of balloons and stents.
- Collateral Circulation: Alternative vessels (collaterals) used to cross the occlusion may sometimes be very small or tortuous, making retrograde techniques more challenging.
- Bifurcation Points: If the occlusion is located at a major vessel branching point, the risk of post-procedural thrombosis may increase.
- Impact of Previous Interventions: The condition of previously placed stents or bypass grafts may affect the new intervention.
The Importance of Expertise and Experience
CTO treatment requires greater expertise and experience compared to standard angiography procedures. Experienced cardiologists in this field increase success rates and minimize complication risks by effectively using specialized techniques and equipment. Therefore, patient selection and the experience of the center where the procedure will be performed are of great importance in CTO treatment.
Post-Treatment Care and Follow-Up in Chronic Total Occlusion (CTO)
After successful CTO treatment, a comprehensive follow-up program is implemented to support the patient’s recovery process and prevent future cardiac events.
Medication Therapy and Side Effects
After PCI, patients are usually started on dual antiplatelet therapy (for example, aspirin and clopidogrel/ticagrelor/prasugrel). These medications are critical in preventing clot formation within the stent (stent thrombosis) and are generally used for at least 12 months. In addition, medications such as statins (cholesterol-lowering), beta-blockers, and ACE inhibitors are prescribed according to the patient’s condition. Patients should be informed about possible side effects of these medications (bleeding risk, muscle pain, cough, etc.) and should be followed with regular physician check-ups.
Lifestyle Changes
Lifestyle changes are indispensable for lasting treatment success:
- Smoking Cessation: Smoking is one of the greatest threats to vascular health. It must be completely stopped.
- Healthy Nutrition: A low-fat, low-salt Mediterranean diet rich in vegetables and fruits is recommended.
- Regular Exercise: Regular aerobic exercise (walking, swimming, etc.) should be performed as recommended by the physician.
- Weight Control: Maintaining ideal body weight is important.
- Stress Management: Techniques for coping with stress (yoga, meditation, etc.) should be learned.
Regular Check-Ups and Imaging
It is recommended that the patient be regularly followed in cardiology outpatient clinics during the first few months after treatment. During these visits, symptoms, medication adherence, and overall health status are evaluated. If necessary, tests such as ECG, ECHO, or stress tests may be repeated. Since the risk of in-stent restenosis (re-narrowing) or thrombosis is higher especially within the first year, careful follow-up is essential. In the long term, cardiovascular health continues to be monitored with check-ups performed every 6 months or annually depending on the patient’s condition.
Complications and Their Management
As with any invasive procedure, certain risks and complications exist in CTO treatment. These may include vessel rupture during or after the procedure, bleeding, infection, stroke, heart attack, arrhythmia, and stent thrombosis. However, thanks to advanced technology and experienced teams, the incidence of these complications is quite low (around 1–2%). In patients who develop complications, successful outcomes are generally achieved with early diagnosis and appropriate intervention. For example, in patients who develop stent thrombosis, emergency angiography and stent replacement may be required.
Frequently Asked Questions
Chronic Total Occlusion generally occurs as a result of progressive atherosclerosis in the vessel wall. Over time, the plaque hardens and completely blocks the vessel lumen. Clot formation and long-standing narrowing may also lead to total occlusion.
Chronic Total Occlusion is more common in individuals with diabetes, hypertension, smoking, and high cholesterol. The risk increases significantly in patients who have previously had a heart attack or have widespread vascular disease.
Chronic Total Occlusion interrupts blood flow to the heart muscle, causing oxygen deficiency. Over time, the heart muscle may weaken, its contractile strength may decrease, and the risk of heart failure may arise.
Because Chronic Total Occlusion develops slowly, the body may form collateral vessels. This collateral circulation partially compensates for blood flow and chest pain may be milder or intermittent in some patients.
If left untreated, Chronic Total Occlusion may lead to progressive chest pain, heart failure, and rhythm disorders. In the long term, the risk of heart attack and sudden cardiac death may increase.
Chronic Total Occlusion can be opened with angioplasty using special guidewires and advanced techniques. During the procedure, a balloon and stent are placed to restore blood flow in the vessel.
In some patients, Chronic Total Occlusion may require bypass surgery. Especially if multiple vessels are blocked or angioplasty has failed, surgical options are evaluated.
The recovery process after Chronic Total Occlusion treatment depends on the method applied. While patients can return to daily life within a few days after angioplasty, recovery after bypass surgery may take weeks.
Chronic Total Occlusion may reduce quality of life with chest pain and decreased exercise capacity. After successful treatment, shortness of breath decreases and physical endurance improves in most patients.
Chronic Total Occlusion may rarely recur after treatment. Re-narrowing within the stent or new plaque formation in other vessels may occur. Regular follow-up and management of risk factors are important.